Last Updated: March 2026 | Reading Time: 9 minutes | ~2,000 words
India has the highest burden of iron deficiency anaemia in the world. According to NFHS-5 (2019–21), 57% of children aged 6–59 months, 52.2% of women aged 15–49 years, and 25% of men in India are anaemic — figures nearly unchanged from NFHS-4, despite decades of national supplementation programmes. Anaemia is not just tiredness — it causes impaired brain development in children (irreversible cognitive deficits), reduced work productivity in adults (estimated 2% GDP loss), maternal mortality in pregnancy (anaemia contributes to 20% of maternal deaths in India), and reduced immunity. Yet the commonest form — iron deficiency anaemia (IDA) — is almost entirely preventable and curable through dietary changes, supplementation, and treatment of underlying causes. This guide provides everything an Indian family needs to understand, detect, and address anaemia.
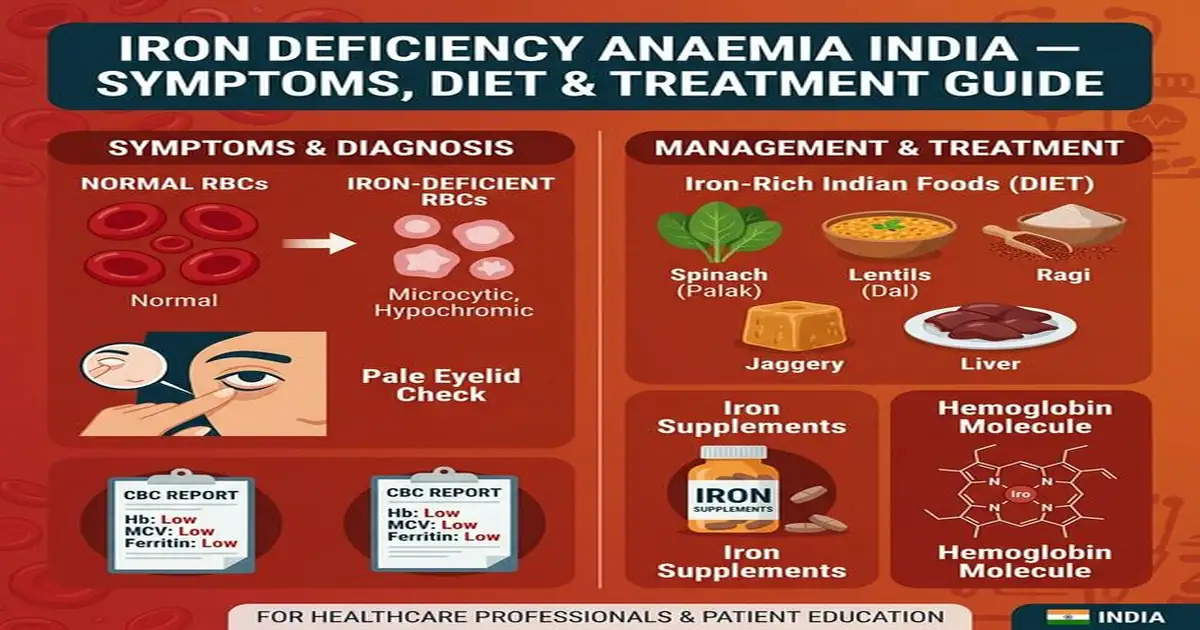
What is Iron Deficiency Anaemia?
Anaemia is defined as haemoglobin (Hb) below the WHO threshold for age and sex: men <13 g/dL; women <12 g/dL; pregnant women <11 g/dL; children 6–59 months <11 g/dL. Iron deficiency is the most common cause of anaemia globally and in India (60–70% of all anaemia), but other causes include Vitamin B12/folate deficiency, thalassaemia trait, chronic disease, and haemolysis. Iron is essential for haemoglobin synthesis (the oxygen-carrying protein in red blood cells), myoglobin (muscle oxygen storage), cytochrome enzymes (cellular energy), immune function (neutrophil killing), and brain neurotransmitter synthesis (dopamine, serotonin). When iron stores are depleted, haemoglobin production fails → microcytic (small), hypochromic (pale) red blood cells → reduced oxygen delivery to every organ.
Haemoglobin Severity Grading
| Severity | Haemoglobin (Adults) | Symptoms | India Management |
|---|---|---|---|
| Mild anaemia | 10–11.9 g/dL (women); 10–12.9 g/dL (men) | Fatigue on exertion; mild pallor; may be asymptomatic at rest | Oral iron + dietary correction at PHC level |
| Moderate anaemia | 7–9.9 g/dL | Fatigue at rest; breathlessness on exertion; palpitations; headache; poor concentration; pallor of conjunctiva, tongue, palms | Oral iron + investigate cause; refer if not responding |
| Severe anaemia | <7 g/dL | Breathlessness at rest; cardiac failure; angina; high output heart failure; bounding pulse; significant pallor; potentially fatal in pregnancy | Hospitalize; IV iron or blood transfusion if cardiac compromise; urgent cause investigation |
| Very severe / crisis | <5 g/dL | Cardiac failure, altered consciousness, potentially fatal | Emergency blood transfusion; ICU support |
Symptoms of Iron Deficiency Anaemia
| System | Symptoms and Signs | India-Specific Notes |
|---|---|---|
| General | Fatigue, weakness, tiredness on minimal exertion — often dismissed as “laziness” or “weakness of body” | Commonest complaint in rural anaemic women; wrongly attributed to overwork or heat |
| Cardiovascular | Palpitations (rapid heartbeat even at rest); breathlessness on exertion; cardiac flow murmur (anaemia murmur) Hb <8 g/dL | Severely anaemic patients misdiagnosed with heart disease in primary care |
| Neurological | Headache; poor concentration; irritability; brain fog; in children: poor academic performance, ADHD-like behaviour, IQ reduction (irreversible if in first 2 years of life) | Most critical consequence — anaemia in first 1000 days is the leading preventable cause of cognitive impairment in India |
| Skin/nails/hair | Pallor of conjunctiva (inner eyelid — most reliable clinical sign), tongue, palm creases; brittle nails; koilonychia (spoon-shaped nails); hair loss; dry skin | Pallor of conjunctiva is the easiest bedside check — pull lower eyelid and check if pink or pale |
| Mouth/tongue | Angular stomatitis (cracks at corners of mouth); glossitis (smooth red tongue — painful); atrophic glossitis | Very common in severely anaemic Indian women; combined with B12 deficiency in vegetarians |
| Pica | Craving for non-food items — ice (pagophagia), clay/soil (geophagia), chalk, raw rice — pathognomonic of iron deficiency | Clay and soil eating — geophagia — widely reported in rural India, particularly in pregnant women; indicates severe iron deficiency |
| Restless legs | Uncomfortable urge to move legs at night — iron is the cofactor for dopamine synthesis; iron deficiency causes RLS | Often unrecognised; treated with iron supplementation, not sleep aids |
Iron-Rich Indian Foods — Complete Guide
| Food | Iron Content (per 100g) | Type | Absorption Tips |
|---|---|---|---|
| Til (sesame seeds) | 14.1 mg — highest among common Indian foods | Non-haem | Eat with lemon juice/amla (Vitamin C doubles non-haem iron absorption) |
| Ragi (finger millet) | 3.9 mg | Non-haem | Ragi mudde + coriander chutney (Vit C); popular South India staple |
| Rajma (kidney beans) | 6.2 mg | Non-haem | Soak overnight (reduces phytates that inhibit iron absorption) |
| Lentils / Masoor dal | 7.6 mg | Non-haem | Add lemon squeeze or tomato; avoid tea/coffee for 1 hour before/after |
| Spinach / Palak | 2.7 mg — but contains oxalates that reduce absorption; net absorption only ~1–2% | Non-haem | Palak paneer (paneer does not inhibit iron absorption); cook with tomatoes |
| Liver (goat/chicken) | 6–10 mg + haem iron | Haem iron (2–3× better absorbed) | Highly bioavailable; best single dietary source; weekly serving recommended |
| Red meat (mutton) | 3.5 mg haem iron | Haem iron | Twice weekly; haem iron absorption not affected by phytates/tea |
| Jaggery (gur) | 11 mg — but quantity consumed small; often overestimated as iron source | Non-haem | Useful in small amounts; total iron contribution limited by serving size |
| Fortified rice/wheat | Fortification adds 28 mg iron/kg grain under POSHAN Abhiyan | Non-haem | Government fortified rice distributed through PDS — major public health intervention |
Key absorption rules: Tea, coffee, milk, and calcium supplements significantly REDUCE non-haem iron absorption — avoid within 1 hour of meals or iron supplements. Vitamin C (lemon, amla, tomato, orange) DOUBLES non-haem iron absorption — consume with every iron-rich meal. Haem iron (meat, liver) is absorbed at 15–35%, nearly unaffected by inhibitors.
Iron Supplementation in India
- 💊 Ferrous sulphate 200mg (65mg elemental iron): Cheapest and most available; best absorbed on empty stomach but causes GI side effects (nausea, constipation, black stool); take with Vitamin C drink; cost ₹2–5/tablet; available at every PHC free under NHM.
- 💊 Ferrous bisglycinate / Ferrous gluconate: Gentler on GI tract; better tolerated; slightly lower elemental iron per tablet but better compliance; cost ₹8–20/tablet; recommended if ferrous sulphate not tolerated.
- 💊 IV Iron (ferric carboxymaltose / iron sucrose): For severe anaemia Hb <7 (especially in pregnancy), malabsorption (post-bariatric, IBD), non-compliance with oral iron, or rapid correction needed; single dose FCM can give 500–1000mg iron; available at government district hospitals; cost ₹800–3,000/dose — expensive but far faster replenishment than oral.
- 📋 Treatment duration: Continue oral iron for 3–6 months AFTER haemoglobin normalises to replenish body stores (ferritin) — stopping when Hb corrects is a common error causing early relapse.
Frequently Asked Questions
Why is India’s anaemia burden so high despite supplementation programmes?
India has had a National Nutritional Anaemia Prophylaxis Programme since 1970, yet anaemia prevalence in NFHS-5 (2019–21) is nearly identical to NFHS-4 (2015–16). This paradox has been studied extensively and the causes are multifactorial: Dietary patterns: India’s predominantly vegetarian diet provides primarily non-haem iron — with very poor bioavailability (2–8% of non-haem iron absorbed vs 15–35% for haem iron). Iron inhibitors — phytates in cereals (the dietary staple), tannins in tea (India’s most consumed beverage), and oxalates in leafy vegetables — dramatically reduce absorption from an already non-haem-heavy diet. India’s tea consumption is particularly problematic — chai with meals is culturally ubiquitous and reduces iron absorption by 60–80%. Iron supplementation programme implementation failures: Worms (helminth infections) — hookworm infestation causes continuous GI blood loss of 0.03–0.05 mL blood per worm per day; 200–400 hookworms = 6–20 mL blood lost daily = perpetual severe anaemia. The Albendazole deworming programme (bi-annual for children under the National Deworming Day) is critical co-intervention. Supply chain failures — IFA (iron-folic acid) tablets not consistently available at PHC level; cold chain breaks; stockouts. Compliance — IFA tablets cause GI side effects leading to poor compliance; black stool alarming patients who stop. Structural determinants: Open defecation (now reduced but ongoing) → hookworm transmission → anaemia. Malaria — haemolytic anaemia from Plasmodium falciparum, particularly in tribal and forested regions. Early marriage and adolescent pregnancy — teenage mothers are simultaneously iron-deficient themselves while supporting foetal iron needs. The solution requires simultaneous action: Dietary diversification (promote liver, pulses + Vitamin C); IFA supplementation with GI-tolerant formulations; deworming; fortification of staples (government fortified rice under POSHAN Abhiyan); delayed cord clamping in newborns (transfers extra 80–100 mg iron); continued open defecation elimination.
What blood tests diagnose iron deficiency anaemia?
A complete diagnostic approach to anaemia uses a staged workup: First-line (CBC — Complete Blood Count): Haemoglobin level; MCV (Mean Corpuscular Volume — reduced in IDA: <80 fL → microcytic anaemia); MCH (Mean Corpuscular Haemoglobin — reduced in IDA: <27 pg → hypochromic anaemia); RBC count; red cell distribution width (RDW — elevated in IDA, reflecting anisocytosis). Peripheral blood smear: microcytic hypochromic red cells, pencil cells, target cells. CBC cost: ₹100–300. Iron studies (confirm IDA diagnosis): Serum ferritin — the most sensitive indicator of iron stores; <30 ng/mL confirms iron deficiency; <12 ng/mL confirms depletion; can be falsely elevated in inflammation (ferritin is an acute phase reactant). Serum iron: reduced in IDA (<60 μg/dL). TIBC (Total Iron Binding Capacity): elevated in IDA (>360 μg/dL). Transferrin saturation: reduced (<20% in IDA). Cost: ferritin ₹300–600; full iron studies ₹500–1,000. Additional workup for cause: Stool for occult blood and ova/cyst (GI bleeding, hookworm); urine routine (haematuria causing iron loss); endoscopy (upper/lower GI) for unexplained IDA in adults — particularly important in men and post-menopausal women where IDA is NOT normal and a GI cause (cancer, peptic ulcer, angiodysplasia) must be excluded. Distinguishing IDA from Thalassaemia trait: Both cause microcytic anaemia. Key difference: thalassaemia trait has normal ferritin (iron stores intact) and very high RBC count despite low Hb; IDA has low ferritin. HPLC or haemoglobin electrophoresis diagnoses thalassaemia trait — critical in Indian context given the high carrier frequency (3–4% beta-thalassaemia trait, up to 40% in some Sindhi, Gujar, and Bengali communities).
Is anaemia dangerous in pregnancy?
Yes — anaemia in pregnancy is one of India’s most critical maternal health problems. Prevalence: 50–55% of Indian pregnant women are anaemic (Hb <11 g/dL); 10–15% have severe anaemia (Hb <7 g/dL). Consequences for mother: Anaemia contributes to 20–40% of maternal deaths in India — through cardiac failure (high-output failure from severe anaemia plus the 30–40% increase in blood volume of pregnancy), postpartum haemorrhage (PPH — the reduced blood reserve means even normal PPH becomes life-threatening), infections (anaemia impairs immune function), pre-eclampsia association. Consequences for baby: Intrauterine growth restriction (IUGR); preterm birth; low birth weight (<2.5 kg — double the risk with severe maternal anaemia); the foetus preferentially extracts iron from the mother, but if maternal stores are depleted, the baby is born with low iron stores and is already at risk for infant iron deficiency and its irreversible cognitive consequences. National programme — Anaemia Mukt Bharat (Anaemia-Free India): WHO iron supplementation for all pregnant women: 60 mg elemental iron + 400 μg folic acid daily from first trimester for 6 months (180 tablets); India extends this to 6 months postpartum. Baseline Hb check at antenatal booking and at 28 weeks. IV iron (ferric carboxymaltose) for Hb <8 g/dL in second/third trimester — oral cannot correct anaemia fast enough. Blood transfusion for Hb <7 g/dL near term. Prevention starts before pregnancy: Iron supplementation in adolescent girls — the Weekly Iron and Folic Acid Supplementation (WIFS) programme provides 1 weekly IFA tablet to all school-going adolescent girls — critical because the iron stores a woman enters pregnancy with determine her pregnancy anaemia risk.
Why are vegetarians more prone to iron deficiency?
Vegetarians in India (60–70% of the population by dietary preference, most of whom are lacto-vegetarian without egg) have significantly higher risk of iron deficiency for fundamental biochemical reasons: Type of iron in diet: Plant foods contain only non-haem iron (ferric Fe³⁺) which must be converted to ferrous Fe²⁺ for absorption — a pH-dependent process highly susceptible to inhibitors. Animal foods (meat, fish, poultry, liver) contain haem iron (ferrous Fe²⁺) directly bound to haemoglobin — absorbed through a separate receptor, completely resistant to dietary inhibitors. Absorption rates comparison: Non-haem iron: 1–10% absorbed (typically 2–5% in Indian diets with high phytate and tea). Haem iron: 15–35% absorbed regardless of inhibitors. This means an Indian vegetarian diet providing 20 mg/day of food iron may deliver only 0.4–1 mg of absorbed iron — less than the minimum requirement (8 mg/day for men, 18 mg/day for premenopausal women). Solutions for Indian vegetarians: Maximise Vitamin C co-ingestion with every iron-rich meal (fresh lemon on dal, raw tomato, amla) — can increase non-haem absorption 2–4×. Avoid tea, coffee, and milk within 1 hour of meals. Include til (sesame), ragi, rajma, masoor dal, and green leafy vegetables daily. Soak and sprout legumes (reduces phytate content). Cook in iron kadai (traditional Indian iron cookware) — demonstrated to increase iron content of cooked food by 2–5× (Lancet study). Include moringa (drumstick leaves — sahjan ke patte) — 28 mg iron/100g dried leaves, extremely high bioavailability, used extensively in traditional medicine and now validated. Eggs (acceptable to many Indian vegetarians) contain significant haem-equivalent iron — 2 eggs/day can significantly supplement non-haem diet. Periodic iron supplementation for vegetarian adolescent girls and pregnant women is essentially non-negotiable.
Does drinking milk, tea, or coffee affect iron absorption?
Yes — this is one of the most practically important dietary interactions for Indian families, given the cultural centrality of chai (tea), coffee, and milk in Indian daily life: Tea (all types including green, black, herbal): Contains tannins — polyphenols that bind ferric iron in the GI tract forming insoluble complexes that pass through unabsorbed. A cup of black tea with a meal reduces non-haem iron absorption by 60–80%. The strength matters: strong masala chai with high tea leaf concentration is more inhibitory than light tea. This is one of the most important nutritional interventions for anaemia prevention in India — shifting chai timing to 1 hour AFTER meals rather than with meals can significantly improve iron absorption at no cost. Coffee: Similar polyphenol content to tea; reduces iron absorption by 40–60%; timing applies similarly. Milk and calcium: Calcium competes with iron for absorption transporters in the GI mucosa; 300mg calcium (1 glass milk) reduces both haem and non-haem iron absorption by 30–40%. This is the reason why telling anaemic patients to “drink more milk for strength” is counterproductive when given simultaneously with iron-rich foods. Practical advice for Indian families: Iron-rich meal + lemon/tomato (Vitamin C) → 45 minutes THEN chai/coffee/milk. Iron tablets: take on empty stomach or with water/Vit C drink; separate from tea, milk, and calcium by at least 2 hours. This single behavioural change — separating chai from meals — may be as impactful as iron supplementation for many mildly anaemic Indian women.
What to Read Next
- Vitamin B12 Deficiency — B12 and Iron Both Cause Anaemia; Often Coexist in Indian Vegetarians
- Vitamin D — Vitamin D Deficiency Impairs Iron Absorption; Both Are Pandemic in India
- PCOS — Heavy Menstrual Bleeding in PCOS Causes Iron Deficiency
- Thyroid — Hypothyroidism Reduces Iron Absorption; Both Coexist in Indian Women
- CKD — Renal Anaemia (EPO Deficiency + Iron Deficiency) in Advanced CKD
57% of Indian children under 5 are anaemic. Their brains are developing right now — and iron is the raw material. Every school meal that includes a lemon squeeze over dal, every child who gets their deworming tablet, every adolescent girl who takes her weekly IFA — that is a mind being protected. The solution to India’s anaemia crisis is not expensive or exotic. It is knowledge, applied daily, in every kitchen.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on NFHS-5 data, WHO Anaemia World Health Report, ICMR dietary guidelines, and Anaemia Mukt Bharat programme guidelines. Last updated: March 2026.
Authoritative Sources: NFHS-5 India | WHO — Anaemia | ICMR India | Anaemia Mukt Bharat — NHM
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Anaemia diagnosis requires a blood count. Iron supplements should be taken under medical supervision — iron overload is harmful. In men and post-menopausal women, iron deficiency without an obvious cause requires GI investigation to exclude cancer.
