Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
Liver cirrhosis is the end stage of chronic liver disease — and India carries one of the highest cirrhosis burdens in the world. With over 10 million Indians living with cirrhosis and an estimated 200,000 cirrhosis-related deaths annually, it is a major but under-recognised public health crisis. Unlike many other chronic diseases, cirrhosis in India strikes through a uniquely diverse set of causes: alcohol (rising sharply in urban India), hepatitis B (India has 40 million carriers), hepatitis C (6–12 million infected), and non-alcoholic fatty liver disease (NAFLD, now the fastest-growing cause). The crucial fact often missed: cirrhosis is not a sudden disease — it develops silently over 10–30 years. Recognising it early and addressing the cause can halt or even partially reverse fibrosis — but only if caught before the end stage.
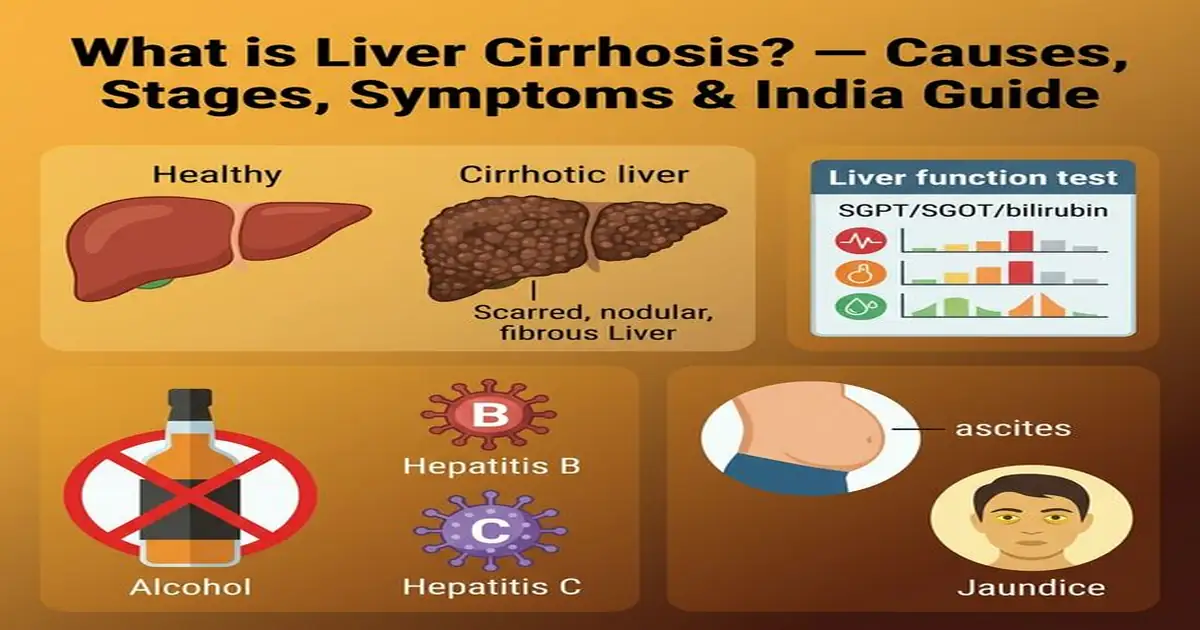
What is Liver Cirrhosis? — The Fibrous End Stage
Cirrhosis is the final, advanced stage of liver fibrosis — where repeated damage and repair cycles replace functional liver tissue with non-functional scar tissue (fibrosis). The normal liver has remarkable regenerative capacity — but when injured repeatedly and chronically (by alcohol, viral hepatitis, fatty liver, etc.), the healing response produces collagen-rich scar tissue instead of normal hepatocytes. Over years, this scar tissue progressively distorts the normal liver architecture into regenerative nodules surrounded by fibrous bands. The result: dramatically reduced functional hepatocyte mass, disrupted blood flow through the liver (causing portal hypertension), and failure of all liver functions simultaneously — clotting, protein synthesis, detoxification, bile production, and hormone metabolism.
Causes of Liver Cirrhosis in India
| Cause | % Cirrhosis in India | Mechanism | Specific India Context |
|---|---|---|---|
| Alcohol-Related Liver Disease (ARLD) | ~30–35% | Acetaldehyde toxicity → steatohepatitis → fibrosis → cirrhosis; threshold: 80g/day men, 40g/day women × 10+ years | Rapidly rising urban India; binge drinking pattern particularly harmful; often undiagnosed until acute decompensation |
| Hepatitis B (HBV) | ~25–30% | Chronic HBV infection → immune-mediated hepatocyte destruction → cirrhosis → HCC | 40 million Indian HBsAg carriers; many undiagnosed; vaccine since 1995 (reducing new infections); antiviral therapy (tenofovir) prevents cirrhosis |
| Non-Alcoholic Fatty Liver Disease (NAFLD/NASH) | ~20% (rapidly rising) | Fat accumulation → NASH (inflammatory) → fibrosis → cirrhosis; metabolic syndrome driven | Fastest growing cause of cirrhosis in India; closely linked to diabetes, obesity, and the consumption of refined carbs |
| Hepatitis C (HCV) | ~10–15% | Chronic HCV → progressive fibrosis → cirrhosis in 20–30% over 20–30 years | 6–12 million Indians infected; most undiagnosed; now 100% curable with 12-week DAA course (sofosbuvir/velpatasvir) |
| Autoimmune Hepatitis (AIH) | ~5% | Immune attack on hepatocytes; responds to immunosuppression if caught early | More common in women; requires liver biopsy for diagnosis |
| Wilson’s Disease | Rare but important | Genetic copper accumulation; causes cirrhosis in young patients (teens–30s) if untreated | India has higher prevalence than Western populations; must rule out in young cirrhosis patients |
| Primary Biliary Cholangitis (PBC) / PSC | ~3–5% | Immune-mediated bile duct destruction → cholestatic cirrhosis | PBC predominantly women; PSC associated with IBD |
Child-Pugh Score — Staging Cirrhosis Severity
| Parameter | 1 Point | 2 Points | 3 Points |
|---|---|---|---|
| Bilirubin (mg/dL) | <2 | 2–3 | >3 |
| Albumin (g/dL) | >3.5 | 2.8–3.5 | <2.8 |
| PT/INR (coagulation) | <1.7 | 1.7–2.3 | >2.3 |
| Ascites | None | Mild/controlled with diuretics | Tense/refractory |
| Hepatic Encephalopathy | None | Grades 1–2 | Grades 3–4 |
Child-Pugh A (5–6 points): Compensated cirrhosis — good liver reserves; surgery tolerable; 1-year survival ~95%. Child-Pugh B (7–9 points): Significant liver compromise; treatment complications common; liver transplant evaluation. Child-Pugh C (10–15 points): Decompensated cirrhosis — poor prognosis; 1-year survival ~35–45%; urgent transplant listing.
Complications of Liver Cirrhosis
| Complication | Mechanism | Treatment |
|---|---|---|
| Ascites (fluid in abdomen) | Portal hypertension + low albumin → fluid leaks into peritoneal cavity; abdominal distension, discomfort | Salt restriction; spironolactone + furosemide; large-volume paracentesis for tense ascites; TIPS procedure |
| Variceal Bleeding | Portal hypertension → dilated veins in oesophagus/stomach (varices) → risk of catastrophic bleed; 50% mortality per episode | Emergency: IV terlipressin + endoscopic band ligation/sclerotherapy; prophylaxis: propranolol; TIPS for refractory |
| Hepatic Encephalopathy (HE) | Liver fails to clear ammonia → brain dysfunction; ranges from subtle personality change to coma | Lactulose 30ml 2–3×/day (reduces ammonia); rifaximin; identify and treat precipitant (infection, bleeding, dehydration) |
| Spontaneous Bacterial Peritonitis (SBP) | Bacterial infection of ascitic fluid without abdominal source; fever, abdominal pain, HE worsening | IV cefotaxime/ceftriaxone; norfloxacin prophylaxis after first episode; albumin infusion reduces mortality |
| Hepatorenal Syndrome (HRS) | Functional kidney failure in advanced cirrhosis; kidney is structurally normal but receives inadequate blood flow | Terlipressin + albumin (HRS Type 1); address precipitants; transplant is only definitive cure |
| Hepatocellular Carcinoma (HCC) | Cirrhosis → HCC risk 2–4% per year; HBV/HCV cirrhosis highest risk; most HCC in India arises in cirrhotic liver | Surveillance: 6-monthly AFP + liver ultrasound; early HCC: curative resection or ablation; advanced: sorafenib |
Frequently Asked Questions
Can liver cirrhosis be reversed?
The traditional view was that cirrhosis is irreversible — but the last decade of hepatology research has fundamentally revised this. The answer is nuanced by stage: Early fibrosis (F1–F2 — pre-cirrhosis): Completely reversible with cause elimination. A patient with NAFLD-related F2 fibrosis who loses 10% body weight and normalises metabolic parameters can have complete fibrosis resolution on repeat biopsy. A hepatitis B patient started on tenofovir at F2 stage often has near-normal liver biopsy after 5 years. Early cirrhosis (F3–F4, compensated, Child-Pugh A): Partially reversible. Viral hepatitis cirrhosis treated with antivirals, or alcoholic cirrhosis with sustained abstinence (2+ years), can show significant histological improvement — a process called “cirrhosis regression.” Not complete reversal but meaningful functional improvement and reduced complication risk. Advanced/decompensated cirrhosis (Child-Pugh B–C with ascites, HE, varices): Irreversible without liver transplantation. The architectural disruption and portal hypertension are too established. The critical message for action: if you have NAFLD, hepatitis B, hepatitis C, or alcohol-related liver disease — deal with it NOW, before cirrhosis develops. A fatty liver can be reversed; a fully decompensated cirrhotic liver cannot.
What is the difference between fatty liver and cirrhosis?
Fatty liver and cirrhosis represent opposite ends of a long progressive spectrum of liver disease — understanding the journey between them is important for motivation to act early. Fatty Liver (NAFLD/Hepatic Steatosis — Grade 1–3): Fat accumulation in liver cells (>5% of hepatocytes); completely reversible with lifestyle changes; no scar tissue; normal or mildly elevated liver enzymes; detected on ultrasound. No symptoms in most. This is where most Indians with the disease currently are. NASH (Non-Alcoholic SteatoHepatitis): Inflammatory fatty liver — fat + inflammation + early cell damage; reversible at this stage with aggressive lifestyle intervention; elevated SGPT/SGOT; beginning of fibrosis risk. Fibrosis (F1–F3): Scar tissue forming but liver structure mostly intact; still partially reversible; requires liver biopsy to stage accurately; FibroScan (elastography) is a good non-invasive alternative. Cirrhosis (F4): Extensive, established scarring; architectural distortion; portal hypertension begins; largely irreversible in advanced stages. The liver “shrinks” and becomes nodular on imaging. The timeline: fatty liver → NASH → fibrosis → cirrhosis typically takes 10–20 years. This is the prevention window. An Indian currently with fatty liver has 10–20 years to prevent cirrhosis — by losing weight, controlling diabetes, changing diet, and stopping any alcohol.
What should a cirrhosis patient eat?
Nutrition in cirrhosis is one of the most critical and underaddressed aspects of management. Cirrhosis causes severe malnutrition in 50–90% of patients — which independently worsens prognosis, increases complications, and increases mortality. Key nutritional principles: High protein intake (1.2–1.5g/kg/day): Contrary to old advice (which recommended low protein to reduce ammonia), current evidence strongly supports HIGH protein in all but overt hepatic encephalopathy. Muscles are the primary alternative ammonia detoxification organ — muscle wasting from low protein intake actually WORSENS ammonia levels and HE. Prefer branched-chain amino acids (BCAA) if intolerant to regular protein — found in dal, milk, eggs. High calorie (35–40 kcal/kg/day): Cirrhosis is hypermetabolic — patients need more calories than perceived body size suggests. Late-evening snack: Proven to improve nitrogen balance in cirrhosis — a BCAA-rich snack before sleep (e.g. 100g chana + glass of milk at 10pm) prevents overnight fasting-induced protein catabolism. Salt restriction (<2g sodium/day): Essential for ascites control — no pickles, papad, packaged foods, processed snacks. Avoid alcohol completely: Even 1 peg accelerates decompensation in all cirrhosis patients, regardless of aetiology. Manage zinc deficiency: Almost universal in cirrhosis; zinc supplementation (zinc sulphate 150mg/day) reduces HE episodes. No raw shellfish: Vibrio vulnificus infection from raw seafood is rapidly fatal in cirrhosis — avoid raw fish, oysters, clams entirely.
Is hepatitis B treatable — can it prevent cirrhosis?
Yes — this is one of the great success stories of modern hepatology and directly relevant to the 40 million Indian HBsAg carriers. While hepatitis B cannot be completely “cured” (HBsAg clearance — “functional cure” — occurs in only 5–10% on treatment), it can be completely suppressed with antiviral therapy to undetectable levels where continued liver damage essentially stops. The results are remarkable: Tenofovir disoproxil fumarate (TDF) or tenofovir alafenamide (TAF) — the current first-line agents — suppress HBV DNA to undetectable within 12–24 weeks in >90% of patients. Long-term tenofovir treatment significantly reduces: fibrosis progression (regression of fibrosis documented on biopsy), cirrhosis development (from 10-year cumulative incidence of 20% to <5%), hepatocellular carcinoma risk (from 2–5%/year to <0.5%/year in cirrhotic patients), and liver-related mortality (> 50% reduction). The treatment is very well tolerated; minimal side effects; can be used in pregnancy (important as vertical transmission is the dominant route in India). Tenofovir (generic branded Tenvir, Tenof) costs INR 20–30 per tablet in India — about ₹600–900/month — and is available on the government’s National List of Essential Medicines free at some centres. Every HBsAg-positive Indian should know their HBV DNA level and liver fibrosis stage, and be on antiviral therapy if indicated. Treating hepatitis B is directly preventing cirrhosis and liver cancer.
What is a liver transplant in India — who needs one and what does it cost?
Liver transplantation is the only definitive treatment for end-stage liver disease (decompensated Child-Pugh C cirrhosis) and for certain liver cancers within specific criteria. India has one of the world’s most advanced liver transplant programmes — performing approximately 2,500–3,000 liver transplants annually at centres including ILBS Delhi, Medanta, Apollo, CMC Vellore, and Government Medical College centres. Two types: Living donor liver transplant (LDLT) — most common in India (75%); a genetically related or emotionally related living donor donates the right lobe of their liver (60% of total liver volume). The donor’s liver regenerates to ~85% of original volume within 6–8 weeks. Both donor and recipient can live complete normal lives long-term. Donor surgery requires 3–5 day hospitalisation; full recovery 6–8 weeks; donors can return to all activities including heavy work after 3 months. Deceased donor (DD) transplant — from a brain-dead donor; waiting time 1–5 years in India (NOTTO waitlist); availability very limited due to low deceased organ donation rates (~0.8 per million in India vs. 40+ in Spain). Cost: ₹20–40 lakhs for surgery; ₹15,000–30,000/month lifelong immunosuppression (tacrolimus + mycophenolate). Ayushman Bharat-PM JAY covers liver transplant up to ₹5 lakhs at most empanelled hospitals — inadequate but helpful. Some state government schemes (Tamil Nadu CM Health Insurance, Karnataka Vajpayee Arogyashri) provide more substantial coverage. Post-transplant outcomes in India at top centres: 1-year survival ~90%, 5-year survival ~75–80% — comparable to world’s best centres.
What to Read Next
- Fatty Liver Disease — The Earliest Reversible Stage Before Cirrhosis
- Diabetes — Metabolic Syndrome Driving NAFLD and Cirrhosis in India
- Cholesterol — High Triglycerides Directly Linked to NAFLD Progression
- Vitamin B12 — Liver Stores B12; Cirrhosis Depletes B12 Severely
- Anemia India — Cirrhosis Causes Multi-factorial Anaemia (Bleeding + Hypersplenism)
The liver never complains — it filters, detoxifies, and repairs silently for decades. By the time it tells you something is wrong through jaundice, ascites, or bleeding varices, 80% of its capacity is gone. Test for hepatitis B. Don’t drink daily. Lose the extra 10 kilos. These three acts protect your liver for life.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on AASLD/EASL Cirrhosis Guidelines 2023, Indian National Association for Study of Liver (INASL) guidelines, and India-specific hepatology epidemiology. Last updated: March 2026.
Authoritative Sources: AASLD — Liver Disease Guidelines | EASL — European Association for Study of Liver | INASL — Indian National Association for Study of Liver | ICMR India
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Liver cirrhosis diagnosis requires clinical evaluation, blood tests, imaging, and sometimes liver biopsy or elastography. Never self-manage cirrhosis complications — variceal bleeding and SBP are medical emergencies. Always consult a hepatologist or gastroenterologist.
