Last Updated: March 2026 | Reading Time: 9 minutes | ~2,000 words
Osteoporosis — literally “porous bone” — is a skeletal disease characterised by reduced bone density and deteriorated bone architecture, leading to fragile bones that fracture with minimal trauma. India has an estimated 50 million people with osteoporosis or osteopenia, yet it remains catastrophically underdiagnosed — surveys suggest less than 5% of Indian osteoporosis patients are ever diagnosed or treated. The disease is called a “silent epidemic” because it causes no pain or symptoms until a fracture occurs. An Indian woman over 50 has a 1-in-3 lifetime risk of an osteoporotic fracture — higher than her risk of breast cancer, heart attack, and stroke combined. A hip fracture in an elderly Indian carries a 20–30% one-year mortality and dramatically reduces quality of life. Yet simple, inexpensive interventions — calcium, Vitamin D, bisphosphonates — can prevent 50–60% of these fractures.
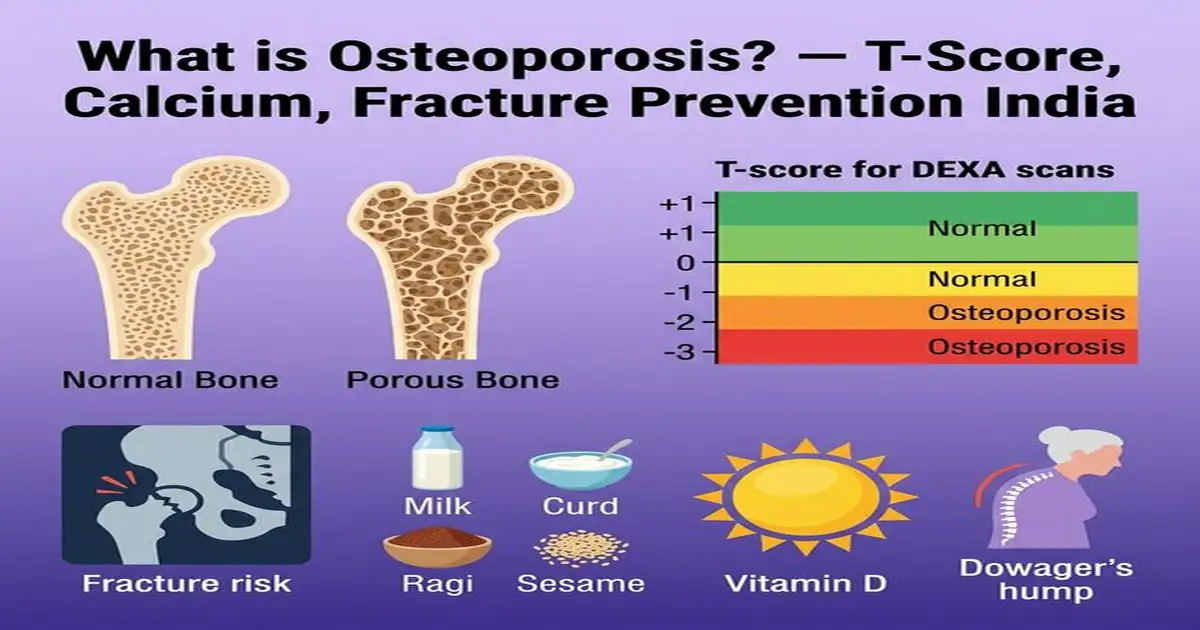
What is Osteoporosis? — Bone Density Explained
Bone is living tissue — continuously being broken down by osteoclasts and rebuilt by osteoblasts in a process called bone remodelling. In childhood and early adulthood, bone formation exceeds resorption → bones grow denser → peak bone mass is reached at age 25–30. After 35, bone resorption begins to gradually exceed formation. In women, oestrogen (which suppresses osteoclast activity) falls sharply at menopause → accelerated bone loss of 3–5% per year for 5–7 years post-menopause. Osteoporosis occurs when this bone loss is severe enough that bone microarchitecture becomes fragile and fracture risk becomes clinically significant. The WHO defines osteoporosis by DEXA scan T-score ≤ −2.5 at the hip or spine.
Understanding Your T-Score — DEXA Scan Results
| T-Score | Classification | Fracture Risk | Action |
|---|---|---|---|
| ≥ −1.0 | Normal bone density | Normal | Maintain with adequate calcium, Vitamin D, weight-bearing exercise; reassess in 5–10 years |
| −1.0 to −2.5 | Osteopenia (low bone mass) | Mildly elevated | Lifestyle optimisation; calcium + Vit D supplementation; FRAX score; consider bisphosphonate if FRAX high |
| ≤ −2.5 | Osteoporosis | Significantly elevated | Bisphosphonate therapy (alendronate/zoledronate); calcium + Vit D; fall prevention; physiotherapy |
| ≤ −2.5 + fragility fracture | Severe Osteoporosis | Very high | Anabolic agents (teriparatide/romosozumab) if bisphosphonate inadequate; specialist management |
Risk Factors for Osteoporosis in India
| Risk Factor | Indian Context | Modifiable? |
|---|---|---|
| Female sex post-menopause | Oestrogen loss → accelerated bone loss for 5–7 years; menopausal age in India averages 46–48 years (earlier than West → longer post-menopausal bone-loss window) | Partially (HRT if appropriate) |
| Vitamin D deficiency | Paradoxically universal in India despite abundant sunshine — covered skin, indoor lifestyle, low dietary Vit D; 70–90% of Indians have low Vit D levels. Vit D is essential for calcium absorption. | ✅ Yes — supplementation |
| Low dietary calcium | Indian vegetarian diet is often calcium-poor — many avoid milk and dairy out of preference or perceived intolerance; ragi and sesame are good non-dairy sources but underconsumed | ✅ Yes — diet + supplements |
| Low peak bone mass | Indian children and adolescents have lower peak bone mass than Western counterparts — due to chronic childhood malnutrition, lower dairy consumption, and lower Vit D levels during growth years | ✅ Yes in childhood and adolescence |
| Corticosteroid use | Long-term prednisolone (asthma, COPD, autoimmune disease, nephrotic syndrome) — most common secondary cause of osteoporosis in India; steroid osteoporosis requires bisphosphonate prophylaxis from day 1 | ✅ Yes — bisphosphonate prophylaxis |
| Sedentary lifestyle | Mechanical loading through weight-bearing exercise is essential for bone maintenance; urban India increasingly sedentary | ✅ Yes — exercise |
| Tobacco and alcohol | Smoking → impairs osteoblast function; alcohol → suppresses bone formation + causes falls | ✅ Yes — cessation |
| Family history | Parental hip fracture doubles individual risk | ❌ No — but increases vigilance |
Calcium — How Much Do Indians Need?
| Group | Recommended Daily Calcium (ICMR) | Best Indian Sources |
|---|---|---|
| Adults (19–50 years) | 600–800 mg/day | Milk (120mg/100ml), curd (120mg/100g), paneer (200mg/100g), ragi (344mg/100g), til/sesame (975mg/100g), rajma/chana (140mg/100g) |
| Post-menopausal women | 1,000–1,200 mg/day | Same sources; supplement (calcium carbonate 500mg with food if dietary insufficiency) |
| Elderly men >70 years | 1,000–1,200 mg/day | Same + supplement if needed |
| Children (9–18 years) | 800–1,000 mg/day | Critical window for peak bone mass; milk + ragi achievable without supplements |
🌱 India’s best non-dairy calcium sources: Ragi (nachni/finger millet) at 344mg/100g is one of the richest plant calcium sources in the world. Til (sesame seeds) at 975mg/100g is extraordinarily calcium-dense — even 2 tablespoons of til ladoo or chutney provides significant calcium. Rajma, chana, and other legumes provide 100–150mg/100g. These are the foods that can bridge the dairy gap for vegetarians avoiding milk.
Treatment — Bisphosphonates and Anabolic Agents
- 💊 Alendronate (70mg weekly oral): First-line bisphosphonate; reduces vertebral fractures by 50%, hip fractures by 40%; must be taken on empty stomach with full glass of water + stay upright 30 mins to prevent oesophageal irritation; generic available in India ₹150–250/month. Branded: Osteofos, Endofos.
- 💉 Zoledronic acid (5mg IV annually): Yearly intravenous infusion; most potent bisphosphonate; reduces hip fractures by 41%; ideal for patients who cannot tolerate oral bisphosphonates; IV administered over 15–30 minutes; one injection per year. Cost: ₹3,000–6,000/injection at private centres; available at government hospitals.
- 💉 Denosumab (60mg SC every 6 months): RANK ligand inhibitor; very effective; advantage in patients with poor kidney function where bisphosphonates are contraindicated; rebound fracture risk if stopped abruptly — must transition to bisphosphonate on stopping. Cost: ₹8,000–12,000 per injection.
- 💉 Teriparatide (20mcg SC daily for 24 months): Anabolic agent — the only treatment that stimulates NEW bone formation rather than just preventing resorption; for severe osteoporosis with multiple fractures; expensive (₹30,000–50,000/month); available under PM-JAY at some centres.
- 🦴 Duration: Bisphosphonates generally given for 5 years (oral) or 3 years (IV zoledronate) then stopped for a “drug holiday” — residual effects persist in bone; reassess after holiday with DEXA.
Frequently Asked Questions
Can osteoporosis be reversed?
Osteoporosis cannot be “cured” in the sense of restoring bone to its original youthful architecture — once trabecular microarchitecture is lost, it cannot be fully regenerated. However, the disease can be significantly improved and fractures effectively prevented: T-score improvement — bisphosphonate therapy increases bone mineral density by 5–10% over 3–5 years on DEXA scan, and teriparatide (anabolic) can increase BMD by 10–15% in just 18–24 months. These BMD gains translate directly into fracture risk reduction even without restoring “normal” microarchitecture. Fracture prevention is the actual goal — alendronate reduces vertebral fractures by 50% and hip fractures by 40% even in patients who started with severe osteoporosis. A person can have persistent low T-score but dramatically reduced fracture risk with treatment. Secondary osteoporosis IS reversible: Steroid-induced osteoporosis improves significantly when steroids are withdrawn; hypogonadism-related (testosterone deficiency in men) improves with hormone replacement; coeliac disease-related improves with gluten-free diet restoring calcium absorption. The preventable tragedy in India: most osteoporosis fractures (hip, vertebral, wrist) occur in patients who never knew they had osteoporosis — because they were never tested. Screen: every woman over 50 should have one DEXA scan. Every person on long-term steroids should have a baseline DEXA and preventive bisphosphonate.
Which calcium supplement is best — carbonate or citrate?
Both calcium carbonate and calcium citrate are effective for osteoporosis prevention and treatment, but they have important practical differences relevant to Indian patients: Calcium carbonate (e.g. Shelcal, Calcimax, Ostocalcium) — most commonly available and cheapest in India (₹5–10/tablet); contains 40% elemental calcium (500mg tablet = 200mg elemental calcium); MUST be taken with food — requires stomach acid for absorption; poor absorption if taken on empty stomach or by patients on PPIs (omeprazole, pantoprazole). A major issue in India: millions of Indians take PPIs daily for gastritis/GERD — for them, calcium carbonate absorption is significantly impaired. Calcium citrate — contains 21% elemental calcium; absorbed effectively without food and without acid — ideal for patients on PPIs, elderly patients (lower stomach acid), and those with achlorhydria; slightly more expensive than carbonate; taken on an empty stomach is fine. Practical Indian guidance: take no more than 500mg elemental calcium per dose (absorption is limited and excess goes to urine, slightly increasing kidney stone risk); two doses throughout the day (with meals for carbonate) are better than one large dose; always combine with Vitamin D3 (1,000 IU/day minimum) — calcium without Vit D is far less effective as intestinal calcium absorption is Vit D-dependent; the Shelcal-HD (500mg calcium + 250IU Vit D) or Calcimax Forte combination tablets are practical and affordable. Dietary calcium is always preferable to supplements — the goal of supplementation is to bridge the gap, not replace food entirely.
Does exercise help build bone?
Yes — weight-bearing and resistance exercise are among the most important non-pharmacological interventions for both preventing and managing osteoporosis, and they work through a clear biological mechanism: mechanical loading of bone stimulates osteoblast activity and bone formation, while also reducing osteoclast-mediated resorption (through mechanical signal transduction via piezoelectric effects in bone). Best exercises for bone health: Weight-bearing aerobic exercise (walking, jogging, dancing, climbing stairs) — creates impact loading stimulating bone remodelling; walking for 30 minutes daily reduces hip fracture risk by 30–40% in postmenopausal women in population studies. Resistance/strength training (weights, resistance bands, bodyweight squats, lunges) — directly loads the skeleton; particularly benefits the hip, spine, and wrist — the three most common osteoporotic fracture sites; even 2–3 sessions/week of strength training significantly improves BMD and reduces falls. Balance training (yoga, tai chi, single-leg standing) — reduces FALLS, which is critically important because a fall is required to cause most osteoporotic fractures. Tai chi in particular reduces fall rates by 47% in elderly studies. What to avoid in established osteoporosis: High-impact activities risking falls (running on uneven surfaces); forward-bending exercises (sit-ups, toe-touches) that compress vertebrae; twisting exercises with heavy weights. The practical prescription for Indian women over 50: 30 minutes daily walking + 2× weekly resistance training (even with bodyweight) + daily yoga for balance. This costs nothing and reduces fracture risk substantially.
Should Indian menopausal women take HRT for bones?
HRT (Hormone Replacement Therapy) — oestrogen alone or oestrogen + progestogen — is highly effective for preserving bone density during and immediately after menopause, when the rate of bone loss is fastest. The WHI trial (which initially caused HRT abandonment in 2002) has been substantially re-analysed: the elevated breast cancer risk was mainly in women who started HRT late (>10 years post-menopause) and in older women. Current guidance for Indian women: HRT initiated within 10 years of menopause (the “timing hypothesis/window of opportunity”) significantly reduces osteoporotic fracture risk AND reduces cardiovascular disease risk AND improves quality of life (reducing hot flushes, sleep disturbance, mood changes, vaginal dryness). Standard menopause treatment guidelines (NAMS, IMS, FOGSI India) now support HRT as an appropriate option for most healthy women under 60 or within 10 years of menopause without contraindications. Contraindications: personal history of breast cancer, oestrogen-dependent gynaecological cancers, unprovoked DVT/PE. Alternative to systemic HRT for bone: raloxifene (SERM) — a selective oestrogen receptor modulator specific to bone — reduces vertebral fracture risk without stimulating breast or uterus, though does not prevent hip fractures as effectively and may cause hot flushes in symptomatic women. For Indian women aged 48–58, menopausal symptoms plus bone loss concern — a gynaecological consultation to discuss HRT with individual risk-benefit assessment is the appropriate step.
What is a hip fracture and why is it so dangerous in India?
A hip fracture — fracture of the proximal femur (femoral neck or intertrochanteric region) — is the most feared consequence of osteoporosis. In India, hip fractures carry uniquely high mortality for several reasons: Late presentation: Many elderly Indian patients with hip fracture wait days before reaching hospital — from lack of family awareness that a fall causing inability to walk requires emergency care, transport challenges in rural areas, and financial concerns about surgery. Every hour of delay worsens outcomes. High complication rate: Prolonged bed rest waiting for surgery or from financial inability to afford surgery causes fatal pneumonia, pulmonary embolism (blood clots), and pressure sores — all preventable with early surgical fixation. Surgical outcomes: Hip fractures require either internal fixation (for non-displaced fractures) or hemiarthroplasty/total hip replacement (for displaced femoral neck fractures) within 24–48 hours. Studies show surgery within 24 hours reduces 30-day mortality by 40%. Conservative management (bed rest without surgery) carries 50%+ one-year mortality. Financial barrier: Hip surgery costs ₹1–3 lakhs at private hospitals; PM-JAY covers this under the health scheme at empanelled hospitals. Prevention is far better: hip protector pads for high-fall-risk elderly; non-slip bathroom mats; adequate lighting; bisphosphonate therapy; Vitamin D and calcium; strength/balance exercise. The one-year mortality after hip fracture in India (25–30%) means that osteoporosis prevention is literally life-saving for elderly Indians.
What to Read Next
- Vitamin D Deficiency — Essential Partner to Calcium for Bone Health
- PCOS — Irregular Periods → Oestrogen Deficiency → Bone Loss Risk
- CKD — Renal Osteodystrophy: Bone Disease from Kidney Failure
- Vitamin B12 — B12 Deficiency Linked to Reduced BMD and Hip Fracture Risk
- Thyroid — Hyperthyroidism Causes Accelerated Bone Resorption and Osteoporosis
The bones that carry you through six decades of life ask for very little — calcium, sunlight, and the effort of a daily walk. Give them that in your 30s and 40s, and they will not betray you in your 70s. The fracture that kills a grandmother begins with the glass of milk she avoided in middle age.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on IOF (International Osteoporosis Foundation) guidelines, ICMR Dietary Reference Values, and Indian osteoporosis epidemiology data. Last updated: March 2026.
Authoritative Sources: International Osteoporosis Foundation (IOF) | ICMR Dietary Reference Values | Mayo Clinic — Osteoporosis | ASBMR — Bone and Mineral Research
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. Osteoporosis diagnosis requires DEXA scanning; fracture risk assessment (FRAX) should be performed by a physician. Bisphosphonate and HRT decisions require medical evaluation. A hip fracture is a medical emergency — seek immediate hospital care.
