Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
Stroke is India’s second leading cause of death and the leading cause of adult disability — yet it is one of the most time-sensitive emergencies in medicine where minutes literally equal brain tissue. India registers approximately 1.8 million new strokes every year, with a stroke occurring every 20 seconds. The tragedy: most Indian stroke patients arrive at hospital 12–24 hours after onset — missing the 4.5-hour thrombolysis (clot-busting) window that could restore function and save lives. A stroke destroys 1.9 million neurons every minute it is untreated. The FAST acronym — Face drooping, Arm weakness, Speech slurred, Time to call emergency — is the single most important public health message that India needs. Knowing FAST could save a family member’s life.
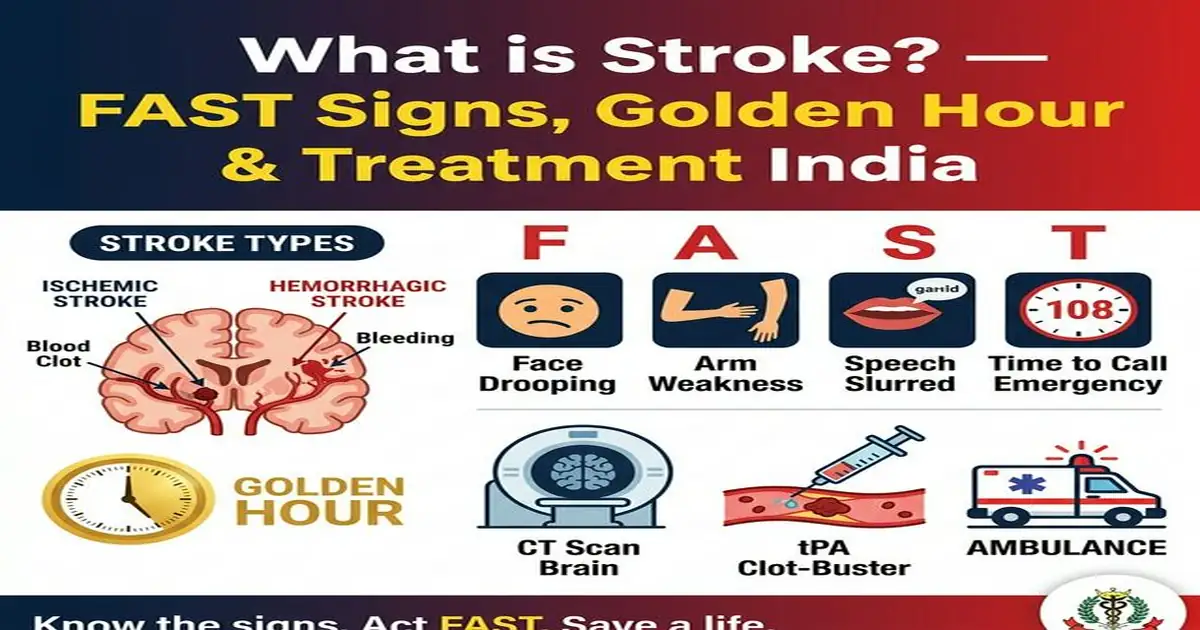
What is a Stroke? — Ischemic vs Hemorrhagic
| Feature | Ischemic Stroke (85%) | Hemorrhagic Stroke (15%) |
|---|---|---|
| Mechanism | Blood clot blocks artery supplying brain → brain tissue dies from lack of oxygen | Blood vessel bursts → blood floods brain tissue → compression + toxic blood damages neurons |
| Causes | Atrial fibrillation (heart clot), carotid artery atherosclerosis, small vessel disease (hypertension/diabetes), cardioembolism | Uncontrolled hypertension (most common in India), ruptured aneurysm, AVM, anticoagulant excess |
| CT scan appearance | Early CT normal (<6 hours); later shows dark (hypodense) infarcted area; MRI DWI shows within 30 minutes | Bright (hyperdense) blood visible immediately on CT — no waiting |
| Treatment | IV tPA (thrombolysis) within 4.5 hours; mechanical thrombectomy (clot removal) within 6–24 hours | Blood pressure control; surgical evacuation for large bleeds; NO tPA (would worsen bleeding) |
| India proportion | ~75–80% of all Indian strokes | ~20–25% — higher than Western countries due to hypertension prevalence and poor BP control |
🚨 FAST — Recognise Stroke in 60 Seconds
| Letter | Sign | How to Check |
|---|---|---|
| F — Face | Face drooping or uneven smile | Ask person to smile — does one side droop? Is the face asymmetrical? |
| A — Arms | Arm weakness — one arm drifts down | Ask to raise both arms — does one drift down involuntarily? |
| S — Speech | Speech slurred, confused, or unable to speak | Ask to repeat “The sky is blue” — is speech garbled, wrong words, or absent? |
| T — Time | Time to call emergency immediately | Note the EXACT TIME symptoms started. Call 108 immediately. Do not drive yourself. Do not wait to see if it improves. |
🧠 Additional FAST signs: sudden severe headache “worst of life” (subarachnoid haemorrhage); sudden vision loss in one eye or double vision; sudden loss of balance/coordination; sudden confusion. ANY sudden neurological symptom = potential stroke = emergency.
The Golden Hour — Why Every Minute Counts
In ischemic stroke, brain tissue is dying at a rate of 1.9 million neurons, 13.8 billion synapses, and 12 km of myelinated nerve fibres per minute. The “Time is Brain” concept quantifies this: for every 1-hour delay in recanalisation (restoring blood flow), the equivalent of 3.6 years of normal brain ageing is lost. Treatment windows:
- ⏰ 0–4.5 hours: IV tPA (alteplase/tenecteplase) thrombolysis — dissolves the clot chemically; restores blood flow in 30–40% of cases; improves functional outcome at 3 months by 30%; available at all certified stroke centres
- ⏰ 0–6 hours (up to 24 hours in selected patients): Mechanical thrombectomy — interventional radiologist passes catheter from groin artery to brain, physically removes clot with stent retriever; 60–70%+ recanalisation rate; dramatic recovery possible; available at comprehensive stroke centres (AIIMS, major private hospitals)
- ⏰ >4.5 hours: tPA not effective; thrombectomy still possible for large vessel occlusions within window; supportive care, BP management, aspirin
Risk Factors for Stroke in India
| Risk Factor | Stroke Risk Increase | India Context |
|---|---|---|
| Hypertension | 4–5× increased risk; accounts for 54% of stroke burden globally | Most important modifiable risk factor in India; 1 in 4 Indians hypertensive; BP control below 130/80 is the most impactful stroke prevention |
| Atrial Fibrillation (AF) | 5× increased risk; responsible for 20–25% of ischemic strokes | AF stroke is the most devastating (large vessel occlusion); anticoagulation (warfarin or NOAC) prevents 65% of AF-related strokes; many AF patients in India not anticoagulated |
| Diabetes | 2–3× increased risk; accelerates cerebrovascular atherosclerosis | India’s 100M+ diabetics are at significant stroke risk; HbA1c <7 reduces cerebrovascular events |
| Smoking | 2× increased risk; bidi smoking particularly harmful | Male stroke patients in India — smoking is present in 60–70%; bidi smokers have higher stroke risk due to unfiltered smoke |
| High cholesterol / LDL | Atherosclerotic plaque → carotid stenosis → embolic stroke | Statin therapy targets LDL <70 mg/dL for secondary stroke prevention |
| Young stroke (age <45) | India-specific concern — 20–30% of Indian strokes in people under 45 years | Causes: cardioembolism (rheumatic heart disease, CIED), hypercoagulability, vasculitis, substance abuse, migraine with aura; requires different investigation (TEE, thrombophilia screen) |
Stroke Rehabilitation — Recovery After Stroke
The brain has remarkable capacity for recovery through neuroplasticity — the ability of surviving neurons to form new connections and compensate for damaged areas. Recovery is most rapid in the first 3–6 months and continues more slowly for 1–2 years. Rehabilitation components: Physiotherapy — restores motor function, gait, and coordination; started within 24–48 hours even in ICU. Speech therapy — for aphasia (language problems) and dysphagia (swallowing difficulty — present in 50% of acute strokes). Occupational therapy — restores ability to perform daily activities (dressing, cooking, writing). Cognitive rehabilitation — for post-stroke cognitive impairment (present in 30–50% at 3 months). Psychological support — post-stroke depression affects 30–40% of survivors; untreated depression dramatically worsens rehabilitation outcomes. In India, comprehensive inpatient rehabilitation is available at NIMHANS, AIIMS, and major facilities; most patients receive outpatient physiotherapy. Government Ayushman Bharat covers stroke rehabilitation at empanelled centres.
Frequently Asked Questions
What should I do if someone is having a stroke right now?
This is the most important question in stroke medicine — and the correct response saves lives. Immediately: Note the exact time symptoms started — this single data point determines treatment eligibility (tPA requires onset within 4.5 hours). Call 108 (national ambulance) immediately — do not drive the person yourself (ambulance can alert the hospital, begin assessment en route, and get patient to CT faster). Tell the 108 operator “I think this is a stroke” — this triggers a stroke alert at the receiving hospital. What NOT to do: Do not give aspirin immediately — aspirating in an unresponsive patient is dangerous; and if the stroke is hemorrhagic, aspirin worsens bleeding. Do not give food or water — 50% of acute stroke patients have swallowing problems; aspiration pneumonia is a leading cause of stroke death. Do not wait to see if symptoms improve — a TIA (transient ischaemic attack) that resolves completely is a warning of impending major stroke (10% risk of stroke in next 48 hours); still requires emergency evaluation. Do not look for “home remedies” or call a family doctor first — every minute of delay reduces treatment effectiveness by 1.8 million neurons. At hospital: Insist on CT scan immediately (within 25 minutes of arrival is the target). If CT shows no bleeding, ask about tPA eligibility. Ask for a neurologist if not immediately called. Time to treatment from hospital arrival should be <60 minutes at certified stroke centres. If the hospital cannot provide thrombolysis, ask for immediate transfer to a stroke centre — “drip and ship” (tPA at first hospital + transfer for thrombectomy) is an accepted protocol.
Can a stroke be predicted or prevented?
Yes — approximately 90% of strokes are preventable through addressing modifiable risk factors. The INTERSTROKE study (including large Indian cohort) identified 10 risk factors accounting for 90% of global stroke risk: hypertension (most important — 35% attributable risk), smoking, abdominal obesity, diet, physical inactivity, diabetes, alcohol, cardiac causes, dyslipidaemia, and psychological stress. Prevention protocol: Blood pressure below 130/80 mmHg — the single most impactful intervention; every 10 mmHg reduction in systolic BP reduces stroke risk by 22%. Take antihypertensive medication consistently — BP control alone could prevent 1 in 3 Indian strokes. LDL cholesterol below 70 mg/dL for high-risk individuals — statin therapy (atorvastatin/rosuvastatin) reduces stroke risk by 20–25%. Atrial fibrillation anticoagulation — warfarin (INR 2–3) or NOACs (apixaban, dabigatran, rivaroxaban) reduce AF stroke risk by 65%. Antiplatelet therapy (aspirin + clopidogrel short-term for high-risk TIA, then aspirin or clopidogrel alone) for secondary prevention. Smoking cessation — risk returns to non-smoker levels within 5 years. Warning sign — TIA: A TIA (transient ischaemic attack) — stroke symptoms resolving within 24 hours — is the most important stroke warning. The ABCD2 score (Age, BP, Clinical features, Duration, Diabetes) identifies high-risk TIA patients who need immediate hospitalisation. Up to 10% of TIA patients will have a major stroke within 48 hours without treatment. Never dismiss TIA as “just a dizzy spell.”
Why do young Indians get strokes?
India has a disproportionately high burden of stroke in young adults (age 18–45) — accounting for 20–30% of all Indian strokes, compared to 10–15% in Western countries. This is a uniquely important public health issue because young stroke causes decades of productive life lost and enormous family impact. Causes of young stroke in India: Rheumatic heart disease — damaged heart valves from untreated streptococcal fever form clots that embolise to the brain; mitral stenosis is the classic cause; India has the highest rheumatic heart disease burden globally due to inadequate primary antibiotic coverage of streptococcal throat infections. Antiphospholipid syndrome — autoimmune hypercoagulability; particularly affects young women; associated with recurrent pregnancy loss; requires anticoagulation. Cerebral venous sinus thrombosis (CVST) — clotting of the cerebral veins rather than arteries; more common in India (dehydration, post-partum state, OCP use, infection, hypercoagulability); presents with headache, seizures, focal deficits; treated with anticoagulation (NOT clot-busting). Drug abuse — cocaine, amphetamine, and increasingly methamphetamine cause vasospasm and hemorrhagic stroke; rising in urban India. Migraine with aura — modestly increases ischemic stroke risk; particularly in women on OCPs who smoke — the triple combination is particularly hazardous. Uncontrolled hypertension in pregnancy — eclampsia causes hemorrhagic and ischemic stroke; young women post-partum are vulnerable. Investigation of young stroke: full echo (cardioembolism), thrombophilia screen (Factor V Leiden, protein C/S, APLA), MRA intracranial vessels, HIV, CSF analysis — distinct from the elderly stroke workup.
What is recovery like after a stroke?
Stroke recovery is one of the most variable outcomes in medicine — ranging from complete recovery to permanent severe disability — and the trajectory is shaped by stroke severity, location, time to treatment, and quality of rehabilitation. Factors predicting better recovery: Smaller stroke volume (less brain tissue destroyed); successful recanalisation with tPA or thrombectomy; younger age (more neuroplasticity); early and intensive rehabilitation (starting within 24–48 hours); absence of post-stroke depression; good social support and caregiver engagement; pre-stroke baseline health. Recovery timeline: First 3 months — most rapid recovery phase; maximum neuroplasticity; intensive rehabilitation critical in this window. 3–12 months — continued but slower improvement; function gains continue with persistent rehabilitation. Beyond 12 months — further improvement possible but slower; constraint-induced movement therapy, robot-assisted rehabilitation, and brain stimulation techniques may augment recovery. Common residual deficits in Indian context: Hemiplegia (one-sided weakness) — most common; physiotherapy can restore walking in 60–80% of patients with hemisphere strokes. Aphasia (language problems) — most distressing for patients and families; speech therapy can significantly improve communication over 2+ years. Post-stroke cognitive impairment — affects 30–50%; vascular dementia may develop in recurrent stroke. Realistic expectation-setting: A large middle cerebral artery stroke causing dense hemiplegia and aphasia has a very different prognosis from a small lacunar stroke causing only hand weakness. Both benefit from rehabilitation — but honest discussion of likely functional outcomes allows families to plan care appropriately. Post-stroke depression is treatable (sertraline, escitalopram) and its treatment significantly improves rehabilitation outcomes — this crossover of physical and mental health is critical in stroke care.
Is there a difference between a stroke and a brain haemorrhage?
“Brain haemorrhage” and “stroke” are related but not synonymous terms that cause significant confusion for patients and families. Stroke is the umbrella term for any sudden neurological deficit caused by cerebrovascular disease. It includes both ischemic stroke (87%) and hemorrhagic stroke (13%). Hemorrhagic stroke is a type of stroke caused by bleeding — either intracerebral haemorrhage (ICH — bleeding within the brain parenchyma) or subarachnoid haemorrhage (SAH — bleeding into the space around the brain from a ruptured aneurysm). Intracerebral haemorrhage (ICH): Most commonly caused by hypertension-induced rupture of small penetrating arteries (lenticulostriate arteries); basal ganglia is the most common location; presents identically to ischemic stroke clinically — CT scan distinguishes (bright blood vs dark/normal infarct). ICH is NOT treated with tPA — it is treated with urgent blood pressure control (systolic <140 mmHg), reversal of any anticoagulation, and large haematomas may need surgical evacuation. Prognosis depends on haematoma volume and location. Subarachnoid haemorrhage (SAH): Classic presentation is “thunderclap headache” — the worst headache of life, sudden onset, maximal at onset; caused by ruptured cerebral aneurysm in 75% of cases. SAH is a neurosurgical emergency — CTA to find aneurysm + coiling or clipping. Mortality even with treatment 30–40%. This distinction matters critically because the treatment of ischemic stroke (tPA, anticoagulation) is directly harmful in hemorrhagic stroke — which is why CT scan before any treatment is absolutely mandatory.
What to Read Next
- High Blood Pressure — Hypertension Causes 54% of Global Stroke Burden
- Diabetes — Diabetes Doubles Stroke Risk Through Cerebrovascular Atherosclerosis
- Cholesterol — LDL Causes Carotid Plaques That Embolise to Brain
- Heart Attack — AF After MI is a Major Source of Cardioembolic Stroke
- Depression — Post-stroke Depression Affects 40% of Survivors and Worsens Recovery
Every year, 1.8 million Indian families go through the terror of watching a loved one collapse with a stroke. Most of them do not know that a treatment existed — if only they had arrived within 4.5 hours. The FAST acronym takes 10 seconds to learn. It could give back 10 years of life.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on Indian Stroke Association guidelines, INTERSTROKE study, and AHA/ASA Stroke Guidelines 2023. Last updated: March 2026.
Emergency: If stroke symptoms — call 108 immediately. Note the time. Every minute counts.
Authoritative Sources: Indian Stroke Association | American Stroke Association | WHO — Stroke | ICMR India
🚨 Stroke Emergency: If you see FAST signs — Face drooping, Arm weakness, Speech slurred — call 108 immediately. Note the exact time. Do NOT wait. Do NOT drive yourself. Every minute of delay destroys 1.9 million brain neurons.
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Stroke is a medical emergency requiring immediate hospital care. Never attempt home treatment. Never take aspirin without emergency medical instruction in acute stroke.
