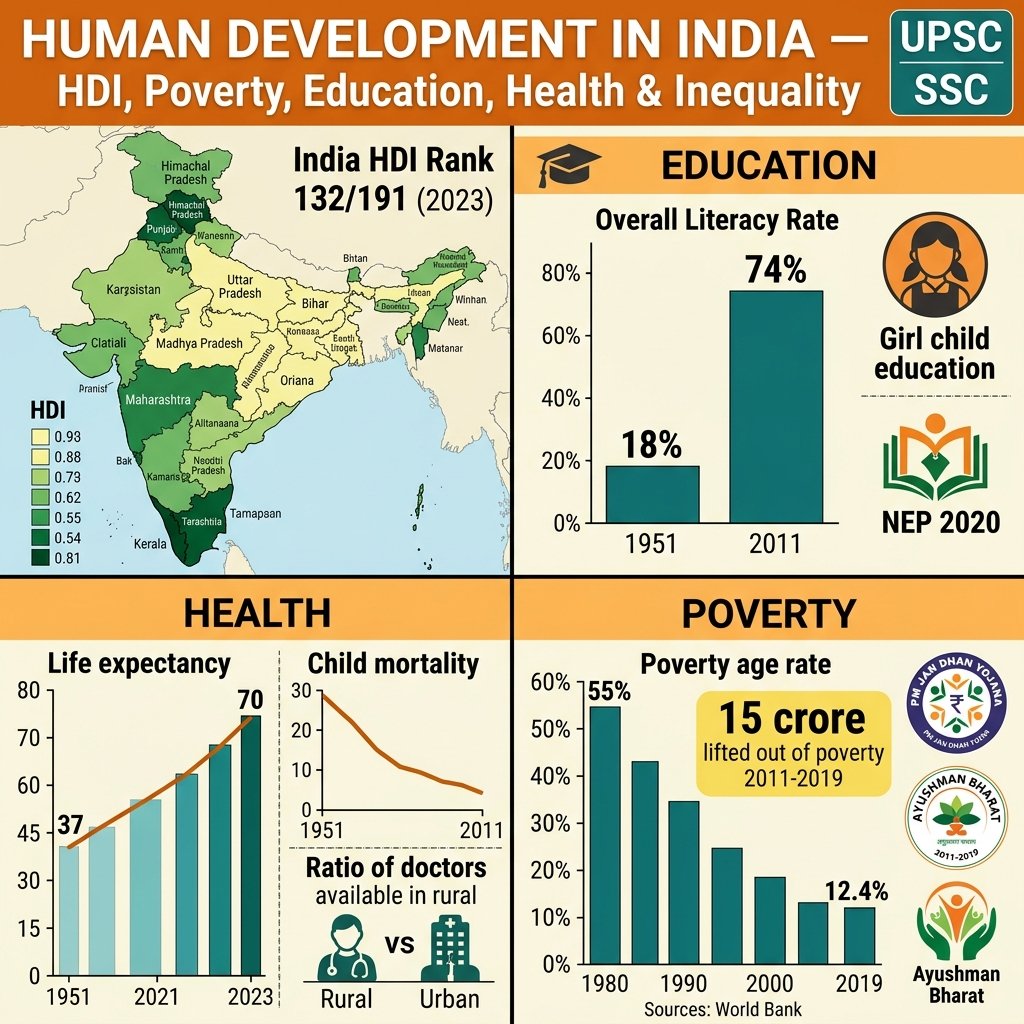
Human development is the process of expanding people’s freedoms and opportunities to live lives they have reason to value — health, education, and a decent standard of living. India’s human development story since 1947 is simultaneously one of remarkable achievement and deeply troubling inequality. Life expectancy has doubled (37 years in 1951 to 70.8 years in 2021); literacy has quadrupled (18% to 77%); child mortality has fallen dramatically (IMR: 146 to 28 per 1,000 live births); and between 2005–06 and 2019–21 alone, India lifted an estimated 415 million people out of multidimensional poverty — the largest and fastest poverty reduction in human history. Yet India ranks 132nd out of 193 countries on the UNDP Human Development Index (HDI 2023) — below Sri Lanka (78), China (75), and Bhutan (125). Within India, the gap between Kerala (HDI comparable to a middle-income East European nation) and Bihar (HDI comparable to sub-Saharan Africa) is wider than the gap between many pairs of countries. Understanding India’s human development profile, poverty measurements, social sector programmes, and regional disparities is critical for UPSC, SSC, and all competitive examinations.
Human Development Index (HDI) — India’s Position
- 📊 India’s HDI (2023 Report, data 2022): 0.644 = Rank 132/193; categorised as Medium Human Development; India’s HDI has risen continuously (0.345 in 1990 to 0.644 in 2022 = 86.6% improvement) but ranking has improved more slowly because other countries also improved
- 🧮 HDI = three dimensions: (1) Long and healthy life = Life Expectancy Index; (2) Knowledge = Education Index (Mean Years of Schooling + Expected Years of Schooling); (3) Decent standard of living = GNI per capita (PPP $)
- 📍 India’s HDI sub-indices (2022): Life Expectancy = 67.7 years (HDI calculator uses GNI-adjusted); Mean Years of Schooling = 6.57 years; Expected Years of Schooling = 11.9 years; GNI per capita = $8,475 PPP
| Country / State | HDI Score | Global Rank / Context | Life Expectancy | Mean Schooling Years |
|---|---|---|---|---|
| 🌍 Sri Lanka | 0.780 | Rank 78 — High HD | 77.0 | 10.3 |
| 🌍 China | 0.788 | Rank 75 — High HD | 78.2 | 8.1 |
| 🌍 Bhutan | 0.681 | Rank 125 — Medium HD | 72.5 | 5.7 |
| 🇮🇳 India (national) | 0.644 | Rank 132 — Medium HD | 67.7 | 6.57 |
| Kerala (state HDI est.) | ~0.775 | ~Equivalent to global rank ~80 | 77.3 | ~9.0 |
| HP / Punjab | ~0.720 | ~Equivalent to global rank ~105 | 73–74 | ~8.0 |
| UP / Rajasthan | ~0.590 | ~Equivalent to global rank ~150 | 65–67 | ~5.5 |
| Bihar (lowest) | ~0.574 | ~Equivalent to sub-Saharan Africa | 68.1 | ~4.7 |
Poverty in India — Multiple Dimensions
Poverty Lines & Measurement
- 💰 World Bank Extreme Poverty Line: $2.15/day (2022 PPP); India’s extreme poverty rate: ~12.9% in 2021 (World Bank); ~228 million people below extreme poverty; note: India disputes some methodology but uses similar concept
- 💰 Government of India Poverty Line: Based on caloric adequacy — historically Tendulkar Committee (2009) set line at ₹816/month rural and ₹1,000/month urban (2011–12 prices); Rangarajan Committee (2014) revised upward; official BPL (Below Poverty Line) population is contentious
- 📊 Official poverty rate trend (Planning Commission/NITI Aayog): 45.3% (1993–94) → 37.2% (2004–05) → 21.9% (2011–12); decline accelerated post-2005
- 🌐 MPI (Multidimensional Poverty Index): UNDP/Oxford measure covering 10 indicators across health, education, and living standards; India’s MPI: 16.4% (2021 NFHS-5 data) = ~228 million multidimensionally poor; 415 million lifted out of MPI poverty between 2005–06 and 2019–21 = largest and fastest reduction globally (UNDP 2023 MPI Report)
Poverty — State-level Disparities
| State | MPI Poor % (2019–21) | Key Challenge |
|---|---|---|
| Bihar | 51.9% (highest) | High fertility, low literacy, limited industry, poor infrastructure |
| Jharkhand | 42.2% | Mineral-rich but Adivasi communities locked out of resource benefits |
| UP | 37.8% | Large population, low female LFPR, poor urban services |
| Rajasthan | 33.0% | Improving rapidly; desert geography constraints |
| MP | 36.6% | Large tribal population; low industrialisation |
| Kerala | 0.71% (lowest) | Model state — high education, health, social mobility |
| Goa | 1.7% | Tourism economy, small population |
| Punjab / HP | ~5–7% | Relatively prosperous; agriculture + tourism income |
| All India | 16.4% | Dramatic improvement from 55.1% (2005–06) to 16.4% (2019–21) |
Education in India
- 📚 Literacy: India national literacy rate = 74.0% (Census 2011); Male 82.1%, Female 65.5%; target: 100% functional literacy by 2030 under India’s commitment to SDG 4
- 📚 State literacy extremes: Kerala = 94.0% (highest, Census 2011); Rajasthan = 66.1%; Bihar = 63.8%; Jharkhand = 66.4%; lowest female literacy states: Rajasthan (52.7%), Bihar (53.3%), Jharkhand (56.2%)
- 📚 Gross Enrolment Ratio (GER): Primary (Class 1–5) = ~100% (universalised); Upper Primary (6–8) = ~92%; Secondary (9–12) = ~56%; Higher Education GER = 28.4% (2021–22); target 50% GER higher education by 2035 (NEP 2020)
- 📚 National Education Policy (NEP) 2020: Biggest overhaul since 1986 NPE; key changes: (1) 5+3+3+4 school structure replacing 10+2; (2) Mother tongue instruction till Class 5; (3) Academic Bank of Credits (ABC) for multiple entry-exit in higher education; (4) Multidisciplinary universities replacing single-stream colleges; (5) 6% GDP target for education; (6) Vocational education from Class 6; (7) Coding from Class 6
- 📚 Right to Education (RTE) Act 2009: Free and compulsory education for children 6–14 years; 25% reservation in private schools for EWS/disadvantaged group children; currently facing implementation challenges (learning outcomes — ASER report consistently shows 50%+ Class 5 children cannot read Class 2 text)
- 📚 ASER (Annual Status of Education Report): Civil society survey; consistently reveals the gap between enrolment (high) and learning outcomes (poor); ASER 2023 found 73.3% Class 8 students in rural India could do basic division — improvement from previous years
Health in India
| Health Indicator | 1951 | 2011 | 2020–23 | Target / Comparator |
|---|---|---|---|---|
| Life Expectancy (years) | 37 | 67.5 | 70.8 (2019–21) | 75 by 2030 (NHP 2017) |
| Infant Mortality Rate (per 1,000) | 146 | 44 | 28 (SRS 2020) | <12 by 2030 (SDG) |
| Maternal Mortality Ratio (per 100,000) | ~2,000 | 212 | 97 (SRS 2018–20) | <70 by 2030 (SDG) |
| Under-5 Mortality Rate (per 1,000) | ~250+ | 59 | 32 (NFHS-5) | <25 by 2030 (SDG) |
| Stunting in children under 5 | — | ~48% | 35.5% (NFHS-5) | Declining but still very high |
| Anaemia in women (15–49 yrs) | — | ~55% | 57.0% (NFHS-5) = worsened! | WHO target 50% by 2025 |
| Full vaccination coverage (children) | — | ~44% | 76.4% (NFHS-5) | 90% by 2030 |
| Public health expenditure (% GDP) | — | ~1.0% | 2.1% (2022–23) | 2.5% target (2025–26 Budget) |
- 🏥 Kerala Model of Health: Kerala achieves life expectancy (77.3 years) and IMR (7 per 1,000) comparable to developed nations at a per capita income far below them. The “Kerala paradox” — low income, high health outcomes — is explained by: (1) High female literacy leading to better child health practices; (2) Strong public health infrastructure (public health centres, district hospitals free at point of use); (3) Low fertility (TFR 1.8); (4) Community health tradition; (5) Remittances from Gulf diaspora funding private health purchases. Kerala is the global template for achieving health outcomes through social development rather than income alone.
- 💊 Ayushman Bharat — PM-JAY: Pradhan Mantri Jan Arogya Yojana (2018) — world’s largest government-funded health insurance scheme; covers 50 crore beneficiaries (bottom 40% income); ₹5 lakh per family per year hospitalisation cover; cashless treatment at empanelled public and private hospitals; 30,000+ hospitals empanelled; 6 crore+ hospital admissions by 2024; financed jointly by Centre (60%) and States (40%)
- 🏥 Ayushman Bharat — Health & Wellness Centres (HWCs): 1.5 lakh Sub-Centres and Primary Health Centres converted to HWCs providing comprehensive primary care (NCD screening, mental health, maternal health, AYUSH integration)
- 🩺 India’s doctor-patient crisis: India has 1 doctor per 1,445 people (WHO recommends 1:1,000); in rural India this falls to 1 doctor per ~5,000+ people; 75% of doctors practise in urban areas serving 35% of population; rural doctor deployment remains one of India’s most intractable health system challenges
Gender Development & Inequality
- 👩 Gender Development Index (GDI): India’s GDI = 0.849 (2022); Female HDI = 0.615 vs Male HDI = 0.669 — significant gender gap in human development
- 👩 Gender Inequality Index (GII): India ranked 108/166 (2023); measures reproductive health, empowerment, and labour market; reproductive health (MMR, adolescent birth rate) remains India’s biggest GII drag
- 👩 Female Labour Force Participation Rate (FLFPR): India = ~25% (2022–23) — among the lowest in the world for India’s income level; declined from ~36% (2004–05) to ~23% (2017–18) before recovering; reasons for decline: rising female education keeping young women out of low-quality jobs; social norms; lack of safe workplaces; inadequate childcare; mismatch between jobs available and women’s aspirations
- 👩 Important gender schemes: Beti Bachao Beti Padhao (save daughter, educate daughter) — targets declining child sex ratio (CSR was 918 per 1,000 males in 2011); Sukanya Samriddhi Yojana (girl child savings scheme); PM Matru Vandana Yojana (maternity benefit ₹6,000); One Stop Centres (Sakhi Centres) for violence against women; Ujjwala Yojana (free LPG = reduced women’s kitchen drudgery)
Key Social Sector Schemes — Quick Reference
| Scheme | Launch | Target | Key Numbers |
|---|---|---|---|
| PM-JAY (Ayushman Bharat) | 2018 | 50 crore beneficiaries; ₹5 lakh hospitalisation cover/family | 6 crore+ admissions; world’s largest health insurance |
| PM Garib Kalyan Anna Yojana (PMGKAY) | 2020 | 81 crore beneficiaries; free foodgrain (5 kg/person/month) | Extended 5 years (2024–28); ₹2 lakh crore/year cost |
| PM Awas Yojana (Gramin) | 2016 | 2.95 crore rural houses for homeless | 2.6 crore houses completed by 2024 |
| PM Awas Yojana (Urban) | 2015 | Urban housing for EWS/LIG/MIG | 1.18 crore houses sanctioned; ~75% complete |
| Jal Jeevan Mission | 2019 | Tap water to all 19.4 crore rural homes by 2024 | 14.8 crore connections made by 2024 (76%) |
| PM Ujjwala Yojana | 2016 | Free LPG to BPL women; 10 crore target | 10.35 crore connections; reduced indoor air pollution |
| PM Jan Dhan Yojana (PMJDY) | 2014 | Bank account for every household | 52 crore accounts (2024); 55% women account holders |
| Swachh Bharat Mission | 2014 | ODF (Open Defecation Free) India; 10 crore toilets rural | 11.5 crore toilets built; rural ODF claimed by 2019 |
| MGNREGA | 2005 | 100 days guaranteed employment to rural households | ~9 crore households employed annually; ₹89,000 crore budget (2023–24) |
| Mid-Day Meal / PM Poshan | 1995 (expanded 2001) | Free cooked meal to 12 crore+ school children | Largest school feeding programme in world; linked to school enrolment rise |
⭐ Important for Exams — Quick Revision
- 🔑 India HDI 2023: 0.644; Rank 132/193; Medium Human Development; below Sri Lanka (78), China (75), Bhutan (125)
- 🔑 HDI three dimensions: Life expectancy (health) + Education (mean + expected schooling years) + GNI per capita (income)
- 🔑 MPI (Multidimensional Poverty): India 16.4% (2019–21); 415 million lifted out of poverty (2005–21) = world’s largest and fastest
- 🔑 Bihar = highest MPI poverty (51.9%); Kerala = lowest (0.71%)
- 🔑 World Bank extreme poverty: $2.15/day; India ~12.9% (2021)
- 🔑 HDI state extremes: Kerala (~0.775) vs Bihar (~0.574); gap comparable to different countries
- 🔑 Literacy: 74% national (Census 2011); Kerala highest (94%); Bihar lowest (63.8%); female literacy gap = 16.6 points
- 🔑 NEP 2020: 5+3+3+4 structure; mother tongue till Class 5; multiple entry-exit; 6% GDP target
- 🔑 RTE Act 2009: Free compulsory education 6–14 years; 25% EWS reservation private schools
- 🔑 ASER: Annual education survey; shows learning outcome crisis — 50%+ Class 5 cannot read Class 2 text
- 🔑 Anaemia in women = 57% (NFHS-5) — worsened from NFHS-4; stunting 35.5%; vaccination 76.4%
- 🔑 MMR India = 97 (SRS 2018–20); down from 2,000 (1951); Kerala MMR = 19 (lowest); UP/Bihar = 150+ (highest)
- 🔑 PM-JAY (2018): World’s largest health insurance; 50 crore beneficiaries; ₹5 lakh cover
- 🔑 India doctor-patient ratio = 1:1,445 (WHO recommends 1:1,000); 75% doctors in urban areas
- 🔑 FLFPR India ~25% = among world’s lowest for India’s income level; key barrier to demographic dividend
- 🔑 PMJDY (2014): 52 crore bank accounts; 55% women; foundation of DBT (Direct Benefit Transfer)
- 🔑 Jal Jeevan Mission (2019): Tap water to all rural homes; 76% complete (14.8 crore of 19.4 crore)
- 🔑 Kerala Model: High HDI at low per capita income = proof education + health can precede income growth
Frequently Asked Questions (FAQs)
1. Why does India rank 132nd on HDI despite being the world’s 5th largest economy?
This question goes to the heart of the distinction between economic growth and human development — a distinction that Amartya Sen’s capability approach and Mahbub ul Haq’s HDI framework were specifically designed to make. India’s GDP (nominal, 2024) of ~$3.7 trillion makes it the world’s 5th largest economy in aggregate terms. Yet its rank of 132 on the HDI places it in the “medium human development” category, below much smaller or poorer nations. The explanation lies in three structural realities. First, GDP per capita tells a very different story from aggregate GDP. India’s per capita GNI is ~$8,475 (PPP) — when converted back to actual purchasing power for the median Indian, this represents a distinctly middle-low income. India’s large aggregate GDP reflects its enormous 1.44 billion population — divide that GDP by the population, and the average Indian’s income is far more modest than that of citizens of countries ranked above India. Second, India’s income inequality is severe and rising. The aggregate GDP captures headline growth, but India’s Gini coefficient (~0.35–0.38 by income, higher by wealth — Oxfam estimates suggest the top 1% hold 40% of national wealth) means the gains from growth have been disproportionately captured by the top segments. HDI, by contrast, captures outcomes — life expectancy, actual schooling years, actual incomes — which reflect what the middle and bottom of India’s distribution experience, not the wealthy top. Third, public investment in health and education has been historically low, limiting human capital accumulation. India spends ~2.1% of GDP on public health (WHO recommends 5%) and ~2.9% of GDP on education (NEP 2020 targets 6%); by comparison, Sri Lanka (ranked 78) spends ~1.6% of GDP on health but has historically had excellent primary health systems and near-universal literacy. The Kerala example within India is instructive: Kerala, with a per capita GSDP similar to the Indian average for decades, achieved HDI outcomes comparable to developed nations — demonstrating that it is how a society invests (especially in women, primary education, public health) rather than how much it earns that determines human development. The good news is that India’s trajectory is strongly upward — since 1990, India’s HDI has improved by 86.6%, one of the largest improvements globally; the challenge is that the starting base was so low that significant catch-up remains needed.
2. What is the “Kerala Model” and can Bihar replicate it?
The Kerala Model refers to Kerala’s achievement of human development outcomes (life expectancy ~77 years, literacy ~94%, IMR ~7 per 1,000, TFR 1.8) that are comparable to European middle-income nations, despite a per capita income that was, for most of Kerala’s developmental history, only comparable to the Indian average. The model is frequently cited internationally as proof that human development does not require prior income growth — that the sequence can be reversed: invest in education and health first, and income growth follows. What created the Kerala Model? Multiple complementary factors reinforced each other over generations: (1) Historical legacy of education: Kerala’s princely states of Travancore and Cochin had compulsory primary education laws as early as the 1840s — a full century before the rest of India. Christian missionaries (especially London Missionary Society), and then Sree Narayana Guru’s reform movement among lower castes, further expanded access to education for historically marginalised communities. By Independence, literacy was already ~47% — far above the national 18%. (2) Land reforms (1969–1970): Kerala’s landmark Land Reforms Act was one of India’s most comprehensive redistributions — it effectively eliminated large zamindari estates and spread economic security among small landholders, reducing the extreme poverty that hampers human development elsewhere. (3) Strong public health system: Kerala developed an extensive Primary Health Centre network (one of India’s densest, relative to population) with genuinely functioning services — not just buildings on paper. (4) Women’s empowerment: Kerala’s matrilineal tradition in several communities (Nair community historically practiced marumakkathayam — inheritance through the female line), combined with missionary education access for girls, created high female literacy and educational attainment that breaks the intergenerational poverty cycle (educated mothers have fewer, healthier, better-educated children). (5) Kudumbashree: Kerala’s unique community network of 4.5 million women’s self-help groups providing microfinance, enterprise support, and social solidarity at the neighbourhood level. Can Bihar replicate it? Directly transplanting is unlikely — Kerala’s model was path-dependent, built over 150+ years of historically unique conditions. But the lessons can be applied: (1) Invest in girls’ education comprehensively, not incrementally; (2) Build genuinely functional primary health systems rather than aspirational targets; (3) Implement land and social reform to break the asset inequality that perpetuates poverty cycles; (4) Address the political economy of caste — Bihar’s caste hierarchy historically controlled access to education and economic opportunity for scheduled castes and tribes. Bihar is improving (TFR falling, MMR declining, Jal Jeevan Mission making progress), but from such a low base that catching up meaningfully requires sustained, multi-decade investment across all human development pillars simultaneously.
3. Does Swachh Bharat Mission actually work — and what is the evidence on open defecation and health outcomes?
The Swachh Bharat Mission (SBM) — launched on Gandhi Jayanti (October 2, 2014) — set out to build 10 crore toilets in rural India and achieve Open Defecation Free (ODF) status for all villages by October 2019. By the government’s own account, 11.5+ crore toilets were built and India was declared ODF rural by 2019. But as with many large-scale sanitation programmes globally, the relationship between toilet construction, toilet use, and health outcomes is complex and contested. What the evidence shows: A landmark randomised controlled trial by WASH Benefits India (2018, published in Lancet Global Health) studied sanitation behaviour across 2,335 rural villages in Bihar and UP. The study found that SBM toilet construction, in its early phase in these states, did not significantly improve child height-for-age (stunting), the primary outcome expected from reduced open defecation. However, this study captured an early phase when toilet construction had outrun sustained behaviour change; follow-up research in villages with high toilet use found clearer benefits. A different perspective comes from NFHS-5 (2019–21): rural household toilet access rose from 38.7% (NFHS-4, 2015–16) to 70.2% (NFHS-5) — a dramatic improvement in infrastructure. The critical challenge is toilet use not just construction: in 2012, SQUAT Survey found that 40% of households that had toilets had at least one member still defecating in the open — due to preferences (perceived openness, freshness), functionality of toilet (pit full, no water), and social norms. The government’s SBM Phase II (2020–25) therefore focused less on construction and more on ODF Sustainability and ODF Plus — ensuring existing toilets are functional, used consistently, and that solid/liquid waste management is addressed. The evidence from India and globally is clear that consistent, universal toilet use does reduce diarrhoeal disease mortality significantly — but achieving consistent use requires sustained behaviour change communication, community-led total sanitation approaches, and functioning water supply (toilet use drops dramatically when there is no running water for flushing/cleaning). The Jal Jeevan Mission’s focus on household tap water connections is therefore directly complementary to SBM’s sanitation goals. India’s infant and child mortality decline since 2014, while not attributable solely to SBM, is consistent with improvements in sanitation access being one contributing factor alongside nutrition, vaccine coverage, and maternal health improvements.
Related Geology Articles on StudyHub
- ➡️ Population India — Demographic Dividend & Growth
- ➡️ Agriculture India — Food Security & Farmer Welfare
- ➡️ Transport India — Infrastructure for Human Mobility
- ➡️ Water Resources — Jal Jeevan Mission Context
- ➡️ Wildlife Conservation — Human-Nature Balance
