Last Updated: March 2026 | Reading Time: 9 minutes | ~2,000 words
Food allergy is an immune-mediated adverse reaction to a specific food protein — distinct from food intolerance (non-immune), food poisoning (microbial), and food sensitivity. While historically considered a “Western” problem, India’s food allergy burden is rising rapidly with urbanisation — affecting an estimated 3–6% of Indian children and 1–2% of adults. More critically, anaphylaxis — the potentially fatal severe allergic reaction — is frequently mismanaged in India due to unfamiliarity with epinephrine auto-injectors, over-reliance on antihistamines and steroids (which are INSUFFICIENT for anaphylaxis), and inadequate emergency protocols. Every year, Indians die from anaphylaxis that could have been treated with timely intramuscular epinephrine. This guide provides the life-saving knowledge that every Indian family, school, and healthcare worker needs.
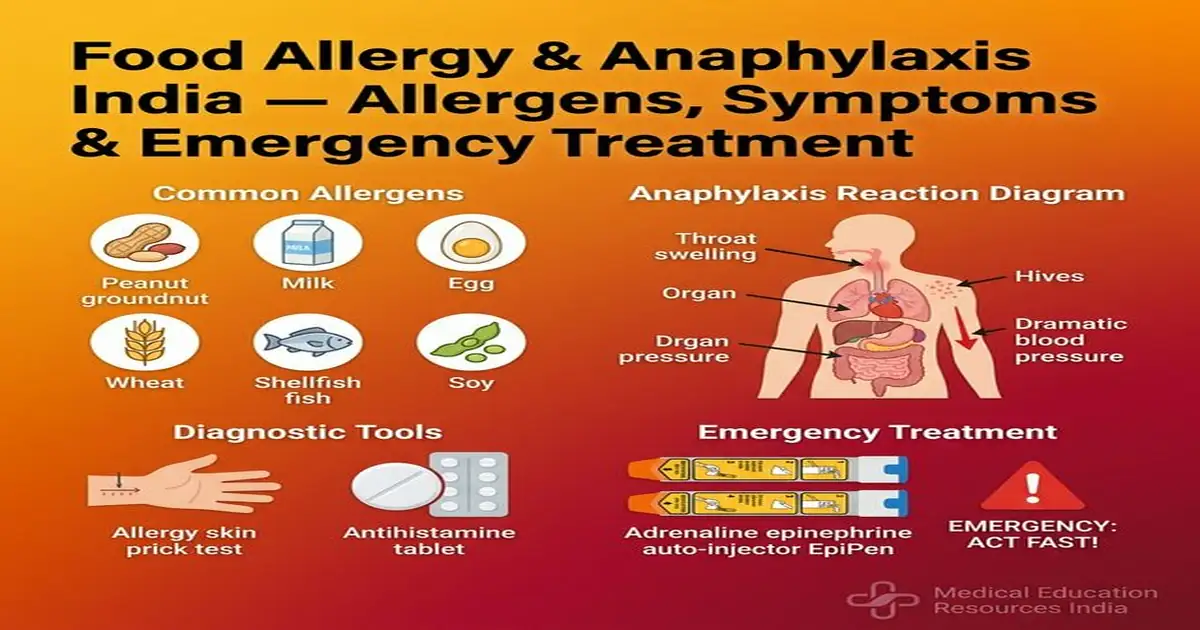
Food Allergy vs Food Intolerance — Critical Distinction
| Feature | Food Allergy (IgE-mediated) | Food Intolerance |
|---|---|---|
| Mechanism | IgE antibodies activate mast cells → histamine and other mediators released → allergic symptoms | Non-immune: enzyme deficiency (lactase in lactose intolerance), pharmacological (tyramine in cheese), irritant (spicy food) |
| Onset | Rapid — within minutes to 2 hours of exposure (immediate hypersensitivity) | Delayed — hours after ingestion; dose-dependent |
| Dose | Even trace amounts (milligrams) can trigger severe reaction — NOT dose-dependent | Usually dose-dependent — small amounts may be tolerated |
| Symptoms | Skin (hives, angioedema), respiratory (wheeze, throat tightening), cardiovascular (BP drop, collapse), GI (vomiting, diarrhoea) — anaphylaxis possible | Primarily GI: abdominal bloating, cramps, diarrhoea — no anaphylaxis risk |
| Testing | Skin prick test (SPT); specific IgE (ImmunoCAP/RAST); oral food challenge (gold standard) | Hydrogen breath test (lactose intolerance); elimination diet; food diary |
| Management | Strict lifelong avoidance; emergency epinephrine for anaphylaxis | Dose reduction; enzyme supplements (lactase drops for lactose intolerance); manage triggers |
Major Food Allergens in India
| Allergen | India Significance | Hidden Sources |
|---|---|---|
| Peanuts (groundnuts / moongphali) | Most common cause of anaphylaxis in India; widely used in Indian cooking (chikki, groundnut chutney, dal preparations, cooking oil); peanut allergy does NOT mean tree nut allergy | Peanut oil (refined peanut oil may be allergen-free, cold-pressed is not); mithais, chikki, groundnut chutney, satay sauce, some sabzi preparations, bhel puri |
| Milk (cow’s milk protein) | Most common food allergy in Indian infants (2–3%); distinct from lactose intolerance — milk protein triggers immune reaction; many Indian children outgrow by age 3–5 | Ghee (may contain milk protein traces), paneer, curd, kheer, mithai (almost all milk-based), cheese, butter, baked goods with milk, protein powders |
| Egg | 2nd most common after milk in children; egg white (albumin) is main allergen; egg yolk allergy less common; many children outgrow egg allergy | Baked goods (cakes, biscuits), mayonnaise, noodles, some vaccines (MMR, influenza — inform allergist) |
| Wheat / Gluten | Wheat allergy distinct from celiac disease (autoimmune) and non-celiac gluten sensitivity; wheat allergy is IgE-mediated with anaphylaxis risk; unusual for wheat to be severely allergenic in India despite high consumption — makes it less common allergically but celiac disease is underdiagnosed | Maida (refined wheat) in all breads, biscuits, pasta, sauces, soups; wheat starch in some medications |
| Shellfish and Fish | Significant allergen in coastal Indian populations (Kerala, Bengal, coastal Tamil Nadu, Goa); shellfish allergy (shrimp, prawn, crab) is the most common adult food allergy; shellfish allergy often persists lifelong | Fish sauce, shrimp paste in coastal preparations; Worcestershire sauce contains anchovies; shared cooking oil/vessels in restaurants causes cross-contamination |
| Tree nuts (cashew, almond, walnut) | Cashew nut is the most important tree nut allergen in India; a significant cause of anaphylaxis; cashew widely used in biryanis, mithais, gravies | Festivals (Diwali mithais, Holi sweets, biryani preparations), restaurant gravies (cashew-based white gravies ubiquitous in North Indian cuisine) |
🚨 Anaphylaxis — Recognition and Emergency Treatment
Anaphylaxis is a severe, potentially life-threatening systemic allergic reaction requiring immediate treatment with intramuscular epinephrine (adrenaline). It occurs when exposure to an allergen causes mast cell degranulation across multiple organ systems simultaneously. Diagnosis (World Allergy Organisation criteria — any ONE of three):
- 🔴 Criterion 1: Acute onset illness with skin/mucosal symptoms (hives, flushing, swollen lips/tongue/throat) PLUS at least one of: respiratory compromise OR reduced BP/syncope/collapse
- 🔴 Criterion 2: Two or more of following after exposure to likely allergen: skin/mucosal symptoms; respiratory compromise; reduced BP/collapse; persistent GI symptoms (vomiting, cramping)
- 🔴 Criterion 3: Reduced BP alone after exposure to KNOWN allergen
| Step | Action | India Context |
|---|---|---|
| 1 — Assess & Call 108 | Recognise anaphylaxis; call emergency services immediately (108); lay person flat with legs raised (unless breathing difficulty — then sit up); do NOT leave alone | 108 must be called even if person appears to improve — biphasic anaphylaxis can recur 4–8 hours later without re-exposure |
| 2 — Epinephrine FIRST (IM) | Adrenaline 0.01 mg/kg IM into outer thigh (through clothing if needed); adult dose: 0.5 mg (0.5 mL of 1:1000); child: 0.01 mg/kg; may repeat after 5 minutes if no improvement | THIS IS THE ONLY LIFE-SAVING TREATMENT. Antihistamines and steroids are adjuncts — they do NOT stop anaphylaxis. In India, epinephrine auto-injectors exist but are rare; standard 1mL syringe with adrenaline 1:1000 ampule used in hospitals; families with known severe allergy should carry adrenaline ampule + syringe |
| 3 — Position | Flat with legs elevated for hypotension; semi-recumbent for respiratory distress; recovery position if unconscious | Do NOT make the person sit or stand — orthostatic fall in already hypotensive anaphylaxis is fatal |
| 4 — Oxygen | High-flow oxygen via face mask if available; ambulance should provide | 108 ambulances should carry oxygen and adrenaline; ALS ambulances in metro cities have IV access |
| 5 — Antihistamine + Steroid (adjuncts) | IV chlorpheniramine (antihistamine) + IV hydrocortisone after epinephrine; these do NOT replace epinephrine; they reduce secondary reactions and urticaria | Many Indian healthcare workers administer antihistamines first and delay epinephrine — this is the most dangerous management error in anaphylaxis |
| 6 — Hospital observation | Minimum 4–6 hours observation after apparent recovery; biphasic reactions occur in 5–20% without re-exposure; ICU observation for severe reactions | Discharging anaphylaxis patients immediately after improvement is dangerous; prescribe epinephrine auto-injector on discharge; refer to allergist |
Frequently Asked Questions
How is food allergy diagnosed in India?
Accurate food allergy diagnosis is essential — overdiagnosis leads to unnecessary dietary restriction with nutritional consequences, while underdiagnosis leaves patients at anaphylaxis risk. The diagnostic pathway: Clinical history — the foundation: Detailed account of the reaction: which food, how prepared, how much consumed, time to onset of symptoms (IgE-mediated: <2 hours), nature of symptoms (skin, respiratory, GI, cardiovascular), resolution with treatment. Consistent reproducibility across multiple exposures. Skin Prick Test (SPT): Allergen extract placed on forearm → punctured through → after 15 minutes, a wheal (raised bump) ≥3mm larger than negative control = positive. Sensitivity 70–90%; specificity 70–80% for most foods. Key limitation: a positive SPT means sensitisation (antibodies present) — not necessarily clinical allergy (some sensitised individuals tolerate the food without symptoms). Cost: ₹500–2,000 at allergist clinics; available in major cities. Specific IgE blood test (ImmunoCAP/RAST): Measures serum levels of food-specific IgE antibodies. Useful when SPT is not feasible (extensive eczema, dermographism). High IgE levels correlate with clinical allergy probability. Available at private diagnostics (Metropolis, SRL) ₹800–1,500 per allergen. Oral Food Challenge (OFC) — Gold Standard: Supervised feeding of increasing amounts of suspected food under medical observation; confirms or refutes clinical allergy; essential when SPT/specific IgE is ambiguous; performed at hospital with anaphylaxis management capability; the definitive test. Limited availability in India — major academic centres and private allergy clinics in metros. What NOT to use: IgG food allergy tests — widely marketed in India by wellness laboratories as detecting “food sensitivity” — these measure IgG antibodies which are normal immune responses to ingested food proteins; IgG4 food tests have NO diagnostic value for food allergy; they lead to unnecessary dietary restrictions; strongly discouraged by all major allergy societies. Hair analysis, applied kinesiology, ELISA panels for 90+ foods from wellness clinics — none of these are validated for food allergy diagnosis.
Can food allergy be cured?
The food allergy treatment landscape has changed dramatically in the last decade — moving from “strict avoidance only” to active immunotherapy approaches: Natural outgrowth (in children): Many childhood food allergies resolve naturally with age: Milk allergy: 80%+ resolve by age 5–6. Egg allergy: 70%+ resolve by age 5. Wheat allergy: most resolve by school age. Peanut, tree nut, shellfish, sesame: typically PERSIST into adulthood — these are the “permanent” allergies requiring lifelong management. Outgrowth is monitored by periodic repeat SPT and specific IgE — and confirmed by supervised OFC. Oral Immunotherapy (OIT) — the breakthrough treatment: Controlled daily ingestion of gradually increasing amounts of the allergen (starting at microgram amounts) → desensitisation → eventually able to tolerate clinically significant amounts. Peanut OIT (Palforzia — FDA-approved oral peanut immunotherapy): now available internationally; reduces risk of anaphylaxis on accidental exposure; does not cure allergy but raises threshold dramatically. OIT available in India at select allergy centres (mainly private, metros) — not yet widely accessible. Requires careful medical supervision during dose escalation. Anti-IgE therapy (omalizumab/Xolair): Monoclonal antibody that binds IgE — reduces anaphylaxis risk; approved by FDA as adjunct to OIT (allows faster dose escalation) and as standalone for multifood allergy; available in India at ₹8,000–15,000/injection monthly; very expensive for long-term use. For most Indian families currently: Strict allergen avoidance remains the cornerstone; education on hidden allergens; emergency epinephrine for known severe allergy; periodic allergist review; OIT referral where feasible for peanut/milk/egg allergy in children aged 4–17.
Is peanut allergy common in vegetarian Indians?
Peanut allergy has a complex and India-specific pattern that differs meaningfully from Western epidemiology: India’s peanut allergy paradox: Despite peanuts being consumed ubiquitously from infancy in India (groundnut chutney, chikki in childhood; peanut oil for cooking), India’s peanut allergy rates are significantly lower than in Western countries (0.5–1% vs 1.5–2% in USA/UK). This appears to support the dual exposure hypothesis (Lack hypothesis): early oral exposure to peanut (eating peanuts in infancy) promotes tolerance, while percutaneous sensitisation (peanut protein in skin creams, through inflamed eczema skin) promotes allergy. India’s early and robust oral peanut exposure from weaning may be protective — similar to why traditional Israeli children (who eat peanut-based snacks from infancy) have far lower peanut allergy than UK children (where peanut was historically avoided in infancy). The LEAP (Learning Early About Peanut) study proved this definitively: early peanut introduction in high-risk infants reduced peanut allergy by 80%. India has inadvertently practiced this protective feeding pattern for generations. Who is at risk in India despite this: Infants with severe eczema who are not introduced to peanut early, or who had peanut exposure only through inflamed skin before oral introduction; children in urban India with eczema and delayed weaning practices; individuals who develop peanut sensitisation through non-dietary routes. Vegetarian consideration: Peanut is a critical protein source for vegetarian Indians — peanut allergy in a vegetarian child has significant nutritional implications and requires careful dietitian support to ensure protein adequacy without peanut, using alternatives like lentils, dal, paneer, and seeds.
Why are antihistamines not enough for anaphylaxis?
This is the most dangerous misconception in Indian allergy management — and understanding the pharmacology makes the answer clear: Anaphylaxis mechanisms requiring epinephrine: Anaphylaxis involves simultaneous activation of mast cells and basophils releasing histamine PLUS a cascade of other mediators: prostaglandins (bronchoconstriction), leukotrienes (prolonged bronchoconstriction), tryptase (vascular activation), platelet-activating factor (severe hypotension), and others. Histamine is only ONE of these mediators. What antihistamines do (and don’t do): Antihistamines (cetirizine, chlorpheniramine, diphenhydramine) BLOCK the H1 receptor — preventing histamine-mediated effects (itching, hives, some vasodilation). They do NOTHING to: reverse bronchospasm (life-threatening airway narrowing); reverse the profound hypotension from non-histamine mediators; restore vascular tone; prevent or treat airway oedema (angioedema of throat/larynx which can kill by obstruction). An anaphylaxis patient dying from bronchospasm and cardiovascular collapse is not dying from a histamine excess that antihistamine can address — they are dying from a mediator storm that only epinephrine can reverse. What epinephrine does: Alpha-1 agonism → peripheral vasoconstriction → reverses hypotension → maintains brain and heart perfusion. Beta-2 agonism → bronchodilation → opens obstructed airways → reverses bronchospasm. Beta-1 agonism → increases heart rate and contractility → supports cardiac output. Inhibits mast cell degranulation → reduces ongoing mediator release. Epinephrine works within 1–5 minutes. It is safe at appropriate IM doses. Steroids: IV hydrocortisone takes 4–6 hours to have anti-inflammatory effect — completely useless for acute anaphylaxis. Useful for preventing biphasic reactions (delayed second wave). The correct protocol: Epinephrine FIRST. ALWAYS. Then call 108. Then antihistamine. Then steroid. Any teaching, training, school protocol, or emergency card that lists antihistamine before epinephrine is wrong and potentially fatal.
How should schools and parents manage children with food allergy in India?
India has no national standard for school food allergy management — unlike the UK (Every Child Matters — school anaphylaxis policy mandatory) or USA (Section 504 plans). This creates significant risk in an environment where food sharing, mithai distribution, and communal eating are culturally integral: Essential components of school allergy management (for parents and school administrators): Written Allergy Action Plan: Created by the child’s allergist; lists the child’s allergens, reaction history, threshold (if known), and step-by-step treatment at school. Copy kept with class teacher, school nurse (if present), and principal. Emergency medication at school: Epinephrine (adrenaline 1:1000 ampule + 1mL syringe) kept accessible (class teacher’s desk, not locked away in a distant medical room); antihistamine tablet as secondary. Staff training: At minimum, the homeroom teacher should be able to recognise anaphylaxis and administer IM epinephrine. Training sessions by allergist available through IAP (Indian Academy of Pediatrics) and Indian College of Allergy Asthma and Applied Immunology (ICAAI). Allergen labelling on food: FSSAI requires labelling of 8 main allergens on packaged food (peanuts, milk, egg, wheat, soy, tree nuts, fish, shellfish) — check labels routinely. Tiffin box policy: Request school to prohibit food sharing for allergy-affected children and display allergen cards. Festivals and special occasions: Diwali mithai distribution and birthday celebrations are highest-risk periods — communicate clearly with teacher in advance; provide allergen-safe alternatives. For parents of newly diagnosed children: Consult a paediatric allergist for full evaluation and action plan. Ensure duplicate medication at home, grandparents’ home, and school. Train all adult caregivers in epinephrine administration. Educate the child age-appropriately — children as young as 5–6 can learn “these foods make me sick, I must not eat them without checking with mama/teacher.” Join allergy parent communities (Food Allergy India — online resource community).
What to Read Next
- Asthma — Food Allergy (Especially Peanut & Shellfish) Triggers Bronchospasm in Asthmatic Patients
- Eczema — Severe Eczema in Infancy is a Major Risk Factor for Later Food Allergy Development
- Anxiety — Food Allergy Anxiety is Common; Safe Exposure Protocols Reduce Fear Without Increasing Risk
- Vitamin B12 — Milk Allergy-Related Diet Restrictions Can Cause B12 Deficiency in Children
- Iron Deficiency — Multiple Food Exclusions Can Lead to Nutritional Deficiencies
A child with a peanut allergy at a Diwali party, a guest with a shellfish allergy at a Bengali wedding, a student with a tree nut allergy at a school celebration — these are not unusual scenarios in modern India. The difference between a managed incident and a tragedy is measured in seconds and in one medication: epinephrine. This knowledge belongs in every home, every school, every dhabha, and every community hall in India.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on World Allergy Organisation (WAO) Anaphylaxis Guidelines, ICAAI (Indian College of Allergy Asthma and Applied Immunology) standards, and LEAP Study evidence. Last updated: March 2026.
Authoritative Sources: World Allergy Organisation | ICAAI India | Australasian Society of Clinical Immunology and Allergy | FARE — Food Allergy Research
🚨 Anaphylaxis Emergency: For suspected anaphylaxis — give IM adrenaline (epinephrine) into the outer thigh FIRST. Call 108. Do NOT wait for antihistamines to work. Do NOT make the person sit or stand. Lay flat, legs raised. EPINEPHRINE FIRST — always.
⚕️ Medical Disclaimer: This article is for general informational and educational purposes. Food allergy diagnosis requires clinical evaluation and specialist testing. IgG food allergy tests have no diagnostic validity. Any child with a history of anaphylaxis must be under regular allergist care with an emergency action plan.
