Last Updated: March 2026 | Reading Time: 9 minutes | ~2,000 words
Kidney stones (urolithiasis) are the most common urological condition in India — with an estimated 12–15% of Indians experiencing at least one kidney stone in their lifetime. The Indian “stone belt” — comprising Rajasthan, Gujarat, Maharashtra, Punjab, and parts of South India — has the highest incidence globally. Kidney stones cause one of the most severe pains in medicine (routinely described as worse than childbirth), yet most stones can be passed naturally, prevented with simple dietary changes, and effectively treated when intervention is needed. Understanding your stone type is the key to preventing the notoriously high recurrence rate (50% within 5 years without preventive measures).
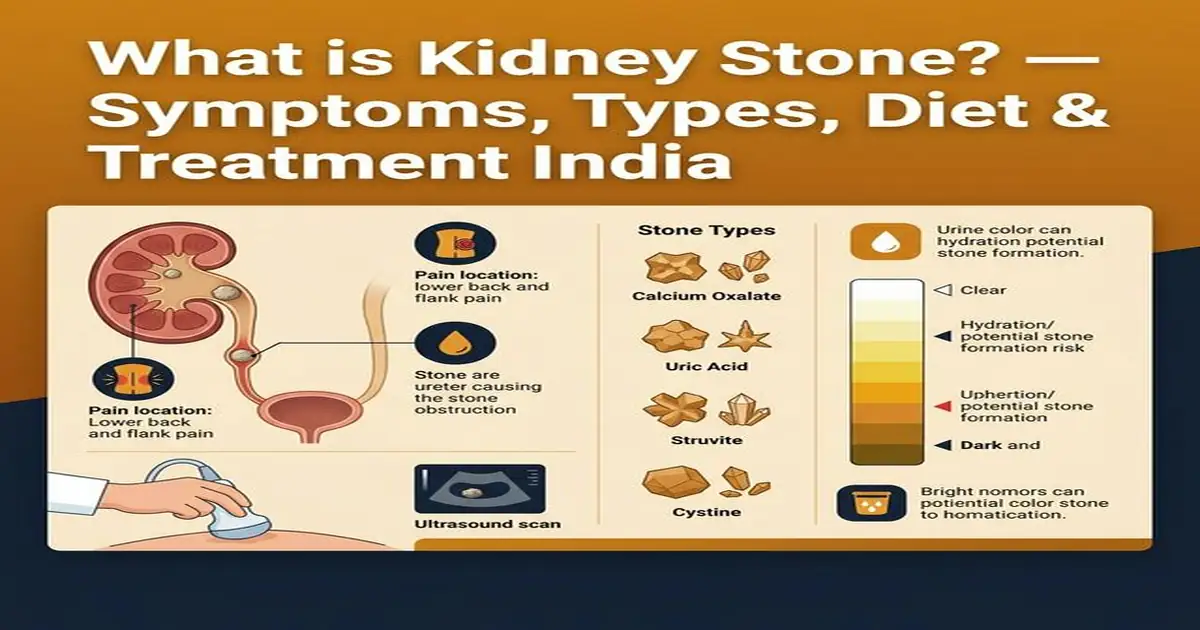
Types of Kidney Stones — Which One Do You Have?
| Stone Type | % of Stones | Appearance on X-ray | Primary Cause | Prevention Focus |
|---|---|---|---|---|
| Calcium Oxalate | 75–80% | Visible (radio-opaque) | High oxalate diet + low fluid intake; low urine citrate; hyperoxaluria | High fluid intake; limit oxalate foods; calcium with meals (binds oxalate); potassium citrate |
| Calcium Phosphate | ~10% | Visible (radio-opaque) | High urine pH; hyperparathyroidism; renal tubular acidosis | Fluid; investigate underlying cause (calcium, PTH levels) |
| Uric Acid | ~10% | Invisible on X-ray (radiolucent) — seen only on CT or ultrasound | High purine diet (meat, seafood); gout; dehydration; acidic urine; metabolic syndrome | Fluid intake; alkalinise urine (potassium citrate or bicarbonate); low-purine diet; allopurinol |
| Struvite (Infection stones) | ~5% | Visible; can be very large (staghorn calculi) | Urease-producing bacteria (Proteus, Klebsiella) in recurrent UTIs; common in women | Complete treatment of UTIs; if stone present → surgical removal required |
| Cystine | <1% | Faintly visible | Genetic disorder — cystinuria; aminoacid transport defect; family history | Very high fluid intake; alkalinise urine; D-penicillamine or tiopronin; genetic counselling |
Symptoms of Kidney Stones
| Symptom | Description | When |
|---|---|---|
| Renal colic (severe flank pain) | Excruciating, wave-like pain from the lower back/flank radiating to groin and inner thigh — follows ureteric peristalsis. Rated 10/10 by most patients. | When stone moves into ureter and causes obstruction |
| Haematuria (blood in urine) | Pink, red, or brown urine; visible or microscopic blood; caused by stone abrading ureter lining | During and after stone passage |
| Nausea and vomiting | Severe nausea/vomiting accompanying colic — vagal response to intense pain | During acute colic attacks |
| Urinary urgency/frequency | Feeling of needing to urinate frequently; burning; when stone is near the bladder (lower ureter) | When stone approaches bladder |
| Fever and chills | 🚨 Emergency sign — indicates infection above stone (obstructive pyelonephritis); requires urgent hospital admission and antibiotics + urgent stone drainage | Any time — urgent if fever + flank pain |
| Silent stones | Many kidney stones cause no symptoms for years — found incidentally on ultrasound done for other reasons; can silently damage kidneys (staghorn calculi) | Asymptomatic throughout |
Diagnosis — Tests for Kidney Stones in India
- 🔊 Ultrasound (USG) KUB — first-line test; detects most stones ≥3mm; available everywhere; no radiation; cannot detect radiolucent uric acid stones reliably; may miss small ureteric stones. Cost: ₹300–800.
- ⚡ NCCT KUB (Non-contrast CT Kidney-Ureter-Bladder) — gold standard; detects EVERY stone type including radiolucent uric acid stones; shows exact location, size, and hounsfield units (density = stone type prediction). Cost: ₹2,000–5,000. Essential before any intervention.
- 🧪 Urine routine + microscopy — haematuria, crystals (oxalate, uric acid crystal shapes help identify type), WBCs (infection), pH (acidic → uric acid; alkaline → struvite)
- 🔬 Stone analysis — if stone passes, save it in a container and bring to lab for infrared spectroscopy analysis — definitively identifies stone composition and guides prevention.
- 🩸 Blood: serum calcium, uric acid, creatinine, eGFR, PTH — identifies secondary causes (hyperparathyroidism, gout, CKD)
- 🧫 24-hour urine collection — the most comprehensive evaluation; measures urine calcium, oxalate, citrate, uric acid, pH, volume — identifies the exact metabolic defect driving stone formation. Recommended for recurrent stone formers.
Treatment — When Stones Pass vs When They Need Intervention
| Stone Size | Spontaneous Passage Rate | Recommended Approach |
|---|---|---|
| ≤ 4 mm | 90–95% | Conservative — high fluid intake; pain management (diclofenac/ketorolac); tamsulosin (alpha blocker) speeds passage; follow-up ultrasound at 4 weeks |
| 5–7 mm | 50–60% | Trial of conservative management with tamsulosin; close monitoring; ESWL or ureteroscopy if not passed in 4 weeks |
| 7–10 mm | 20–30% | Ureteroscopy with laser lithotripsy (Holmium laser — gold standard) preferred; or ESWL for suitable kidney stones |
| > 10 mm (kidney) or > 7mm (ureter) | Very low | ESWL for kidney stones <20mm; URS + laser for ureteric stones; PCNL (percutaneous nephrolithotomy) for large kidney stones >20mm (staghorn) |
| Any size + fever or infection | N/A | 🚨 Emergency — urgent ureteric stent or nephrostomy to drain obstruction + IV antibiotics; stone removal later when infection cleared |
Diet to Prevent Kidney Stones — India-Specific Guide
| Dietary Factor | Calcium Oxalate | Uric Acid | General |
|---|---|---|---|
| 💧 Water intake | 3+ litres/day (urine output ≥2L); most important single prevention measure | 3+ litres/day; prevents uric acid precipitation | Urine should be pale yellow — never dark |
| 🥗 Oxalate-rich foods | Limit: palak (spinach), beet, nuts, chocolate, tea, sweet potato — all high oxalate | No restriction needed | Eat calcium with oxalate foods (calcium binds oxalate in gut) |
| 🥛 Calcium intake | Do NOT restrict calcium — counterintuitively, low dietary calcium increases oxalate absorption and stone risk. Eat normal calcium with meals. | Normal calcium intake | Calcium supplements (not dietary calcium) may increase risk — take with meals if needed |
| 🥩 Purine/protein | Moderate animal protein (excess → acidic urine + hypercalciuria) | Strictly limit: organ meat (kidney, liver), mutton, seafood, red meat, dal in excess | Prefer vegetable protein where possible |
| 🧂 Salt (sodium) | Restrict (<5g/day) — excess sodium → hypercalciuria (calcium leaks into urine) | Restrict — sodium promotes uric acid crystallisation | Avoid papad, pickles, processed foods |
| 🍋 Citrate/lemon | Lemon juice daily (1–2 lemons in water) → urinary citrate → inhibits calcium oxalate crystal formation — highly effective natural prevention | Alkalinises urine — very helpful | Real lemon juice far cheaper than supplement potassium citrate tablets |
| 🫖 Tea consumption | Indian chai (high oxalate from tea leaves) — a significant contributor to high urinary oxalate in Indian stone belt. Limit to 2 cups/day. | Not significant | Replace with water, butter milk, coconut water (isotonic) |
Frequently Asked Questions
Should I avoid calcium and dairy if I have kidney stones?
This is the most dangerous dietary misconception in Indian stone management — and it directly worsens outcomes for the majority of stone patients. For the 75–80% of Indian stones that are calcium oxalate type, restricting dietary calcium is counterproductive and increases stone risk. Here’s why: when you eat calcium-containing foods (milk, curd, paneer), the calcium binds to oxalate in the intestine — forming insoluble calcium oxalate that passes harmlessly in stool and is NEVER absorbed. Without adequate dietary calcium, oxalate is free to be absorbed through the gut wall → reaches the bloodstream → is excreted by kidneys → forms calcium oxalate crystals in urine. Multiple large studies, including a Harvard prospective cohort of 45,000 men, confirmed that higher dietary calcium intake is associated with LOWER kidney stone risk. The crucial nuance: calcium supplements (tablets) taken separately from meals do not have this protective effect and may slightly increase risk — because they don’t encounter food oxalate in the gut. The practical advice for Indian stone patients: eat normal dairy (1–2 cups curd/milk daily), eat paneer normally, and specifically eat calcium WITH meals that contain oxalate (palak, beet, nuts) — the combination protects you. Stop avoiding curd because of kidney stones — it is almost certainly making things worse.
Can kidney stones damage the kidneys permanently?
Yes — and this is an underappreciated risk. While a typical small stone causing acute colic and passing in a few days causes minimal permanent kidney damage, several scenarios do cause lasting harm: Obstructive uropathy — a stone completely blocking urine flow from one kidney for >1–4 weeks causes permanent hydronephrosis (dilatation and scarring of the kidney). The kidney can lose significant function (even become completely non-functional — “silent stone death of the kidney”) without any symptoms if the obstruction is partial or chronic. This is why large asymptomatic kidney stones must be monitored and treated. Infection above obstruction (obstructive pyelonephritis/pyonephrosis) — bacterial infection of urine trapped above a stone causes rapid, irreversible scarring if not drained urgently within hours. This is the most dangerous stone complication. Recurrent stones + recurrent infections — staghorn calculi (struvite stones filling the entire renal collecting system) progressively destroy kidney parenchyma. CKD from stone disease — population studies show nephrolithiasis is an independent risk factor for CKD development; risk is 3× higher in recurrent stone formers. Warning signs of dangerous obstruction: fever + flank pain + nausea (sepsis above obstruction — emergency); inability to urinate from one side; progressive pain unrelieved by painkillers — these require same-day urology evaluation, not waiting at home.
Does drinking coconut water dissolve kidney stones?
Coconut water is widely promoted in India as a kidney stone remedy — and while it has some beneficial properties, it is not a stone dissolver and has important caveats. The benefits: coconut water contains potassium citrate — which alkalinises urine and inhibits calcium oxalate crystal growth, similar to prescribed potassium citrate tablets; natural coconut water contains reasonable magnesium, which also inhibits stone crystallisation; it contributes to fluid intake. The limitations: coconut water contains phosphate which can promote calcium phosphate stone formation; for patients with CKD (even mild), the potassium in coconut water (600–700mg per young coconut) can cause dangerous hyperkalaemia — CKD patients should NOT drink coconut water without nephrologist advice; commercial packaged coconut water often has added sugar and different mineral composition. The verdict: fresh coconut water (1 glass/day) is a reasonable supplement to plain water for stone prevention in healthy individuals with calcium oxalate stones and normal kidney function. It does NOT dissolve existing stones — no beverage does. The primary prevention is plain water — 3+ litres daily. Lemon water (for citrate) is equally effective and much cheaper. Do not replace water with coconut water — take both.
How painful is kidney stone treatment (ESWL / ureteroscopy)?
Modern kidney stone treatment is significantly less traumatic than the perception. ESWL (Extracorporeal Shock Wave Lithotripsy) — a non-invasive procedure where focused shock waves from outside the body break the stone into small fragments that pass in urine. Performed under sedation/analgesia (not general anaesthesia) in 30–45 minutes; patient goes home same day. Mild bruising and haematuria for a few days; may need 2–3 sessions; best for kidney stones under 20mm that are not too dense. Not suitable for lower ureteric stones or very hard stones. Cost in India: ₹15,000–35,000. Ureteroscopy + Laser Lithotripsy (URS-LL) — thin flexible ureteroscope passes through urethra and bladder into ureter; Holmium laser vaporises or fragments the stone; fragments are removed or pass naturally. Performed under spinal or general anaesthesia; day care or overnight stay; a ureteric stent is usually placed for 1–2 weeks post-procedure. Immediate return of urine flow, no residual stones. Cost: ₹25,000–60,000. PCNL (Percutaneous Nephrolithotomy) — for large kidney stones (>20mm, staghorn); a small tube is placed directly into the kidney through the back under imaging guidance; nephroscope removes stone fragments. Requires 2–3 days hospitalisation; highest efficacy for large stones. Cost: ₹50,000–1,20,000. All three procedures are routinely available in tier-2 and tier-3 Indian cities at government hospitals and private urology centres.
Why do Indians get kidney stones more — and how to prevent recurrence?
India’s high kidney stone prevalence results from a convergence of dietary, climate, and genetic factors: Chronic dehydration — hot climate, outdoor work, inadequate water intake, and tea/coffee replacing water all concentrate urine → stone supersaturation. Urine volume below 1 litre/day is strongly associated with stone formation. Diet composition — Indian diet traditionally high in oxalate (palak, beet, nuts), high in salt (pickles, papads, snacks), and increasingly high in animal protein in urban areas. Tea consumption — high tea intake (chai 3–4 cups/day) delivers large amounts of oxalate; Indians drink more tea per capita than almost any other population. Low citrate diet — urinary citrate is the most important natural inhibitor of stone formation; Indian diets are often low in fruit (especially citrus) — the major dietary citrate source. Heat and sweating — outdoor workers in India lose 2–3 litres of fluid through sweat without adequately replacing it, causing chronically concentrated urine. Prevention protocol for recurrent stone formers: 3+ litres water daily (urine pale yellow always); daily lemon juice in water (real lemons); limit palak/beet/chocolate/nuts; normal dairy calcium with meals; restrict salt; limit red meat + organ meat; seek stone analysis after any passed stone; 24-hour urine metabolic evaluation after first recurrence; medication (potassium citrate, allopurinol, thiazide) based on specific metabolic abnormality identified.
What to Read Next
- CKD — Recurrent Stones Are an Independent CKD Risk Factor
- Vitamin D — High-Dose Vitamin D Supplementation Can Cause Hypercalciuria and Stones
- Diabetes — Insulin Resistance Causes Uric Acid Stone Formation
- High Blood Pressure — Hypertension Causes Hypercalciuria; Thiazides Prevent Stones
- What is Anemia? — Ureteroscopy and PCNL Can Cause Temporary Blood Loss
Three litres of water, one lemon squeezed into it, normal curd with meals, less chai — most kidney stones in India are preventable by 4 simple daily habits. The pain of passing a stone—rated as the worst physical pain known to humans — is entirely preventable. Drink more water. Starting today.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on EAU (European Association of Urology) Urolithiasis Guidelines 2024, Indian urolithiasis epidemiology data, and AUA kidney stone guidelines. Last updated: March 2026.
Authoritative Sources: EAU Urolithiasis Guidelines 2024 | AUA — Kidney Stone Guidelines | Mayo Clinic — Kidney Stones | ICMR India
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Kidney stone diagnosis requires ultrasound or CT scanning. Fever + flank pain is an emergency — seek immediate hospital care. Dietary changes should be guided by stone type confirmed by stone analysis or 24-hour urine testing.
