Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
Fatty liver disease is now the most common liver disease in the world — and India is in the grip of a silent epidemic. Studies estimate that 9–32% of the general Indian population has non-alcoholic fatty liver disease (NAFLD), rising to over 50% in people with obesity and 70–80% in those with Type 2 diabetes. Most people with fatty liver have no symptoms at all for years — while fat accumulation gradually progresses toward inflammation, fibrosis, cirrhosis, and ultimately liver failure. The good news: fatty liver is one of the few progressive chronic diseases that can be completely reversed — but only if caught and acted upon early. This guide tells you everything you need to know.
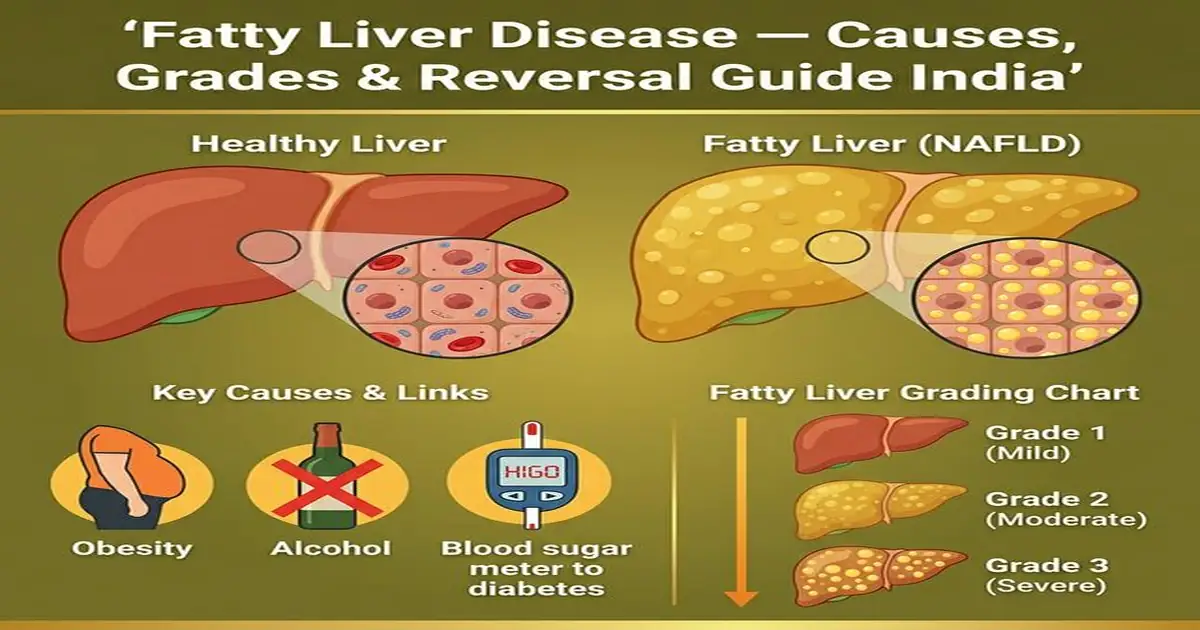
What is Fatty Liver Disease?
Fatty liver disease (medically termed hepatic steatosis) occurs when fat accounts for more than 5% of the liver’s weight. The liver is the body’s primary metabolic organ — processing everything you eat, filtering toxins, and producing proteins. When excess fat accumulates in liver cells (hepatocytes), it impairs these functions and triggers inflammation. There are two main types:
| Type | Cause | New Name (2023) | Prevalence in India |
|---|---|---|---|
| Non-Alcoholic Fatty Liver Disease (NAFLD) | Obesity, diabetes, metabolic syndrome — NOT alcohol | MASLD (Metabolic dysfunction-Associated Steatotic Liver Disease) | 9–32% general population; up to 80% in diabetics |
| Alcoholic Fatty Liver Disease (AFLD) | Chronic excess alcohol consumption | MetALD (when metabolic factors also present) | Significant but less common than NAFLD in India |
Fatty Liver Grades — From Mild to Severe
| Grade | Fat in Liver | Ultrasound Finding | Liver Damage | Reversible? |
|---|---|---|---|---|
| Grade 1 (Mild) | 5–33% | Mild increased echogenicity; vessel borders still visible | None or minimal — simple steatosis | ✅ Yes — fully reversible with lifestyle change |
| Grade 2 (Moderate) | 33–66% | Moderate echogenicity; diaphragm less visible | May have mild inflammation (NASH/MASH) | ✅ Yes — reversible but takes longer (6–12 months) |
| Grade 3 (Severe) | >66% | Marked echogenicity; deep structures cannot be seen | Inflammation likely; early fibrosis possible | ⚠️ Partially — fibrosis may not fully reverse |
| NASH/MASH (Steatohepatitis) | Variable — also inflammation | May not be distinguishable by ultrasound alone; needs biopsy | Active inflammation + cell death | ⚠️ Reversible with treatment; risk of progression |
| Fibrosis (Stage 1–4) | Scarring of liver tissue | Fibroscan (Elastography) measures stiffness | Stage 4 = cirrhosis | ❌ Stage 3–4 largely irreversible; progression can be halted |
Causes and Risk Factors — Why So Many Indians Have Fatty Liver
| Risk Factor | Why It Causes Fatty Liver | Prevalence in India |
|---|---|---|
| Obesity / Central obesity (belly fat) | Visceral fat directly releases free fatty acids into portal vein → liver fat accumulation | Epidemic — especially urban India |
| Type 2 Diabetes / Insulin Resistance | High insulin → liver converts excess glucose to fat (de novo lipogenesis) | 101 million diabetics in India |
| High fructose intake (sugary drinks, maida) | Fructose is metabolised almost exclusively in liver → rapidly converted to fat | Rising with packaged food consumption |
| Excess refined carbohydrates (white rice, maida) | High glycemic index spikes insulin → promotes liver fat storage | Staple Indian diet issue |
| Sedentary lifestyle | No exercise = no mobilisation of liver fat stores; worsens insulin resistance | Common in IT sector, urban workers |
| Dyslipidaemia (high triglycerides, low HDL) | High blood triglycerides directly correlate with liver fat accumulation | Extremely common in India |
| Alcohol (even “moderate” amounts) | Alcohol is metabolised in liver → generates fat precursors and inflammation | Significant — often coexists with NAFLD |
| “Lean NAFLD” — thin Indians with liver fat | Indians have liver fat at lower BMI than Western populations; genetic predisposition; visceral fat despite normal weight | Unique Indian problem — 10–15% of lean Indians have NAFLD |
🇮🇳 The Indian Paradox: Indians develop fatty liver at lower BMI levels than Western standards suggest. An Indian with a BMI of 23 may already have significant liver fat — particularly if they have central obesity (waist >90cm men / >80cm women), high triglycerides, or family history of diabetes. Don’t assume normal weight = no liver disease.
Symptoms of Fatty Liver — Why This is the “Silent Disease”
Simple fatty liver (Grade 1–2 without inflammation) produces no symptoms in 70–80% of patients. This is what makes it dangerous — people live with a progressively worsening condition for 10–20 years before symptoms appear. When symptoms do appear, they typically indicate more advanced disease:
- 😴 Fatigue and weakness — the most common complaint; often attributed to lifestyle stress rather than liver disease
- 🤕 Vague right upper abdomen discomfort — the liver is in the right upper quadrant; mild ache or sense of fullness below the right rib cage
- ⚖️ Unexplained weight gain or inability to lose weight — insulin resistance from fatty liver causes both
- 🩸 Elevated liver enzymes on blood test — SGPT (ALT) and SGOT (AST) above normal is often the first — and only — indication; found incidentally on routine blood work
- 🟡 Jaundice (in advanced disease) — yellowing of eyes and skin indicates serious liver impairment
- 🫃 Enlarged liver (hepatomegaly) — detectable on ultrasound or physical examination by a doctor
- 🦵 Leg swelling and abdominal swelling (ascites) — late-stage sign indicating cirrhosis-level liver failure
Diagnosis — Tests for Fatty Liver in India
| Test | What It Finds | Limitation | Cost (India) |
|---|---|---|---|
| Liver Function Test (LFT) — SGPT/ALT, SGOT/AST | Liver enzyme elevation; SGPT/ALT most sensitive for liver fat damage | Normal SGPT does NOT rule out fatty liver — 70% of NAFLD has normal enzymes | ₹300–600 |
| Ultrasound Abdomen | Grades liver echogenicity; detects fatty liver, liver size, surface | Cannot detect fat below 20–30%; cannot stage fibrosis | ₹800–1,500 |
| FibroScan (Transient Elastography) | Measures liver stiffness (fibrosis stage) and fat content (CAP score) | Less accurate in obesity; not available everywhere | ₹2,000–4,000 |
| Lipid Profile (Triglycerides, HDL) | High triglycerides + low HDL = metabolic syndrome driving NAFLD | Indirect marker only | ₹300–500 |
| Fasting Blood Sugar + HbA1c | Insulin resistance and diabetes are primary NAFLD drivers | Indirect marker | ₹200–400 |
| Liver Biopsy (Gold standard) | Only test that definitively distinguishes NASH from simple steatosis and stages fibrosis | Invasive; expensive; sampling error; reserved for complex cases | ₹15,000–40,000 |
How to Reverse Fatty Liver — Evidence-Based Approach
There is no approved pharmaceutical specifically for NAFLD/MASLD in India (as of 2026). The primary and most effective treatment is lifestyle modification — and the results can be dramatic: Grade 1 fatty liver can fully reverse in 3–6 months with the right interventions.
- ⚖️ Weight loss — the most powerful intervention: Losing just 5% of body weight reduces liver fat. Losing 7–10% significantly reduces liver inflammation (NASH). Losing >10% can reverse fibrosis in early stages. Even 2–3kg weight loss in one month produces measurable liver fat reduction on ultrasound.
- 🚶 Exercise (even without weight loss): 150–300 minutes of moderate aerobic exercise per week directly reduces liver fat independent of weight loss. Resistance training 3×/week additionally improves insulin resistance. Both aerobic + resistance combined is most effective.
- 🍽️ Mediterranean-style diet (adapted for India): Low refined carbohydrates (reduce white rice, maida, sugar), high vegetables, olive/mustard oil over ghee in excess, dal and legumes over red meat, nuts daily. This dietary pattern reduces liver fat faster than any other diet.
- 🚫 Eliminate added sugars and sugary drinks: Fructose is the primary driver of de novo liver fat synthesis. Eliminating cold drinks, fruit juices, and packaged sweets produces rapid liver fat reduction.
- 🍺 Complete alcohol abstinence: Even moderate alcohol dramatically worsens NAFLD prognosis. Zero alcohol is the only safe level for fatty liver patients.
- 💊 Vitamin E (natural tocopherol, 800 IU/day): The only supplement with evidence for NASH treatment; reduces liver inflammation; recommended in AASLD guidelines for non-diabetic NASH patients. Consult doctor before use.
Fatty Liver Diet — What to Eat and Avoid
| Eat More | Why | Eat Less / Avoid | Why |
|---|---|---|---|
| Millets (jowar, bajra, ragi) | Low glycemic index; high fibre; reduces insulin spikes | White rice (large portions) and maida | High GI → insulin → liver fat |
| Dal, rajma, chana, moong | Plant protein + fibre; no liver load | Sugary drinks (cold drinks, packaged juice) | Fructose → direct liver fat synthesis |
| Vegetables (all types) | Fibre reduces fat absorption; antioxidants reduce inflammation | Fried foods, packaged snacks | Trans fats + high calorie → visceral fat |
| Garlic | Allicin reduces liver fat and ALT levels in multiple trials | Alcohol | Direct liver toxin; worsens all fatty liver |
| Fish and omega-3 (2–3×/week) | Omega-3 reduces liver triglycerides and inflammation | Red meat (daily) | Saturated fat + heme iron → liver inflammation |
| Coffee (2–3 cups/day, no sugar) | Strong evidence: coffee drinkers have 40% lower NAFLD progression risk | Full-fat dairy in excess | Saturated fat burden on liver |
| Walnuts | Omega-3 + antioxidants; directly reduce liver fat in NAFLD trials | Jaggery and honey (in excess) | Contain fructose — still metabolised in liver |
Frequently Asked Questions
Can fatty liver be cured completely?
Yes — and this is genuinely good news. Simple fatty liver (Grade 1–2 without fibrosis) is completely reversible with sustained lifestyle changes. Clinical studies consistently show that patients who achieve 7–10% weight loss through diet and exercise have significant regression of liver fat, inflammation (NASH), and even early-stage fibrosis on repeat biopsy or FibroScan. The timeline for reversal depends on severity: Grade 1 fatty liver can normalise on ultrasound within 3–6 months of sustained lifestyle changes; Grade 2 typically takes 6–12 months; NASH (inflammatory stage) may take 12–18 months of consistent effort. The critical caveat: the lifestyle changes must be sustained. Fatty liver returns rapidly if old habits resume. Many patients achieve normal liver enzymes and ultrasound after 6 months, then resume high-sugar, high-GI diets — and develop Grade 2 again within a year. Fatty liver reversal is a permanent lifestyle commitment, not a temporary diet. Advanced fibrosis (Stage 3–4) does not fully reverse but progression can be halted, and some regression is possible with aggressive treatment.
What is the normal SGPT (ALT) level in India?
SGPT (Serum Glutamic Pyruvic Transaminase), also called ALT (Alanine Aminotransferase), is the most liver-specific blood enzyme — primary indicator of liver cell damage. Normal range in India: Up to 40 IU/L for men and 35 IU/L for women (these are the most commonly used Indian lab reference ranges, though some labs use up to 56 IU/L — always compare against your specific lab’s reference range). In fatty liver disease: SGPT elevation of 1.5–3× normal (60–120 IU/L) is typical of active NASH; very high SGPT (>5× normal) should prompt investigation for other liver diseases (viral hepatitis, drug-induced liver injury). Crucially, normal SGPT does NOT rule out fatty liver — studies show 70–80% of NAFLD patients have completely normal SGPT levels while having significant liver fat on ultrasound. Ultrasound is needed to diagnose fatty liver, not just blood tests. When both SGPT and ultrasound are normal but risk factors are present (diabetes, obesity, metabolic syndrome), FibroScan with CAP score provides the most accurate assessment.
Is drinking coffee good for fatty liver?
This is one of the most evidence-backed “good news” findings in hepatology: regular coffee consumption is genuinely protective against fatty liver progression. Multiple large epidemiological studies and a 2017 meta-analysis in the European Journal of Gastroenterology & Hepatology found that drinking 2–3 cups of coffee daily was associated with: 40% lower risk of NAFLD progression to NASH; 40–50% lower risk of liver fibrosis in existing NAFLD; 40% lower risk of hepatocellular carcinoma (liver cancer) in cirrhotic patients. The protective compounds include caffeine (reduces liver fat synthesis) and chlorogenic acids (powerful antioxidants that reduce hepatic oxidative stress and inflammation). The benefit applies to both caffeinated and decaffeinated coffee — suggesting the antioxidant polyphenols, not just caffeine, are the primary drivers. Practical advice: 2–3 cups of black coffee or coffee with minimal milk daily is beneficial for fatty liver patients. No added sugar. Filter coffee (South Indian style), instant coffee, and espresso all appear beneficial based on available studies. Note: this benefit is for patients who already consume coffee and wish to know if it helps — not a recommendation to start drinking coffee solely for liver health.
Can thin people get fatty liver?
Yes — and this is especially relevant in India. “Lean NAFLD” (fatty liver in people with normal BMI) affects an estimated 10–15% of the Indian population with normal body weight — a much higher proportion than in Western countries. The reason is a uniquely Indian metabolic pattern: Indians tend to accumulate visceral fat (fat around organs, especially the liver and abdomen) at lower total body weight. A person who appears thin externally but has a high waist-to-hip ratio, high triglycerides, insulin resistance, or family history of diabetes may have significant liver fat despite a normal BMI. Other risk factors for lean NAFLD in India include: genetic predisposition (PNPLA3 and TM6SF2 gene variants are more common in South Asians), high refined carbohydrate and sugar consumption, sedentary lifestyle, and hypothyroidism (which independently causes fatty liver). The takeaway: liver health screening — ultrasound + SGPT + lipid profile + fasting sugar — should not be limited to obese patients. Any Indian with metabolic risk factors (central obesity, high triglycerides, family history of diabetes, high BP) should be screened regardless of overall body weight.
Which exercise is best for fatty liver?
All moderate aerobic exercise directly reduces liver fat — independent of weight loss. The current evidence-based recommendation for NAFLD patients is: 150–300 minutes of moderate-intensity aerobic exercise per week (30–60 minutes, 5 days/week). Brisk walking is the most practical for most Indians — a meta-analysis of 12 trials found that aerobic exercise alone (without weight loss) reduced liver fat by 20–30% on MRI/FibroScan. For fatty liver patients, the most effective combination is aerobic + resistance training: combine 30 minutes brisk walking (aerobic) with 20 minutes resistance exercises (bodyweight squats, pushups, resistance bands) 3–4 times per week. Resistance training specifically improves insulin sensitivity in muscle, reducing the glucose overflow that becomes liver fat. High-Intensity Interval Training (HIIT) shows the most dramatic liver fat reduction per unit time in clinical trials (20 minutes HIIT = 45 minutes brisk walking for liver fat effect), but may not be appropriate for sedentary or obese beginners — start with walking and progress. The practical first step for a sedentary Indian with fatty liver: 7,000–10,000 steps daily through walking. Research shows this one change alone reduces SGPT significantly within 3 months.
What to Read Next
- How to Reverse Fatty Liver — Complete Diet & Exercise Plan
- What is Diabetes? — Primary Driver of Fatty Liver in India
- High Blood Pressure — Closely Linked with Metabolic Syndrome & Fatty Liver
- PCOS — Insulin Resistance Links PCOS to Fatty Liver in Indian Women
- Control Blood Sugar Naturally — Reversing Insulin Resistance Reverses Fatty Liver
Fatty liver is the liver’s way of documenting your metabolic health. The ultrasound report saying “Grade 1 fatty liver” is not a sentence — it is a warning with a cure attached. Walk for 30 minutes daily, replace maida with millets, stop cold drinks, lose 5% of your weight — and your liver will thank you on the next scan.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on AASLD/EASL NAFLD-NASH guidelines, Indian NAFLD prevalence data, ICMR metabolic disease research, and latest clinical trials. Last updated: March 2026.
Authoritative Sources: AASLD — NAFLD Guidelines | Mayo Clinic — NAFLD | ICMR India | WHO — Liver Disease
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Fatty liver disease requires proper diagnosis through blood tests and ultrasound under medical supervision. Do not start supplements like Vitamin E without consulting your doctor. Always seek professional medical advice for liver health.
