Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
Asthma is the most common chronic respiratory disease in India — affecting an estimated 30–35 million Indians and causing over 100,000 deaths annually. Despite being one of the most treatable chronic diseases in medicine, asthma is massively undertreated in India due to fear of inhalers (“addiction” myths), poor access to diagnosis, and lack of awareness about the difference between a reliever and a preventer. A person with well-controlled asthma can live a completely normal life — run marathons, work in physically demanding jobs, and never experience a single attack. Getting there requires correct diagnosis, the right inhalers, and understanding your triggers.
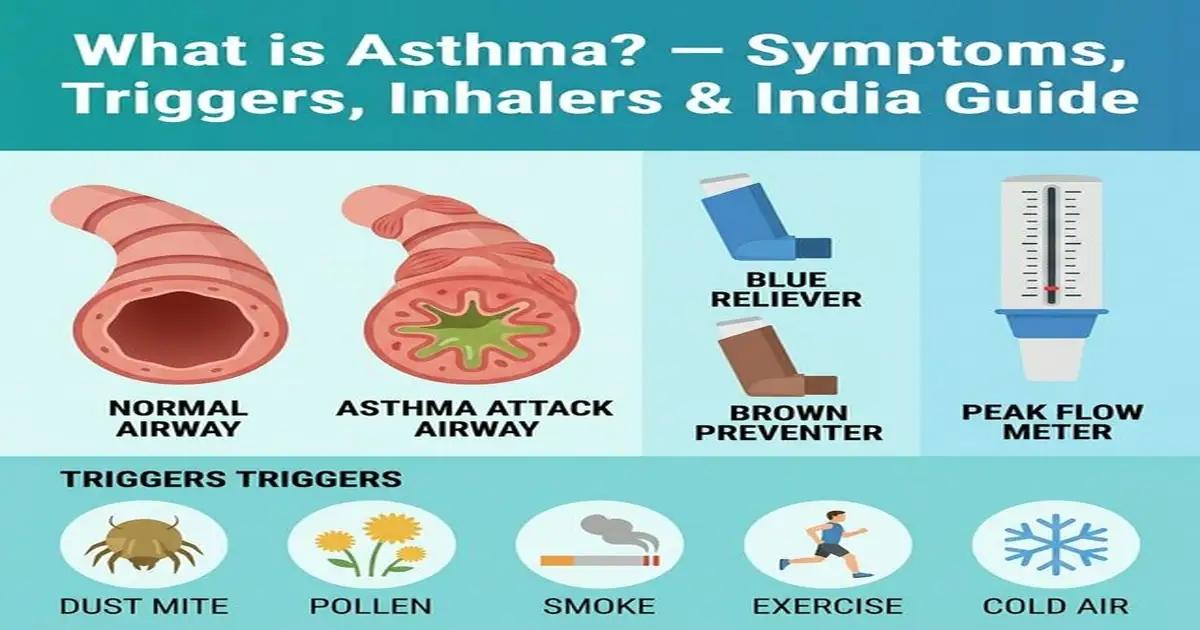
What is Asthma? — What Happens in the Airways
Asthma is a chronic inflammatory disease of the airways (bronchi and bronchioles) characterised by three simultaneous changes: (1) Inflammation — the airway lining becomes swollen and irritated, narrowing the internal passage; (2) Bronchoconstriction — the muscles surrounding the airways tighten and constrict (bronchospasm), further reducing diameter; (3) Mucus hypersecretion — excess thick mucus is produced, further blocking airflow. The result: breathlessness, wheezing, chest tightness, and coughing — particularly at night or early morning. Asthma is also characterised by reversibility — unlike COPD, the airway narrowing in asthma is largely reversible with treatment (bronchodilators), which is a key diagnostic feature. The inflammation in asthma is usually eosinophilic (allergy-type, triggered by allergens and irritants) or non-eosinophilic (non-allergic, triggered by exercise, cold air, infections).
Types of Asthma
| Type | Trigger Pattern | Age of Onset | Indian Relevance |
|---|---|---|---|
| Allergic (Atopic) Asthma | Allergens: dust mites, pet dander, pollen, cockroach, mold | Usually childhood | Most common type; dust mites in humid Indian homes; cockroach allergy very high in Indian urban chawls/slums |
| Non-allergic Asthma | Cold air, exercise, smoke, strong smells, viral infection, stress | Any age; often adult onset | Significant — Diwali fire smoke, kitchen smoke (chulha), crop burning, winter Delhi air |
| Exercise-Induced Bronchoconstriction (EIB) | Vigorous exercise, especially in cold/dry air | Adolescents/young adults | Athletes; PE teachers; outdoor workers in North India winter |
| Occupational Asthma | Workplace exposures: flour dust (bakers), isocyanates, latex, chemical fumes | Working age adults | Construction workers, bakers, healthcare workers |
| Cough-Variant Asthma | Chronic dry cough WITHOUT classic wheeze/breathlessness — the “hidden” asthma | Any age | Very frequently misdiagnosed as chronic bronchitis or GERD in India |
| Severe Asthma | Poorly controlled despite high-dose inhalers; frequent attacks; may have neutrophilic or mixed inflammation | Any | 5–10% of all asthma; requires specialist biologics (dupilumab, mepolizumab) |
Symptoms of Asthma — Complete List
| Symptom | Description | When Worst |
|---|---|---|
| Wheezing | High-pitched whistling sound when breathing out — produced by turbulent airflow through narrowed airways | During attacks; exercise; allergen exposure |
| Breathlessness (dyspnoea) | Difficulty breathing; feeling of not getting enough air; in severe attacks — unable to complete sentences | Attacks; night; early morning; exercise |
| Chest tightness | Feeling of pressure or constriction in the chest — like a band tightening | Often at night or on waking |
| Cough | Usually dry; often worse at night and early morning; can be the only symptom (cough-variant asthma) | Night and early morning; cold air; post-exercise |
| Nocturnal symptoms | Waking at night with any of the above — classic asthma feature; cortisol dips at 4 AM → airway inflammation peaks | 2–5 AM (worst asthma time) |
| Exercise limitation | Symptoms worsen with physical activity — children avoid PE; adults avoid exercise | During and 5–10 min after exercise |
| Prolonged cough after respiratory infection | A cold that “goes to the chest” and cough/wheeze persists for 3–4 weeks — strongly suggests asthma | Post-viral; especially winter |
Asthma Severity Classification — Indian GINA Guidelines
| Level | Daytime Symptoms | Nighttime Symptoms | FEV1 or PEF | Treatment Step |
|---|---|---|---|---|
| Intermittent | ≤2 days/week | ≤2 nights/month | ≥80% predicted | As-needed reliever only (SABA or low-dose ICS-formoterol) |
| Mild Persistent | >2 days/week but not daily | 3–4 nights/month | ≥80% | Low-dose ICS daily + as-needed reliever |
| Moderate Persistent | Daily symptoms | >1 night/week | 60–80% | Medium-dose ICS + LABA daily |
| Severe Persistent | Continuous symptoms; limited activity; frequent attacks | Frequent nighttime symptoms | <60% | High-dose ICS + LABA + add-on therapies; specialist review |
Inhalers — The Most Important Part of Asthma Treatment
| Inhaler Type | Examples (India) | Colour | Purpose | Use |
|---|---|---|---|---|
| SABA — Short-Acting Beta Agonist (Reliever) | Salbutamol (Asthalin, Ventorlin), Levosalbutamol (Levolin) | Usually Blue | Rapid bronchodilation in 5–10 minutes; relieves acute symptoms | Only when needed; NOT for daily regular use alone |
| ICS — Inhaled Corticosteroid (Preventer) | Budesonide (Budecort), Beclomethasone (Beclate), Fluticasone (Flohale) | Usually Brown/Red/Orange | Reduces airway inflammation; prevents attacks; cornerstone of asthma control | Daily, consistently — even when feeling well |
| LABA — Long-Acting Beta Agonist | Formoterol, Salmeterol (Seroflo = Fluticasone+Salmeterol, Symbicort = Budesonide+Formoterol) | Purple/Green | Long bronchodilation (12 hours); always combined with ICS | Daily — NEVER alone in asthma without ICS |
| LAMA — Long-Acting Muscarinic Antagonist | Tiotropium (Spiriva Respimat) | Grey | Add-on bronchodilation; most useful in COPD but used in severe asthma | Daily; add-on therapy |
| ICS + Formoterol (MART regimen) | Symbicort Turbuhaler, Duova DPI (Budesonide+Formoterol) | Purple/Red | Both preventer AND reliever in one device — GINA recommended first-line 2023 | Daily + as-needed — reduces oral steroid courses |
💨 The biggest Indian asthma myth — BUSTED: “Inhalers are addictive.” This is completely false and is the most dangerous medical myth in Indian respiratory health. Inhalers deliver medication directly to the lungs — 100× smaller dose than oral tablets — with minimal systemic absorption and no addiction mechanism whatsoever. The ICS in a preventer inhaler is not the same as anabolic steroids. Refusing inhalers and taking repeated courses of oral steroids (prednisolone) instead is far more harmful.
Common Asthma Triggers in India — and How to Avoid Them
| Trigger | Indian Context | Avoidance Strategy |
|---|---|---|
| House dust mites | Thrive in humid Indian homes, cotton mattresses, curtains — most common allergen trigger in India | Allergen-proof mattress covers; wash bedding in hot water weekly; reduce indoor humidity; remove carpets |
| Cockroach allergen | Extremely common in Indian urban housing; cockroach droppings are potent allergens | Rigorous pest control; seal food; clean kitchen surfaces; boric acid traps |
| Air pollution (outdoor) | Delhi AQI >300 routinely in winter; Diwali firecrackers; stubble burning; diesel vehicles | N95 mask outdoors on high-AQI days; stay indoors on worst days; purifier at home |
| Biomass cooking smoke | Chulha cooking (wood/cow dung) — massive particulate exposure; 600 million Indians still use solid fuels | LPG/electric transition; chimney/exhaust; cook outdoors when possible |
| Incense / agarbatti / dhoop | Daily religious use in most Indian homes — potent fine particulate source | Reduce use; ensure ventilation; asthmatics avoid direct exposure |
| Tobacco smoke (active + passive) | 267 million tobacco users; many children with asthmatic parents exposed to SHS | Complete cessation; never smoke indoors; no tobacco near children |
| GERD / acid reflux | Very common co-trigger in India; acid micro-aspiration triggers airway inflammation | Antacid treatment; avoid lying down after eating; elevate head of bed |
Frequently Asked Questions
Can asthma be cured permanently?
Asthma cannot currently be “cured” in the sense of permanent elimination — it is a chronic condition involving airway hyperresponsiveness that persists throughout life in most patients. However, two important qualifications change that picture significantly: First, childhood asthma “disappears” in 30–50% of cases by adolescence — symptoms remit as airways grow larger and immune responses mature. However, up to 30–50% of these children experience return of symptoms in adulthood, suggesting ongoing airway hyperresponsiveness rather than true cure. Second, well-controlled asthma is functionally equivalent to being cured — with correct treatment (ICS preventer + trigger avoidance), the majority of asthma patients can be completely symptom-free, exercise without restrictions, and have no night waking or attacks. The goal of asthma treatment is not cure but “control” — and full control is achievable for 70–80% of patients with current therapy. Emerging biologics (dupilumab, mepolizumab) targeting specific inflammation pathways are achieving near-remission in severe asthma. Allergen immunotherapy (desensitisation) — regular injections or sublingual drops of allergens — can produce lasting remission in allergic asthma by retraining the immune system, particularly when started in childhood.
Are inhalers safe for children and long-term use?
Yes — inhaled corticosteroids (ICS), which are the main preventer inhaler for asthma, are the safest and most effective long-term asthma treatment available, including for children. The critical context: ICS at the doses used in asthma (budesonide 200–400 mcg/day in a child) delivers a minute fraction of the systemic steroid dose compared to oral prednisolone. The systemic absorption from an ICS inhaler is approximately 1–10% — the rest acts locally in the lungs. Decades of paediatric studies confirm: ICS at standard doses does not cause adrenal suppression, growth retardation, osteoporosis, or immune impairment that are seen with oral steroids. The mild growth effect (<1cm in the first year, not cumulative) seen in some studies with very high-dose ICS is far less harmful than the growth impairment caused by poorly controlled, undertreated asthma itself (frequent oral steroid courses, sleep deprivation, poor oxygenation). Using a spacer device with MDI inhalers (a cylinder between inhaler and mouth) significantly reduces oropharyngeal deposition, minimises any local effects (oral thrush), and improves lung delivery — all children should use inhalers with a spacer. The bottom line: the harm of untreated asthma (attacks, steroid courses, hospitalisations, growth impairment from hypoxia) massively outweighs any risk from appropriate ICS use.
How do I use an inhaler correctly?
Incorrect inhaler technique is the most common cause of inadequately controlled asthma in India — studies show up to 70–80% of patients use their inhalers incorrectly, delivering minimal drug to the lungs. For a pressurised Metered Dose Inhaler (pMDI — the standard “pump” inhaler): (1) Shake well; (2) Breathe out fully; (3) Place mouthpiece between teeth, seal with lips; (4) Press the canister simultaneously as you begin a slow, deep breath IN — over 5 seconds — NOT a fast puff; (5) Hold breath for 10 seconds; (6) Breathe out slowly. For a Dry Powder Inhaler (DPI — Turbuhaler, Rotahaler, Revolizer): (1) Load the dose (twist, click, or open as per device); (2) Breathe out AWAY from the mouthpiece; (3) Place mouthpiece in mouth and breathe in as fast and deep as possible (DPIs require high inspiratory flow, unlike pMDI); (4) Hold for 10 seconds. Critical India-specific advice: always use a spacer with pMDI (Aerochamber, Volumatic) — improves drug delivery by 3–4× and makes technique much easier; rinse mouth after each ICS inhaler dose to prevent oral thrush; demonstrate technique at every follow-up appointment; watch GINA-endorsed video guides in Hindi on YouTube (search “inhaler use Hindi”).
What is the difference between asthma and COPD?
Asthma and COPD are both obstructive lung diseases causing breathlessness and wheeze — but they are fundamentally different in cause, reversibility, and treatment strategy. Asthma is primarily an allergic/inflammatory condition, typically beginning in childhood, with largely reversible airway obstruction (>12% improvement in FEV1 after bronchodilator) and normal lung function between attacks in most patients. COPD (Chronic Obstructive Pulmonary Disease) is primarily caused by cigarette smoking or biomass smoke exposure, typically diagnosed after age 40, with irreversible or partially reversible airway obstruction and progressive, permanent lung damage. Key differences: Asthma patients are often non-smokers (or mild smokers); COPD is almost always caused by decades of smoking or heavy smoke exposure. Asthma has normal CT scan between attacks; COPD shows emphysema (air trapping, bullae) and small airway thickening on CT. Asthma responds dramatically to ICS; ICS in COPD provides only modest benefit. Blood eosinophils are often elevated in asthma — and now used to guide biologic therapy. Where it gets complicated: “Asthma-COPD Overlap” (ACO) exists in 15–20% of obstructive lung disease patients — particularly ex-smokers with childhood asthma or long-term uncontrolled asthma with fixed obstruction. Spirometry is essential to distinguish: a bronchodilator reversibility test showing >12% and >200ml FEV1 increase confirms asthma; absent reversibility suggests COPD.
What is an asthma attack — and what to do in one?
An asthma attack (exacerbation) is a sudden, acute worsening of asthma symptoms — severe breathlessness, wheeze, and chest tightness that are not relieved by usual reliever inhaler use. Attacks range from mild (responds to 4 puffs salbutamol) to life-threatening (cannot speak in full sentences, oxygen saturation dropping). What to do in a mild-moderate attack: Sit upright (leaning forward on hands); use reliever (salbutamol Asthalin MDI) — 4 puffs one at a time with a spacer every 20 minutes for up to 3 doses; if improving after 1 hour → continue monitoring, double preventer dose for 1–2 weeks, and ring doctor. Warning signs requiring immediate 108/ER visit: Unable to complete a sentence in one breath; lips or fingernails turning blue (cyanosis); reliever not working after 3 doses; peak flow below 50% of personal best; confusion or exhaustion. Hospital treatment: Nebulised salbutamol + ipratropium; systemic steroids (prednisolone or IV hydrocortisone); oxygen; magnesium sulphate IV in severe cases; intubation in life-threatening cases. The most common trigger for severe attacks in India: stopping preventer inhaler when feeling well, combined with a viral respiratory infection (cold, flu, COVID). Every asthmatic should have a written Asthma Action Plan — a card specifying what to do based on symptom severity and peak flow readings.
What to Read Next
- What is Tuberculosis (TB)? — India Has the World’s Highest TB Burden
- What is COPD? — Chronic Lung Disease from Smoking & Biomass Smoke
- Vitamin D Deficiency — Low Vitamin D Worsens Asthma Control
- Thyroid Disease — Hypothyroidism Can Worsen Asthma Symptoms
- Fatty Liver — Metabolic Syndrome Linked to Severe Asthma Phenotype
Asthma with a preventer inhaler is like glasses for poor eyesight — you use them daily, and you see (breathe) normally. Without them, everything is blurred (breathless). The inhaler is not weakness — it is the tool that gives you your life back. Use it. Every day. Even on good days.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on GINA (Global Initiative for Asthma) Guidelines 2024, Indian Chest Society guidelines, and Indian asthma epidemiology data. Last updated: March 2026.
Authoritative Sources: GINA — Global Initiative for Asthma 2024 | Indian Chest Society | Mayo Clinic — Asthma | WHO — Asthma
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Asthma diagnosis requires spirometry or peak flow testing and clinical evaluation by a physician. Never stop prescribed inhalers without medical advice. Seek emergency care if an asthma attack does not respond to your reliever inhaler.
