Last Updated: March 2026 | Reading Time: 8 minutes | ~1,900 words
Acne vulgaris is the most common skin condition globally — affecting an estimated 80–85% of adolescents and a significant proportion of adults, with prevalence rates in India ranging from 25–58% among teenagers. While often dismissed as a cosmetic inconvenience, acne causes significant psychological distress — depression, social anxiety, reduced quality of life — and can lead to permanent scarring if inadequately treated. India has specific acne challenges: high ambient temperatures and humidity increase sebum production; air pollution (PM2.5 — Delhi, Mumbai) clogs pores; widespread use of oily hair oils (coconut, almond) applied to forehead and neck (pomade acne); high PCOS prevalence in Indian women drives hormonal acne; and critically, a deeply rooted culture of self-medication with over-the-counter creams (often containing topical steroids — which worsen acne as perioral steroid dermatitis or steroid acne). The cornerstone of acne management is understanding its four key pathogenic mechanisms: excess sebum production (androgenic drive), follicular hyperkeratinisation (blocked pores — comedones), Cutibacterium acnes (C. acnes) bacterial colonisation, and inflammatory cascade (papules, pustules, nodules, cysts).
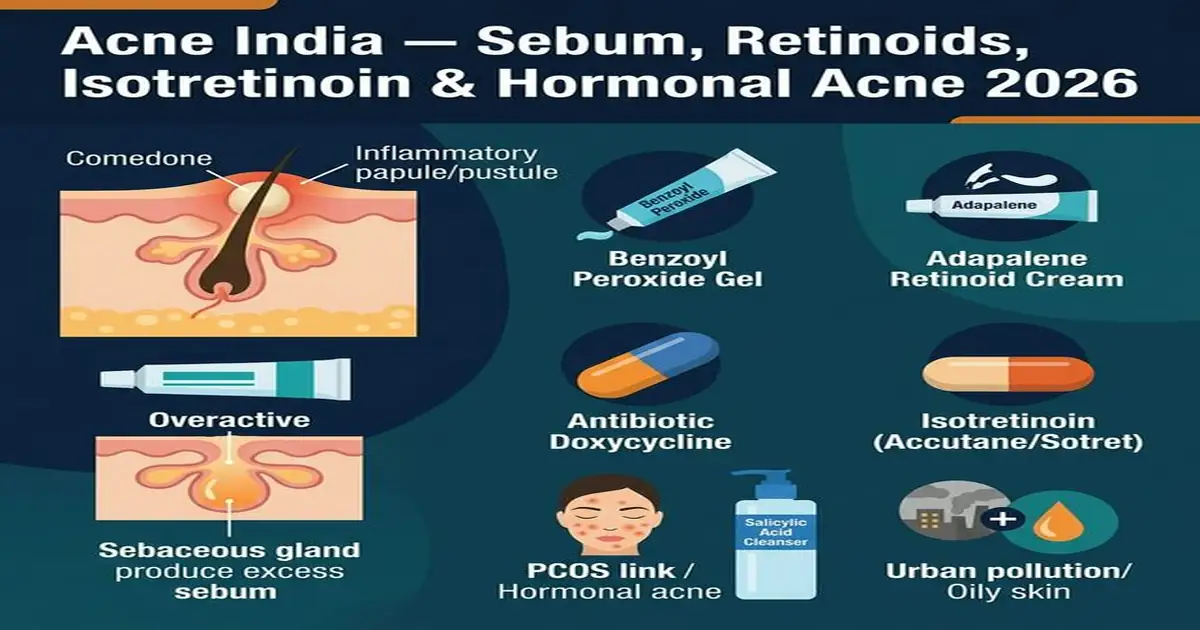
Acne Treatment — Evidence-Based Graded Approach
| Acne Grade | Lesion Type | First-Line Treatment | India-Specific Notes | India Cost |
|---|---|---|---|---|
| Mild (Grade I–II) | Comedones (open blackheads/closed whiteheads) ± few papules; <10 lesions; no nodules/cysts | Topical retinoid: adapalene 0.1% gel (first-line — also available 0.3%); tretinoin 0.025%/0.05% cream; controls both comedones AND inflammation; apply nightly to entire affected area (not spot-treat); takes 8–12 weeks for full effect; ± topical benzoyl peroxide (BPO) 2.5–5% gel (bacterial resistance prevention — reduces C. acnes; anti-inflammatory; add BPO when using retinoid; combination adapalene-BPO one gel — Epiduo) | BPO bleaches fabric — warn patients; adapalene less irritating than tretinoin (preferred in hot Indian climate — tretinoin irritation worsened by heat/humidity); many Indian patients use salicylic acid face wash as sole treatment — inadequate for Grade II+; start adapalene slowly (every other night first week) to acclimatise; sunscreen essential with retinoids (photosensitising) — especially important in India | Adapalene 0.1% gel 15g (Adaferin, Tazret Gel): ₹150–300; Tretinoin cream (A-Ret): ₹80–200; BPO gel (Pepsil, Acnedap): ₹100–200; Sunscreen SPF 50 (La Shield, Re’equil): ₹300–500 |
| Mild-Moderate (Grade II) | Predominantly inflammatory papules/pustules; 10–30 lesions; limited to face ± chest/back; no nodules | Topical combination: Adapalene 0.1% + BPO 2.5% gel (first-line; apply nightly) ± topical clindamycin 1% gel (daytime — anti-C.acnes; always combine clindamycin with BPO to prevent resistance — NEVER clindamycin monotherapy); alternative: azelaic acid 15–20% gel (anti-inflammatory + comedolytic + anti-pigmentation — excellent for post-inflammatory hyperpigmentation PIH which is a major concern in darker Indian skin) | India-specific: PIH (post-inflammatory hyperpigmentation — dark marks after acne lesion resolves) is a disproportionate concern for Indian patients with Fitzpatrick III–VI skin types (darker melanin makes PIH more pronounced and slower to fade); azelaic acid addresses both inflammation and PIH simultaneously — under-prescribed in India; dapsone 5% gel (anti-inflammatory; good for sensitive skin); topical niacinamide (not prescription — cosmeceutical — reduces sebum and PIH; widely available India; OTC) | Clindamycin 1% gel (Clindac A): ₹80–150; Aziderm 10% cream (azelaic acid): ₹180–250; Dapsone gel (Aczone): ₹400–600 |
| Moderate-Severe (Grade III) | Multiple papules/pustules; ≥30 lesions; ± early nodules; truncal acne | Oral antibiotics: doxycycline 100mg once daily (first-line oral antibiotic — anti-C.acnes and anti-inflammatory; use for maximum 3 months then stop — antibiotic resistance); ALWAYS combine with topical retinoid + BPO during oral antibiotic course; alternatives: lymecycline 408mg once daily; minocycline 100mg once daily (higher vestibular side effects in India — doxycycline preferred); azithromycin pulse (azithromycin 500mg Mon/Wed/Fri — useful in India for tetracycline-intolerant patients but resistance increasingly problematic) | Oral antibiotics should NEVER be used as monotherapy for acne (resistance); maintain topical retinoid + BPO throughout and after stopping antibiotic course (BPO prevents resistance; retinoid maintains control); doxycycline contraindicated <8 years and in pregnancy; take with food and water (reduce oesophageal irritation); photosensitivity — sunscreen mandatory in India; India: doxycycline generic extremely cheap and widely available | Doxycycline 100mg (generic): ₹5–10/capsule; 3-month course ≈ ₹450–900; lymecycline: ₹15–25/capsule |
| Severe (Grade IV — Nodulocystic) | Multiple nodules (≥5mm) and cysts; scarring; extensive truncal involvement; acne conglobata | Oral isotretinoin (Accutane/Sotret/Sanciret India): 0.5–1mg/kg/day × 16–24 weeks (cumulative dose target 120–150mg/kg); mechanisms: reduces sebum 70–90%; normalises follicular keratinisation; anti-inflammatory; reduces C. acnes (indirect — sebum reduction); highly effective — 80–90% achieve prolonged remission after one course; repeat course if relapse | CRITICAL — isotretinoin teratogenicity: absolutely contraindicated in pregnancy (causes catastrophic fetal anomalies — cardiac, CNS, craniofacial); mandatory pregnancy test before starting in all women of reproductive age; reliable contraception 1 month before, throughout, and 1 month after course; India: iPledge equivalent system not legally mandated but clinically practiced at responsible centres; monthly liver function + lipid monitoring (isotretinoin raises triglycerides, LFTs); side effects: dry lips (Vaseline — ₹50), dry eyes, photosensitivity, mood monitoring (controversial depression link — monitor); isotretinoin and night driving: visual impairment in low light — relevant for Indian patients who drive motorcycles at night | Isotretinoin 10mg (Sotret, Sanciret generic): ₹8–15/capsule; 80kg patient × 1mg/kg/day × 6 months ≈ ₹15,000–25,000 total (very affordable vs UK/USA) |
| Hormonal Acne (Adult women) | Persistent adult female acne: lower face/jawline/chin; cyclically worsening pre-menstrually; PCOS association | Anti-androgens: combined oral contraceptive pill (COCP — ethinylestradiol + cyproterone acetate: Diane-35; or EE + norgestimate; or EE + drospirenone: Yasmin/Yaz); reduces androgen-driven sebum; effective for hormonal/jawline acne in women not planning pregnancy; alternative: spironolactone 50–100mg/day (off-label anti-androgen — not COCP — aldosterone antagonist with anti-androgen effect; excellent for hormonal acne; monitor potassium/BP; contraindicated in pregnancy) | India PCOS-acne nexus: 25–30% Indian women with adult female acne have underlying PCOS (hyperandrogenism); screen with LH:FSH ratio, testosterone level, pelvic USS in resistant hormonal acne; treat PCOS underlying cause (metformin for insulin resistance + COCP for acne/hirsutism + lifestyle); COCP: Diane-35 ₹150–300/month; spironolactone generic: ₹50–100/month | Diane-35 (cyproterone+EE): ₹150–300/month; Spironolactone 100mg generic: ₹60–120/month |
Frequently Asked Questions
Why does acne leave dark marks on Indian skin — and how to treat them?
Post-inflammatory hyperpigmentation (PIH) — the dark brown or grey marks that remain after an acne lesion heals — is one of the most distressing aspects of acne for Indian patients with darker skin tones (Fitzpatrick III–VI) and frequently the primary concern that drives them to seek treatment: Why PIH is worse in Indian skin: Darker Fitzpatrick types have more melanin (melanocytes produce more melanin basally and respond more intensely to inflammatory stimuli); UV exposure (India’s intense tropical sun) dramatically worsens and prolongs PIH; PIH can last 6–24 months even after acne resolves without treatment; scratching and picking acne lesions dramatically worsens PIH and causes post-inflammatory erythema. Evidence-based PIH treatments: Azelaic acid 15–20% (first-line for PIH in acne — dual action: reduces active acne AND fades PIH; safe for longer-term use; minimal side effects; safe in pregnancy); Topical retinoids (adapalene/tretinoin): promotes skin cell turnover → fades PIH; requires 3–6 months of consistent use; photosensitising (SPF mandatory — especially India); Niacinamide 4–10% (inhibits melanosome transfer from melanocytes to keratinocytes → reduces PIH; OTC; well-tolerated; multiple Indian brands — Minimalist niacinamide 10% serum ₹300; The Derma Co 10% niacinamide ₹400); Vitamin C (L-ascorbic acid): antioxidant → inhibits tyrosinase → reduces melanin; combine with niacinamide; SPF essential; Alpha hydroxy acids (AHA — glycolic acid, lactic acid): chemically exfoliate → accelerate PIH fading; 5–10% OTC; 20–70% chemical peels at dermatologist; Chemical peel (India dermatology): glycolic acid 30–70% or salicylic-mandelic acid peels; effective PIH treatment; professional clinics ₹1,000–3,000/session × 4–6 sessions. What does NOT work and makes PIH worse: Topical steroid creams for dark marks (hydrocortisone, betamethasone on face for PIH): commonly self-applied in India seeking quick whitening → steroid-induced skin atrophy, perioral dermatitis, telangiectasia, and rebound darkening — a major and growing India-specific problem; topical mercury-containing “fairness creams” (banned but still available through unregulated online platforms): nephrotoxic; neurotoxic; avoid completely; sun exposure without sunscreen: UV stimulates melanin → dramatically worsens and prolongs PIH.
Is isotretinoin safe — what are the real risks?
Isotretinoin (oral retinoid — vitamin A derivative) is the most effective acne treatment available — but surrounded by fear, misinformation, and under-prescribing in India that leaves thousands of patients with severe scarring acne untreated: What isotretinoin does — the evidence: 80–90% of patients achieve sustained remission after a single course (120–150mg/kg cumulative dose); no other acne treatment approaches this level of long-term efficacy; normalises all four pathogenic mechanisms simultaneously (sebum ↓90%, keratinisation normalised, C. acnes reduced indirectly, inflammation ↓); acne scars continue to improve for 6–12 months after completing isotretinoin (post-inflammatory remodelling). Real risks of isotretinoin — evidence-based: Teratogenicity: ABSOLUTE contraindication in pregnancy — causes skeletal, cardiac, CNS defects in virtually all exposed fetuses; mandatory: negative pregnancy test before starting; two forms of contraception during and 1 month after; this is the ONE non-negotiable risk; Dry skin/lips: extremely common (80–90%); manage with emollient (CeraVe, white soft paraffin), Vaseline for lips; Dry eyes: troublesome for contact lens wearers — switch to glasses during course; Raised triglycerides/LFTs: monitor baseline + monthly; usually mild; stop only if very elevated; Photosensitivity: sunscreen SPF50 mandatory — particularly important in India; Night vision impairment: rare — advise about night driving. The depression controversy: Earlier concerns about isotretinoin causing depression/suicide have been extensively studied — large meta-analyses and pharmacovigilance data do NOT confirm causal link; acne itself (especially severe scarring acne) causes depression independently; isotretinoin improving acne actually often improves mood; however: monitor mood changes during isotretinoin; if depression develops (which may be coincidental) discuss with dermatologist/psychiatrist; do not routinely withhold isotretinoin for severe scarring acne due to depression risk. Who should prescribe isotretinoin in India: Licensed dermatologist only; India: isotretinoin available as generic (Sotret, Sanciret, Tretin — ₹8–15/capsule vs ₹50–100 in UK for Roaccutane brand); most effective and affordable treatment for severe acne available anywhere in the world when accessed through a responsible dermatologist.
What to Read Next
- PCOS — PCOS-Driven Hormonal Acne: Lower Face/Jawline Pattern; Treat with COCP (Diane-35) or Spironolactone + Metformin for IR
- Psoriasis & Eczema — Distinguish Acne from Rosacea, Perioral Dermatitis (Topical Steroid Overuse) and Folliculitis
- Atopic Dermatitis — Atopic March: Eczema Often Accompanies Acne-Prone Skin; Shared Skin Barrier Impairment
- Depression — Severe Acne Causes Clinically Significant Depression in Adolescents; Treat Acne Aggressively to Prevent Psychological Sequelae
- PCOD/PCOS — Hyperandrogenism Drives Sebaceous Gland Overactivity; Screen All Adult Female Acne for PCOS
An 18-year-old in Bengaluru with moderate acne buys a fairness cream from a pharmacy. It contains betamethasone. Her acne briefly clears (steroid anti-inflammatory effect). Then returns worse. She uses more of it. After 6 months she has steroid-induced perioral dermatitis, severe PIH from steroid-worsened acne, and skin atrophy. The original acne could have been cleared in 12 weeks with adapalene 0.1% gel (₹150) and benzoyl peroxide (₹120). The avoidable harm came from a ₹200 OTC cream. Unrestricted OTC access to topical steroids is one of the most significant drivers of dermatological harm in India today.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on IADVL Acne Guidelines 2023, American Academy of Dermatology Acne Guidelines 2016 (updated 2024), and Global Alliance to Improve Outcomes in Acne (GAIA) recommendations. Last updated: March 2026.
🧴 Retinoid + BPO = The Acne Foundation: For any acne beyond very mild, use adapalene 0.1% gel (₹150) nightly + benzoyl peroxide 2.5% gel (₹120) in the morning. These two topicals address all four pathogenic mechanisms, prevent antibiotic resistance, and work for 6–8 weeks before stopping. This ₹270 combination outperforms most expensive branded creams.
⚠️ Stop Using Steroid Creams for Acne or Dark Marks: Any cream labelled “fairness”, “whitening”, or “anti-acne” that contains betamethasone, clobetasol, or any corticosteroid will make your acne and dark marks dramatically worse over weeks to months. Check the ingredients label. If it contains any steroid on the face, stop immediately and consult a dermatologist.
⚕️ Medical Disclaimer: This article provides general educational information about acne vulgaris. Isotretinoin must be prescribed by a licensed dermatologist with mandatory pregnancy testing in women of reproductive age. Hormonal acne treatment options require individual assessment.
