Last Updated: March 2026 | Reading Time: 9 minutes | ~2,000 words
Benign Prostatic Hyperplasia (BPH) is the most common urological condition in ageing men — affecting over 50% of men by age 60, and up to 90% by age 85, making it virtually inevitable if a man lives long enough. India’s rapidly ageing male population — with over 70 million men aged 60+ — means BPH is a massive and growing public health burden. Despite its ubiquity, BPH is widely undertreated in India due to misconceptions: that urinary symptoms in old age are “normal,” that surgery is the only option, and that discussing urinary problems is embarrassing. In reality, BPH has highly effective medical and minimally invasive treatments that dramatically improve quality of life. Simultaneously, prostate cancer — now the 2nd most common cancer in Indian urban men — requires awareness of PSA testing, its limitations, and when cancer evaluation is warranted vs when watchful waiting is appropriate.
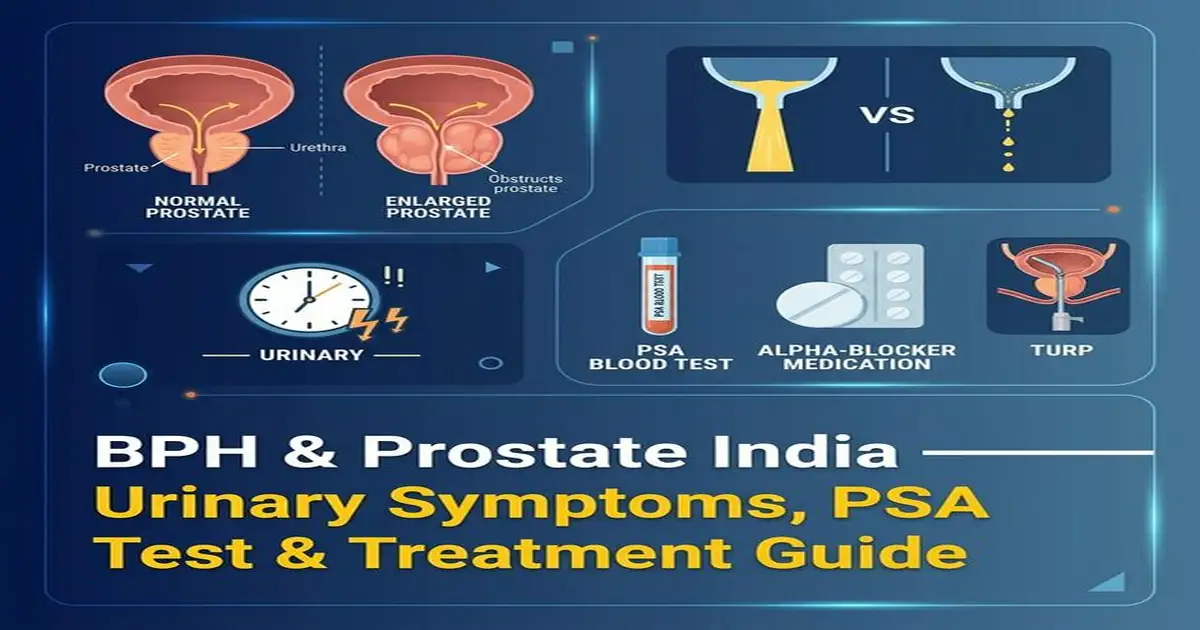
BPH Symptoms — IPSS Score Guide
BPH symptoms are collectively termed LUTS — Lower Urinary Tract Symptoms — and divided into obstructive (from enlarged prostate compressing the urethra) and irritative (from secondary bladder changes). The International Prostate Symptom Score (IPSS) is a 7-question validated tool that quantifies severity and guides treatment decisions:
| Symptom Type | Symptoms | IPSS Score | Management Threshold |
|---|---|---|---|
| Obstructive (voiding) | Weak urine stream (reduced force); hesitancy (delay before flow starts); intermittency (stream stops and starts); sensation of incomplete bladder emptying; straining to urinate; terminal dribbling | 0–7 (mild), 8–19 (moderate), 20–35 (severe) | Mild (0–7): watchful waiting + lifestyle; Moderate (8–19): medical treatment; Severe (20–35): consider surgical referral |
| Irritative (storage) | Urgency (sudden strong urge to urinate); frequency (urinating more than 8 times/24 hours); nocturia (waking 2+ times at night to urinate — most quality-of-life-impacting symptom for Indian men); urge incontinence | Nocturia ≥2 episodes/night = significant symptom burden | Nocturia severely impacts sleep quality, daytime function, fall risk in elderly, and sexual function; undertreated in India |
| Complications (red flags) | Acute urinary retention (AUR — complete inability to urinate; extreme pain); haematuria (blood in urine — always investigate regardless of BPH); recurrent UTI; renal impairment | Not scored — require immediate urological evaluation | AUR = catheterisation emergency; haematuria with BPH = exclude bladder/prostate cancer; bilateral hydronephrosis from chronic retention = renal emergency |
Diagnosis — What Tests Are Needed?
| Test | Purpose | India Notes |
|---|---|---|
| IPSS questionnaire + clinical history | Quantify symptom severity; guide treatment decisions; establish baseline for monitoring treatment response | Available free; takes 5 minutes; most important initial assessment; many Indian urologists skip this for a quick prescription |
| Digital Rectal Examination (DRE) | Assess prostate size, consistency, symmetry; smooth enlarged gland = BPH; hard, nodular, asymmetric = cancer concern → biopsy | Often declined or skipped due to patient embarrassment in India; essential component of prostate evaluation — cannot substitute with blood tests |
| PSA (Prostate-Specific Antigen) | Serum PSA level; elevation can indicate BPH, prostatitis, or prostate cancer; PSA 0–4 ng/mL (age-adjusted); PSA 4–10 ng/mL = “grey zone”; PSA >10 ng/mL = significant cancer concern | PSA is prostate-specific — NOT cancer-specific; large benign prostates elevate PSA too; PSA density (PSA/prostate volume) and PSA velocity (rate of rise over time) add diagnostic specificity; PSA testing in India: available at most hospitals ₹500–1,000 |
| Uroflowmetry | Measures urine flow rate and pattern; peak flow rate (Qmax) <10 mL/sec = significant obstruction; post-void residual (PVR) → incomplete emptying assessment | Available at district hospitals; more objective than symptoms alone; useful pre-surgical assessment |
| Ultrasound (transabdominal/TRUS) | Prostate volume measurement (50g+ = significantly enlarged); post-void residual (PVR) urine measurement; upper tract assessment (hydronephrosis from chronic obstruction) | Widely available India; TRUS (transrectal ultrasound) + TRUS-guided biopsy for prostate cancer evaluation |
| Urine analysis + culture | Exclude UTI as cause of LUTS; exclude haematuria from other causes; dipstick in all men with LUTS | Urinalysis at every PHC; essential first step before prescribing |
Treatment Options — Medical to Surgical
| Treatment | How It Works | Best For | India Cost |
|---|---|---|---|
| Alpha-blockers (tamsulosin, alfuzosin, silodosin) | Relax smooth muscle in prostate and bladder neck → improved urine flow within 48–72 hours; most rapid symptom relief | First-line for moderate-severe LUTS; especially irritative symptoms; prostate size any | Tamsulosin 0.4mg: generic ₹5–15/tablet; widely available; first choice in India |
| 5-Alpha Reductase Inhibitors — 5ARIs (finasteride 5mg, dutasteride 0.5mg) | Block testosterone→DHT conversion → reduce prostate volume by 20–30% over 3–6 months; prevent disease progression; reduce AUR risk 50% | Enlarged prostate (>30g) on ultrasound; PSA >1.4 ng/mL; best for large glands; prevents long-term progression | Finasteride 5mg generic ₹5–20/tablet; dutasteride ₹30–80/tablet; need 6 months for full effect; reduce PSA by 50% (important for PSA interpretation) |
| Combination therapy (alpha-blocker + 5ARI) | MTOPS and CombAT trials prove superior to monotherapy for large glands; rapid symptom relief (alpha-blocker) + long-term size reduction (5ARI) | Large prostate (>40g) with moderate-severe LUTS; men at risk of progression; most cost-effective long-term strategy for large BPH | Combination tablet (Dutas-T — dutasteride + tamsulosin) available India ₹30–80/tablet; generic tamsulosin + generic finasteride separately ₹20–35/day total |
| TURP (Transurethral Resection of Prostate) | Endoscopic surgical resection of obstructing prostate tissue; most effective surgical option; no external incision; gold standard surgical treatment BPH; 85–90% symptom improvement | Failed medical therapy; AUR; large prostate; bladder stones; renal impairment; patient preference for surgical cure | Government hospital ₹20,000–50,000; private ₹80,000–2,50,000; PMJAY covers TURP at empanelled hospitals |
| Laser prostatectomy (HoLEP, GreenLight) | Laser energy enucleates or vaporises prostate tissue; lower bleeding risk than TURP; suitable for very large prostates and anticoagulated patients | Very large prostate (>80g); patients on blood thinners; preferred in centres with laser technology | Private ₹1–3 lakhs; not universally available India; superior to TURP for large glands |
Frequently Asked Questions
What is the PSA test and when should Indian men get it?
PSA (Prostate-Specific Antigen) is a glycoprotein produced by prostate epithelial cells and secreted into seminal fluid, with small amounts entering the bloodstream. It is the most important and most misunderstood tumour marker in men’s health: What PSA measures: PSA is elevated by anything that stimulates or disrupts the prostate gland: BPH (enlarged benign prostate); prostatitis (prostate infection/inflammation); prostate cancer; prostate biopsy or DRE (temporary elevation); ejaculation within 24 hours of testing (minor elevation); urinary catheter trauma; certain medications (testosterone therapy increases PSA). PSA is therefore prostate-specific — NOT cancer-specific. Approximately 25% of men with PSA 4–10 ng/mL have prostate cancer on biopsy — meaning 75% with an “elevated” PSA in the grey zone do NOT have cancer. Conversely, 15–25% of men with PSA <4 ng/mL may have prostate cancer — a “normal” PSA is not a cancer exclusion. Age-adjusted PSA thresholds: 40–49 years: PSA >2.5 ng/mL = concern; 50–59 years: PSA >3.5 ng/mL = concern; 60–69 years: PSA >4.5 ng/mL = concern; 70+ years: PSA >6.5 ng/mL = age-adjusted threshold. PSA density and velocity: PSA density (PSA ÷ prostate volume in mL) <0.15 suggests BPH; >0.15 raises cancer concern. PSA velocity (PSA rise >0.75 ng/mL/year) is concerning for cancer independent of absolute level. Who should be tested in India: Men with LUTS — PSA at initial evaluation; Men aged 50–75 wishing to be screened (shared decision-making — PSA screening does reduce prostate cancer deaths by 20–25% but leads to overdiagnosis and overtreatment of slow-growing cancers); Men with family history of prostate cancer — screening from age 45; Men of African descent (higher prostate cancer risk) — age 40 screening. Important: 5ARI drugs (finasteride, dutasteride) reduce PSA by approximately 50% — a man on finasteride with PSA 2.5 ng/mL has an effective PSA of 5 ng/mL — must be communicated to interpreting physician. 5ARIs do NOT mask prostate cancer effectively; PSA still rises appropriately through treatment with aggressive cancer.
Can BPH lead to prostate cancer?
This is one of the most common concerns men with BPH express — and the good news is clearly defined: BPH does NOT cause prostate cancer and does NOT increase prostate cancer risk. They are entirely separate conditions with different pathophysiology: BPH (benign hyperplasia) arises in the transition zone and periurethral glands of the prostate — the central gland region compressing the urethra. Prostate cancer typically arises in the peripheral zone — the outer back portion of the prostate (which is why DRE can palpate early prostate cancers, as the finger reaches the posterior prostate). These are histologically and anatomically distinct processes that happen to occur in the same organ and therefore can coexist coincidentally in ageing men — just as both commonly increase in prevalence with age. Why the confusion exists: Both BPH and prostate cancer elevate PSA — so men being managed for BPH may have a PSA test that raises cancer concern; this leads to biopsy in some cases where cancer is found — not caused by BPH, but coincidentally present. Both BPH and prostate cancer can cause LUTS, making clinical differentiation important. Both are androgen-dependent conditions — testosterone and DHT drive growth of both benign and malignant prostate tissue. What men with BPH should understand: Having BPH does NOT mean you are more likely to develop prostate cancer. BUT men with BPH are in the age group where prostate cancer is most prevalent — so prostate cancer screening (PSA + DRE) is important as a separate check, not as a consequence of BPH. This distinction reduces unnecessary anxiety while maintaining vigilance about prostate cancer as a distinct concern in ageing men.
Can lifestyle changes improve BPH symptoms?
Lifestyle modification has meaningful evidence for BPH symptom improvement — particularly for irritative LUTS and nocturia — and should be integrated into first-line management alongside or before medication: Fluid management — the most impactful single change: Total daily fluid: Aim for 1.5–2 litres total (reduce if overdrinking is identified as a driver of frequency); avoid excessive fluid after 6pm (to reduce nocturia — the most bothersome symptom for most men). Caffeine reduction: Coffee and tea are diuretics AND bladder irritants — the dual hit worsens frequency and urgency significantly; reducing from 6 cups to 2 cups can reduce nocturia episodes by 1–2 per night. Alcohol: Evening alcohol is a potent diuretic and sleep disruptor → worsens nocturia; reducing evening alcohol consumption is highly effective. Diet and metabolic factors: Lycopene-rich foods (tomatoes, especially cooked/processed — lycopene bioavailability is higher in cooked tomato): epidemiological evidence for prostate health benefit (reduces BPH progression and prostate cancer risk). Zinc-rich foods (pumpkin seeds, sesame, chickpeas): zinc concentrates in prostate tissue; some evidence for BPH progression reduction. Reducing spicy food: capsaicin irritates bladder urothelium → worsens urgency and frequency in BPH; significant in Indian diet context. BMI reduction: Obesity is associated with larger prostate volume and more severe LUTS — weight loss (5–10%) improves IPSS scores meaningfully in obese men with BPH. Bladder training: Timed voiding (urinating according to schedule rather than urgency) can increase functional bladder capacity over 6–8 weeks; pelvic floor training reduces urgency incontinence. “Urge suppression techniques” (distraction, deep breathing at urgency) can reduce urgency-driven frequency without medication. Exercise: Regular aerobic exercise — walking 30 minutes daily — is associated with 25% reduction in LUTS severity in observational studies; reduces sympathetic nervous system tone that drives smooth muscle contraction in the prostate/bladder neck.
What happens if BPH is left untreated?
In many men, mild BPH improves spontaneously or remains stable for years. However, in men with moderate-severe symptoms or large prostates, untreated BPH carries real risks: Acute Urinary Retention (AUR): The most dramatic complication — sudden complete inability to urinate, causing intense suprapubic pain and bladder distension. Requires emergency urethral catheterisation within hours. AUR risk is 2–3% per year in men with moderate BPH untreated; risk doubles with each 5-year increment of age. AUR can be triggered by: high fluid intake at one sitting (wedding/party drinking); cold weather (alpha-adrenergic stimulation); medications (decongestants, antihistamines — most common trigger; tramadol; antidepressants); prolonged immobility; constipation. Treatment with 5ARIs reduces 5-year AUR risk by 57% (PLESS trial evidence). Chronic Urinary Retention (CUR): Gradual incomplete bladder emptying — the bladder never fully empties; PVR (post-void residual) >300 mL indicates high-pressure retention. Bladder detrusor muscle hypertrophies then decompensates → permanent detrusor dysfunction. Most dangerous consequence: bilateral ureteric obstruction → bilateral hydronephrosis → chronic kidney disease → end-stage renal disease. This silent renal failure from untreated BPH is a significant cause of preventable CKD in India — patients present with uraemia (nausea, fatigue, breathlessness) without recognising the urinary retention cause. Urinary Tract Infections: Incomplete bladder emptying → stagnant urine → bacterial proliferation → recurrent UTIs; complicated pyelonephritis in elderly men → sepsis. Men with recurrent UTIs should always have post-void residual assessed. Bladder stones: Concentrated, stagnant urine → crystal precipitation → bladder stone formation; causes haematuria, UTI, and worsened LUTS; requires cystoscopic removal. Bladder decompensation: Years of fighting to empty against resistance → bladder muscle decompensates → atonic bladder — at this point, even surgical relief of obstruction (TURP) may not restore normal voiding. Early treatment prevents this irreversible endpoint.
Are there side effects of BPH medications I should know about?
BPH medications are generally well-tolerated but have specific side effects that Indian men should understand — because unreported or misunderstood side effects are a primary reason for medication discontinuation: Alpha-blockers (tamsulosin, alfuzosin, silodosin): Postural hypotension — the most clinically significant side effect; especially on first dose and first few days; the alpha-blocking effect lowers blood pressure when standing; risk of falls in elderly; take first dose at bedtime to reduce symptom impact; particularly dangerous combined with phosphodiesterase-5 inhibitors (sildenafil/tadalafil — used for ED) — combination can cause severe hypotension. Retrograde ejaculation — silodosin and tamsulosin cause ejaculate to go backward into the bladder rather than out (dry orgasm); harmless but alarming if unexpected; more common with silodosin (28% incidence) vs tamsulosin (6%); reversible on stopping. Dizziness, fatigue — mild, common. Intraoperative Floppy Iris Syndrome (IFIS) — important: men on tamsulosin who require cataract surgery must inform their ophthalmologist, as alpha-blockers affect iris dilator muscles during surgery; serious complication if surgeon is not warned — requires specialised surgical technique. 5-Alpha Reductase Inhibitors (finasteride, dutasteride): Sexual side effects — erectile dysfunction (development or worsening in 5–9%), reduced libido (6%), ejaculatory disorders (7%), reduced ejaculate volume — mediated through DHT reduction in penile/libido physiology. These side effects often improve after 6–12 months as adaptation occurs. Post-Finasteride Syndrome — a controversial and debated entity where some men report persistent sexual dysfunction, depression, and cognitive symptoms after stopping finasteride; the evidence is conflicting; it is not recognised by regulatory bodies as an established syndrome but real cases exist; discussing expectations before starting is important. PSA reduction — 5ARIs reduce PSA by 50% within 6 months; this MUST be communicated: a “normal” PSA on 5ARI requires doubling the value for clinical interpretation. Rare but reported: small increased risk of high-grade prostate cancer detection (more aggressive cancer selection — though this is a complex statistical issue, not a genuine cancer risk increase).
What to Read Next
- Prostate Cancer — BPH and Prostate Cancer Can Coexist; PSA Screening Guide for Indian Men
- Diabetes — Diabetic Autonomic Neuropathy Worsens BPH Bladder Dysfunction
- CKD — Chronic Urinary Retention from BPH is an Underrecognised Cause of Renal Failure
- Sleep Disorders — Nocturia from BPH is a Primary Driver of Sleep Disruption in Indian Men
- Hypertension — Alpha-Blockers Treat Both BPH and Hypertension Simultaneously
The Indian man who wakes 4 times a night to urinate, who no longer attends weddings for fear of urgency, who avoids long bus journeys — he often believes this is simply “getting old.” It is not. It is BPH, and it is treatable. A tamsulosin tablet daily, some evening fluid restriction, reduced tea-drinking — and he sleeps through the night. This article exists so that more Indian men know it is treatable, and fewer spend their later years unnecessarily confined by a condition that responds to a five-rupee tablet.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on EAU (European Association of Urology) BPH Guidelines 2024, AUA (American Urological Association) BPH Guidelines, and USI (Urological Society of India) clinical practice. Last updated: March 2026.
Authoritative Sources: EAU BPH Guidelines | AUA — American Urology Association | Urological Society of India
⚕️ Medical Disclaimer: This article is for general information only. Haematuria (blood in urine) always requires urgent urological evaluation — do not assume it is from BPH alone. PSA testing should involve shared decision-making with a physician. Acute urinary retention is a medical emergency — go to hospital immediately.
