Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
“Arthritis” is not a single disease — it is an umbrella term covering over 100 different joint conditions. In India, an estimated 180–200 million people suffer from some form of arthritis — making it one of the leading causes of disability, lost workdays, and reduced quality of life. Yet arthritis is routinely dismissed as inevitable “old age joint pain” that nothing can be done about. This is dangerously wrong. The two most important types — Osteoarthritis and Rheumatoid Arthritis — are fundamentally different in cause, mechanism, affected joints, and treatment. Understanding the difference determines whether the correct treatment prevents joint destruction or allows irreversible disability to develop silently.
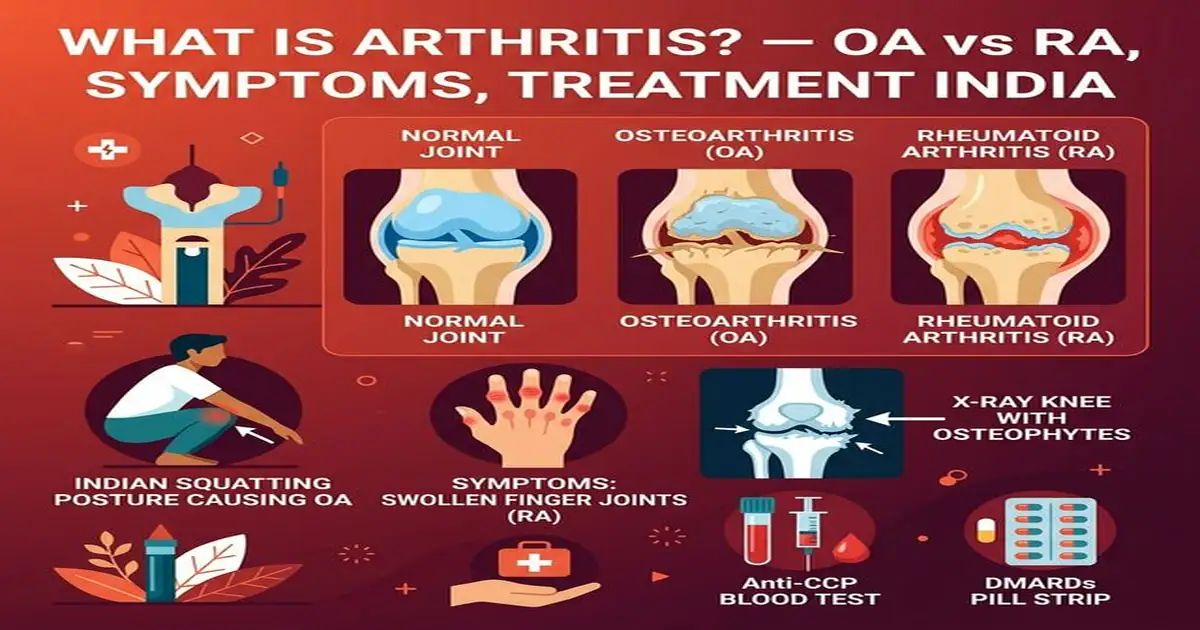
Osteoarthritis vs Rheumatoid Arthritis — Key Differences
| Feature | Osteoarthritis (OA) | Rheumatoid Arthritis (RA) |
|---|---|---|
| Mechanism | Mechanical wear — cartilage degenerates from overuse, obesity, injury; bone-on-bone grinding; osteophyte (bone spur) formation | Autoimmune — immune system attacks synovial membrane (pannus formation); inflammation destroys cartilage and bone |
| Joints affected | Weight-bearing joints: knees, hips, spine (L4–L5), hands (DIP joints — distal interphalangeal) | Small joints of hands (MCP, PIP — knuckles), wrists, feet (MTP joints); symmetric (both sides simultaneously); spares DIP joints |
| Age of onset | Usually >50 years; directly age-related | Any age; peak 30–50 years; can occur in children (JIA) |
| Morning stiffness | Brief (<30 minutes) — improves with movement (gelling phenomenon) | Prolonged (≥1 hour) — signature RA symptom; getting up in morning is most difficult |
| Systemic symptoms | None — purely joint disease | Yes — fatigue, weight loss, anaemia, fever; can affect lungs, heart, eyes (extra-articular RA) |
| Blood tests | Normal CRP/ESR; X-ray: joint space narrowing + osteophytes | Elevated CRP/ESR; RF (Rheumatoid Factor) positive in 70%; anti-CCP positive in 80% (most specific) |
| Treatment goal | Pain relief + function; joint replacement for severe OA | Disease control with DMARDs — to prevent joint destruction; methotrexate first-line |
Osteoarthritis — India’s Knee Epidemic
India has the highest prevalence of knee osteoarthritis in the world — estimated at 28–45% in adults over 60 and rising rapidly with urbanisation and obesity. India-specific factors driving this epidemic: squatting and cross-legged sitting (culturally universal in India — used for daily activities, prayer, cooking) places 7–8× body weight force on the knee joint, dramatically accelerating cartilage wear; obesity — each 1 kg of weight gain adds 4 kg of force on the knee; a 10 kg weight gain increases knee OA risk by 36%; agricultural work — repetitive kneeling, lifting, and walking on uneven terrain; low dietary calcium and Vitamin D — poor bone quality worsens cartilage and subchondral bone health. OA does not just affect the elderly — the Indian OA patient is getting younger with rising obesity rates.
Rheumatoid Arthritis — Diagnosis and the Window of Opportunity
India has an estimated 10 million RA patients — but the most critical message is timing: the first 3–6 months of RA is the “window of opportunity” — during which starting methotrexate (the first-line DMARD) can prevent virtually all joint destruction and achieve clinical remission. After this window, established pannus and cytokine-driven damage becomes harder to control, and radiological joint erosions develop that are irreversible. Warning signs of early RA — see a rheumatologist immediately if: morning stiffness over 1 hour for >6 weeks; swelling of 3+ joints simultaneously; small joint involvement (knuckles, wrists, ball of foot); bilateral and symmetric distribution; associated fatigue. Anti-CCP is the most specific test — positive in 80% of RA and can precede symptoms by years.
Treatment of Arthritis in India
| Treatment | OA | RA | India Specifics |
|---|---|---|---|
| NSAIDs (ibuprofen, diclofenac, etoricoxib) | ✅ First-line for pain; use lowest effective dose for shortest duration; gastroprotection (pantoprazole) with chronic use | ✅ Adjunct for pain/inflammation; NOT disease-modifying | Widely overused chronically in India without gastroprotection → GI bleeding; also nephrotoxic in CKD |
| Methotrexate | ❌ Not used | ✅ Gold standard first-line DMARD — 7.5–25mg weekly oral; reduces joint destruction, improves function; requires folic acid 5mg/day supplementation; monitor LFTs and CBC | Very affordable in India (₹30–50/month); widely available; needs regular monitoring |
| Hydroxychloroquine (HCQ) | ❌ Not used | ✅ Safe adjunct DMARD; added to methotrexate in early RA; good in mild RA and lupus overlap | Requires annual eye check (maculopathy with long-term use) |
| Biologics (TNF inhibitors, IL-6 inhibitors) | ❌ Not applicable | ✅ For methotrexate-inadequate RA — adalimumab, etanercept, tocilizumab, baricitinib (JAK inhibitor) | Cost: ₹10,000–50,000/month; available at AIIMS/government rheumatology centres at reduced cost; some PM-JAY coverage |
| Intra-articular steroid injection | ✅ Very effective for acute flares — methylprednisolone or triamcinolone; 3–4 months pain relief; not more than 3–4/year per joint | ✅ For flares of specific joints while adjusting DMARDs | Very cost-effective (₹200–500); widely used at district hospitals |
| Total Knee Replacement (TKR) | ✅ Definitive for severe OA (Grade 3–4 on X-ray); bilateral in same sitting common in India; PM-JAY covers at empanelled hospitals | ❌ Only for end-stage RA destruction | Government hospitals: ₹50,000–1,20,000; private: ₹1,50,000–3,00,000; outcomes excellent |
| Weight loss (obesity OA) | ✅ Most impactful non-surgical intervention; 10% weight loss → 50% pain reduction in knee OA → delays or avoids TKR | Helpful for overall health | Central to India’s OA management given widespread obesity |
Other Important Arthritis Types in India
| Type | Key Feature | Indian Relevance |
|---|---|---|
| Gout | Uric acid crystal deposition in joints — big toe (first MTP) classic; intensely painful acute attacks; rising rapidly with high-purine diet + metabolic syndrome | Rising sharply in India — meat consumption, alcohol, metabolic syndrome; allopurinol is definitive prevention |
| Ankylosing Spondylitis (AS) | Autoimmune — primarily axial spine; young men; sacroiliac joint fusion; early morning back pain improving with exercise | HLA-B27 positive; often missed in India — misdiagnosed as “spondylitis” or “disc problem” for years |
| Psoriatic Arthritis | Arthritis associated with psoriasis skin disease; asymmetric; can affect spine and DIP joints; nail pitting | Co-exists with psoriasis; diagnosed late when skin manifestations not connected to joint disease |
| Reactive Arthritis | Arthritis triggered by infection (GI or GU) — Reiter’s syndrome; self-limiting 3–6 months | Common post-dysentery; post-STI (chlamydia) in India |
| Septic (Infectious) Arthritis | Bacterial infection of joint — medical emergency; destroys joint within 24–48 hours; TB arthritis common in India | Any sudden severe hot swollen single joint = emergency joint aspiration; TB joint common in endemic areas |
Frequently Asked Questions
Can arthritis be cured permanently?
The answer depends critically on which type of arthritis, and this distinction matters enormously for patient expectations and treatment motivation. Osteoarthritis: Cannot be cured — cartilage once lost does not regenerate with any currently approved treatment. However, OA can be very successfully managed: pain can be controlled, function maintained, and disease progression significantly slowed with weight loss, physiotherapy, appropriate analgesia, and timely joint replacement. Weight loss of 10% combined with exercise can reduce knee OA pain by 50% — a treatment result equivalent to many surgeries. Total knee replacement effectively “cures” the symptoms of end-stage knee OA — patients return to normal walking and activity within 3–6 months. Rheumatoid Arthritis: RA cannot be “cured” in the sense of permanent remission without medication — it is a lifelong autoimmune disease. However, modern DMARD therapy (methotrexate ± biologics) achieves drug-free remission in 10–15% of patients after 5 years of treatment, and sustainable low-disease activity in 50–60%. More importantly, early treatment (within 3–6 months of onset) prevents joint destruction — a patient who is never destroyed their joints is functionally equivalent to cured. Gout: The only truly curable arthritis — allopurinol (urate-lowering therapy) combined with dietary changes and hydration can keep uric acid below 6 mg/dL indefinitely → complete prevention of all future attacks → tophaceous deposition resolves over years. Gout is the arthritis where the word “cure” is most appropriately used. Reactive arthritis: Self-limiting — resolves in 3–6 months without joint destruction in most cases.
Is methotrexate safe for long-term use?
Methotrexate is the cornerstone of RA management worldwide — and the single most important drug in preventing joint destruction. The fear of methotrexate (“chemotherapy drug”) among Indian patients and their families is one of the most critical barriers to timely RA treatment. Important context: methotrexate is used at very different doses for different diseases: cancer (HIGH dose, 100× RA dose — where severe toxicity occurs); RA (LOW weekly dose, 7.5–25mg/week — a fraction of cancer doses). At RA doses, methotrexate has been used for 50+ years with an excellent safety profile when properly monitored. The main risks at RA doses: Hepatotoxicity — elevated liver enzymes, rarely significant fibrosis (especially with alcohol); prevented by avoiding alcohol + monitoring LFTs every 3 months. Bone marrow suppression — reduced blood cells (rare at low doses); prevented by folic acid 5mg/day (MUST be co-prescribed) + regular CBC monitoring. Pulmonary toxicity (MTX pneumonitis) — rare (<1%); presents as new breathlessness; drug is stopped immediately. Teratogenicity — absolutely contraindicated in pregnancy and for 3 months before conception; effective contraception essential in reproductive-age women. Monitoring schedule: LFTs + CBC + creatinine every 3 months for first year; every 6 months thereafter on stable doses. The risk of NOT treating RA with methotrexate — progressive joint destruction, deformity, disability, and cardiovascular mortality from systemic inflammation — enormously outweighs monitoring-addressable risks.
What exercises help arthritis joints?
Exercise is paradoxically one of the best treatments for arthritis — despite seeming that “resting the joint” is logical. For Osteoarthritis: Low-impact aerobic exercise (swimming, cycling, walking on flat surface, water aerobics) reduces OA pain and improves function more effectively than most medications — meta-analyses show exercise equivalent to NSAIDs for pain relief with zero side effects. Quadriceps strengthening is specifically evidence-based for knee OA — strong quadriceps reduce forces on the knee joint and protect remaining cartilage. Tai chi reduces balance and fall risk, and has specific RCT evidence for knee OA pain reduction. What to avoid in OA: High-impact activities (running, jumping, squatting), prolonged squatting and cross-legged sitting (particularly damaging in Indian setting). For Rheumatoid Arthritis: Exercise during remission is strongly encouraged — reduces cardiovascular risk (massively elevated in RA), improves muscle strength, prevents deconditioning. During active flares: gentle range-of-motion exercises only; avoid loading inflamed joints. Hydrotherapy (pool exercises) is particularly gentle for inflamed joints. Physiotherapy prescription for Indian arthritis: A rheumatology physiotherapist should prescribe a specific programme — generic “rest the joints” advice from GPs is outdated and harmful. The prescription: 30 minutes of low-impact exercise 5 days/week, as able with pain tolerance; quadriceps and hip abductor strengthening 2–3×/week; balance training for fall prevention.
Does diet affect arthritis?
Diet significantly affects arthritis through multiple mechanisms — weight management, systemic inflammation, and specific food-metabolism interactions. Anti-inflammatory diet (RA and OA): Mediterranean-pattern diet (olive oil, fish, legumes, vegetables, nuts, whole grains) is associated with lower RA disease activity and lower inflammatory markers (CRP, ESR) in multiple observational studies. Omega-3 fatty acids (EPA + DHA from fish oil 2–4g/day) have modest but real anti-inflammatory effects in RA — reduce morning stiffness and tender joint count by 25–30%; fish oil is a reasonable adjunct, not a replacement for methotrexate. Avoid (RA and OA): Ultra-processed food and refined sugars drive systemic inflammation; red meat (particularly processed) increases uric acid and inflammatory markers; alcohol in RA patients increases methotrexate hepatotoxicity risk — minimise or avoid. Foods with some evidence for arthritis (Indian context): Haldi (turmeric/curcumin) — 1,000mg curcumin supplements show modest anti-inflammatory effects in OA (equivalent to ibuprofen in some small Indian trials) though absorption is poor without piperine (black pepper). Ginger extract — moderate evidence for OA pain reduction. Amla (Indian gooseberry) — high Vitamin C, which is a collagen precursor; may support cartilage health. Gout diet is uniquely critical: Limit organ meat (liver, kidney), shellfish, sardines, yeast extract; avoid alcohol (especially beer — highest purine content); drink 3+ litres water; low-fat dairy actually REDUCES uric acid (uricosuric effect of lactalbumin). Diet alone rarely achieves target uric acid — allopurinol is almost always needed in established gout.
When is knee replacement needed and is it safe?
Total Knee Replacement (TKR) is indicated when knee OA has reached the stage where pain significantly impairs daily function, conservative management (physiotherapy, weight loss, injections, analgesics) has been maximally tried and failed, and X-ray shows Grade 3–4 OA (severe joint space loss ± bone-on-bone contact). TKR is NOT indicated based on X-ray grade alone — active patients with Grade 3 OA who function adequately do not automatically need surgery. Indications in India: inability to walk 500 metres without severe pain; inability to climb one flight of stairs; significant night pain; failure of 6–12 months of conservative management. Safety: TKR is a very safe and highly effective procedure in the hands of experienced surgeons. In-hospital mortality in India at major orthopaedic centres: <0.5%. Most significant risk: deep vein thrombosis and pulmonary embolism (blood clots) — prevented with short-term anticoagulation (rivaroxaban or enoxaparin) for 2–4 weeks post-procedure + early ambulation (walking day 2 post-surgery). The surgery success rate for pain relief: >90% of Indian patients report significant improvement in pain and walking at 1 year. Cost: Government hospitals ₹50,000–1,20,000 (imported implant fee waived at some centres); private hospitals ₹1,50,000–3,00,000; PM-JAY Ayushman Bharat covers TKR up to ₹90,000–1,20,000 at empanelled hospitals — check eligibility. Indian patients commonly ask about “bilateral TKR in same sitting” — performing both knees simultaneously; this is done routinely in India at high-volume centres with similar risk to unilateral, and saves hospitalisation time + overall cost by 30–40%.
What to Read Next
- Osteoporosis — OA and Osteoporosis Often Coexist; Both Need Bone Protection
- Vitamin D — Low VitD Worsens OA Pain and RA Disease Activity
- Cholesterol — RA Significantly Increases Cardiovascular Risk
- CKD — NSAIDs for Arthritis Are Nephrotoxic; Dose Carefully in Kidney Disease
- Fatty Liver — Obesity Drives Both NAFLD and Knee OA; Weight Loss Addresses Both
OA is a message from your knees: “the weight you carry is more than we were built for.” RA is a message from your immune system: “we have forgotten who the enemy is.” Both have answers. Both can be treated. The tragedy is when neither is treated — when pain is accepted as fate and a 55-year-old becomes housebound because they believed that nothing could be done.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on ACR (American College of Rheumatology) and EULAR guidelines, Indian Rheumatology Association guidelines, and Indian epidemiology data. Last updated: March 2026.
Authoritative Sources: ACR — American College of Rheumatology | EULAR — European Rheumatology Alliance | Indian Rheumatology Association | ICMR India
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Arthritis diagnosis requires clinical evaluation and specific blood tests (anti-CCP, CRP, ESR, uric acid). Never self-prescribe methotrexate or biologics. A sudden hot swollen single joint is a medical emergency. Consult a rheumatologist for RA management.
