Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
India has the highest tuberculosis (TB) burden in the world — accounting for 27% of the global TB burden, with approximately 2.8 million new TB cases per year and over 400,000 deaths annually. Despite being a curable disease with effective treatment available free of cost under the Government of India’s Nikshay programme, TB kills more Indians than any other single infectious disease. The reasons are deeply intertwined with poverty, malnutrition, crowded living conditions, delayed diagnosis, and alarmingly rising drug resistance. This comprehensive guide covers everything — from how TB spreads to the DOTS treatment protocol to the rising threat of MDR-TB (Multi-Drug Resistant TB).
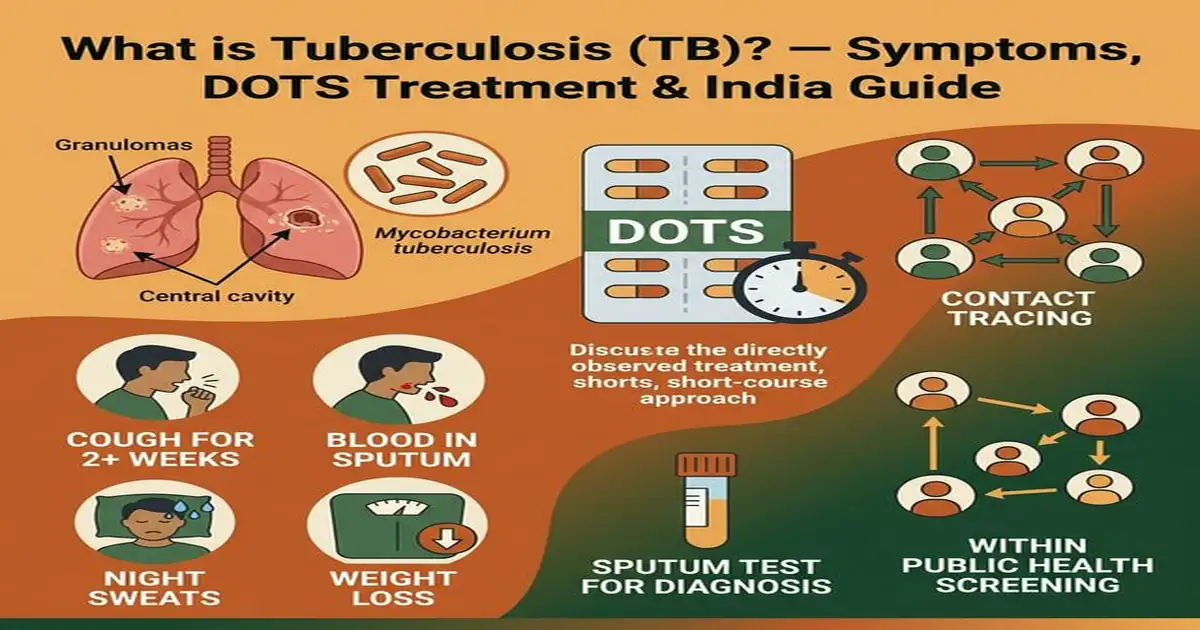
What is Tuberculosis? How TB Spreads
Tuberculosis is a bacterial infection caused by Mycobacterium tuberculosis — a slow-growing, aerobic bacillus that primarily affects the lungs (pulmonary TB) but can spread to virtually any organ in the body (extrapulmonary TB). TB spreads through the air — when a person with active pulmonary TB coughs, sneezes, speaks, or spits, they release microscopic respiratory droplets containing TB bacteria. These droplets can remain suspended in poorly ventilated air for hours. A single cough from an infectious TB patient can release up to 3,000 bacteria-laden droplets. Indoor crowding, poor ventilation, and prolonged close contact are the primary transmission conditions — all of which characterise many Indian living and working environments.
Types of Tuberculosis
| Type | Description | Infectious? | % of TB Cases in India |
|---|---|---|---|
| Pulmonary TB (Lungs) | Classic lung TB — cavities, consolidation; most common form | ✅ Yes — primary source of transmission | ~65% |
| Latent TB Infection (LTBI) | Immune system contains but does not eliminate TB; patient is infected but NOT sick and NOT infectious; can reactivate | ❌ No | 40% of India infected (1 billion people) |
| Lymph Node TB (Lymphadenitis) | Neck or mediastinal lymph nodes; most common extrapulmonary site; presents as painless swollen neck glands | ❌ Usually not | ~15% of extrapulmonary |
| Pleural TB | TB infection of the pleural space (fluid around lungs); chest pain, breathlessness, fever | ❌ Usually not | ~10% of extrapulmonary |
| TB Meningitis | TB in the brain/meninges — most serious; high mortality and disability; severe headache, neck stiffness, altered consciousness | ❌ No | Uncommon but devastating |
| Miliary TB (Disseminated) | TB spreads through bloodstream to all organs simultaneously — seen on chest X-ray as millet-seed pattern; life-threatening | ❌ No | Rare — immunocompromised patients |
| Abdominal TB | TB of intestines, peritoneum, liver, lymph nodes — causes chronic abdominal pain, diarrhoea, weight loss | ❌ No | ~15% of extrapulmonary |
| Bone / Joint TB (Pott’s Disease) | Spinal TB is most common (Pott’s disease); causes back pain, spinal deformity, potential paralysis | ❌ No | ~10% of extrapulmonary |
Symptoms of Tuberculosis — When to Suspect TB
| Symptom | Description | Significance |
|---|---|---|
| 📌 Cough for ≥ 2 weeks | Persistent cough lasting 2+ weeks — the cardinal screening criterion for presumptive TB in India | Must investigate EVERY patient with 2+ week cough for TB |
| Blood in sputum (haemoptysis) | Coughing up blood or blood-streaked sputum | Strongly suggestive of pulmonary TB; requires immediate evaluation |
| Evening rise of temperature / fever | Low-grade fever that peaks in the late afternoon/evening — classic TB pattern | Very characteristic of TB |
| Night sweats | Profuse sweating at night, soaking clothes/sheets — caused by immune response to TB | Classic constitutional TB symptom |
| Unexplained weight loss | Significant unintentional weight loss over weeks to months — patients often describe “slimming down” | Classic TB symptom; TB was called “consumption” for this reason |
| Loss of appetite | Anorexia and inability to eat; compounded by nausea from TB medications | Common; contributes to malnutrition |
| Fatigue and weakness | Persistent severe fatigue out of proportion to activity | Universal in active TB |
| Chest pain / breathlessness | Pleuritic chest pain (worse on breathing) if pleural TB; breathlessness if extensive lung disease | Indicates pleural or advanced pulmonary TB |
TB Diagnosis in India — Tests Available
| Test | What It Detects | Time to Result | Sensitivity | Available Free? |
|---|---|---|---|---|
| Sputum Smear Microscopy (ZN / FM stain) | AFB (acid-fast bacilli) in sputum under microscope | 1–2 hours | Low (40–60%) | ✅ Free at all DOTS centres |
| CBNAAT / GeneXpert (cartridge-based NAT) | TB DNA + rifampicin resistance in 1 test; most important diagnostic advance | 2 hours | High (88–98%) | ✅ Free at DOTS/government labs |
| TrueNat | Similar to GeneXpert; made in India; portable; district-level deployment | 1 hour | High (similar to GeneXpert) | ✅ Free — expanding rapidly |
| LF-LAM (lateral flow lipoarabinomannan) | Urine test for TB; specifically useful in HIV+TB patients with low CD4 | 25 minutes | Moderate (HIV+ only) | ✅ Free in HIV TB co-infection |
| Sputum Culture (MGIT / LJ) | Gold standard; grows actual bacteria; also does full drug sensitivity testing (DST) | 2–8 weeks | Highest | ✅ Free at RNTCP labs |
| Chest X-Ray | TB-typical findings: upper lobe infiltrates, cavities, consolidation, miliary pattern | Minutes | Variable (not specific) | ✅ Government hospitals |
| Tuberculin Skin Test (TST/Mantoux) | Latent TB infection screening — not active TB diagnosis | 48–72 hours (read) | Moderate for LTBI | ✅ Free |
| IGRA (Interferon Gamma Release Assay) | Blood test for LTBI (QuantiFERON-TB Gold) — more specific than Mantoux | 24 hours | High for LTBI | ❌ Private labs — ₹2,000–4,000 |
TB Treatment — DOTS Protocol and Nikshay Programme
- 💊 First-line regimen (Drug-Sensitive TB): 2HRZE / 4HR — Intensive phase: Isoniazid (H) + Rifampicin (R) + Pyrazinamide (Z) + Ethambutol (E) daily for 2 months; then Continuation phase: Isoniazid + Rifampicin daily for 4 months. Total: 6 months. The fixed-dose combination (FDC) tablets now used under Nikshay ensure correct dosing.
- 🏥 DOTS (Directly Observed Treatment, Short-course): India’s national TB control strategy — a healthcare worker observes the patient swallowing every tablet. Despite seeming paternalistic, DOTS has dramatically reduced default rates and treatment failure. All treatment, investigations, and drugs are FREE under PMTBP (Pradhan Mantri TB Mukt Bharat Abhiyaan).
- 💰 Nikshay Poshan Yojana: ₹500/month nutritional support transferred directly to TB patient’s bank account for duration of treatment — recognising that malnutrition is both a cause and consequence of TB in India.
- 🔴 MDR-TB (Multi-Drug Resistant TB): TB resistant to at least Isoniazid + Rifampicin. India has ~100,000 MDR-TB cases annually. Treated with BPaL regimen (Bedaquiline + Pretomanid + Linezolid) for 6–9 months — newer shorter regimen than the older 18–24 month DOTS-Plus. Bedaquiline is now available free in India under RNTCP.
- ⚠️ Treatment completion is non-negotiable: Stopping TB treatment early — even feeling “better” at 2 months — is the primary cause of MDR-TB. The bacteria are not eliminated; the surviving drug-tolerant bacilli multiply and become resistant. Complete all 6 months regardless of symptoms.
Frequently Asked Questions
Is TB completely curable?
Yes — drug-sensitive TB (the most common form) is completely curable with a full 6-month course of first-line antitubercular treatment in the vast majority of patients. The overall treatment success rate for new drug-sensitive TB cases in India’s national programme is approximately 85–88% — meaning 85–88 of every 100 new TB patients who start treatment are cured. The remaining cases represent treatment failure (resistant strains identified too late), death (often from late presentation, HIV, or severe malnutrition at baseline), or default (patient stopped treatment). MDR-TB is harder to treat but still curable — the newer BPaL regimen (Bedaquiline + Pretomanid + Linezolid) achieves 89–93% treatment success in 6 months in clinical trials, a remarkable improvement over the old 18–24 month MDR-TB regimens. XDR-TB (Extensively Drug Resistant TB) remains very challenging but is increasingly treatable with newer drugs (delamanid, pretomanid). The key qualifier: “curable” requires completing the full treatment course. Partial treatment = partial cure = drug resistance. TB treated correctly and completely = genuine cure with no reuse of the same lung scarring (though residual fibrosis may remain on imaging).
Can I get TB from casual contact?
TB transmission requires prolonged, close contact with an infectious (smear-positive pulmonary) TB patient in an enclosed, poorly ventilated space. Casual, brief contact — shaking hands, sharing food briefly, passing someone on the street — does not transmit TB. The primary transmission risk is: living in the same house as an infectious TB patient (household contacts), sharing a small poorly ventilated office or workspace for extended periods, or being in crowded indoor settings (buses, trains, slums) with multiple infectious persons. Even then, exposure does not mean infection — individual immune status, nutritional status, and genetic factors influence whether inhaled TB bacteria establish infection (LTBI) or whether the immune system clears them. Of household contacts of infectious TB patients, approximately 25–50% will become infected (develop LTBI), and of those, only 5–10% will develop active disease over their lifetime (higher if immunocompromised or malnourished). This is why contact tracing of household contacts is a priority — identifying LTBI in contacts and treating it (with 6 months isoniazid preventive therapy) prevents progression to active TB.
What is MDR-TB and how does it happen?
Multi-Drug Resistant Tuberculosis (MDR-TB) is TB caused by Mycobacterium tuberculosis strains resistant to at least Isoniazid AND Rifampicin — the two most effective first-line anti-TB drugs. India has the world’s second-highest MDR-TB burden with approximately 100,000 new MDR-TB cases per year. MDR-TB happens through two mechanisms: Acquired resistance (the more common and preventable cause): a patient with drug-sensitive TB takes irregular treatment — missing doses, stopping early, or taking inadequate drug regimens — allowing drug-tolerant bacterial mutants to survive, multiply, and eventually dominate as resistant strains. This is entirely preventable with proper DOTS. Primary resistance (transmitted): a person newly infected with TB catches a strain that is already resistant — from someone with MDR-TB. No prior treatment required to have MDR-TB. MDR-TB is significantly harder, longer, and more expensive to treat — though the new BPaL regimen has transformed outcomes. The drugs also have more side effects (hearing loss from older injectable aminoglycosides — now largely abandoned; cardiac QT prolongation from bedaquiline requiring ECG monitoring; peripheral neuropathy from linezolid). The most important prevention: complete every single dose of first-line treatment.
Does the BCG vaccine prevent TB?
The BCG (Bacille Calmette-Guérin) vaccine, given at birth in India’s national immunisation schedule, provides significant protection against the most severe forms of childhood TB — particularly TB meningitis (80–90% protection) and miliary (disseminated) TB — but provides variable and often modest protection against pulmonary TB in adults. The vaccine efficacy for pulmonary TB in adults varies enormously by geography — from 0% in South India trials to 80% in UK trials. The leading explanation for this variation is prior sensitisation with environmental mycobacteria (NTMs — non-tuberculous mycobacteria) common in tropical soils — these organisms provide their own partial immunity and also “mask” the BCG immune response. This is why BCG works better in colder climates with fewer NTMs. Despite its limitations for adult pulmonary TB, BCG is crucial for preventing the lethal childhood forms and is maintained in the immunisation schedule for that reason. New TB vaccines being developed (M72/AS01E, VPM1002) show promise for adult protection in clinical trials — Phase 3 results are anticipated. Notably, BCG also has non-specific immune benefits — studies show BCG-vaccinated children have lower mortality from non-TB infections (respiratory, sepsis), suggesting broad immune activation.
What to eat during TB treatment — nutrition guide?
Nutrition is not merely supportive during TB treatment — it is a therapeutic intervention. Malnutrition is both the leading risk factor for active TB (severe protein-energy malnutrition impairs cell-mediated immunity — the primary defence against TB) and a consequence of it (TB causes anorexia, malabsorption, and hypermetabolic state). Studies in India show that malnourished TB patients have 2–3× higher treatment failure and mortality. Key nutritional principles during TB treatment: High protein intake (1.5–2g/kg body weight/day): Protein is essential for immune function and tissue repair. Dal, egg, chicken, fish, paneer in every meal. TB patients who start treatment with severe hypoalbuminaemia (low blood protein) need very aggressive nutritional support. High calorie intake (35–40 kcal/kg/day): The hypermetabolic state of active TB burns significantly more calories — patients need to consciously eat MORE, not less. Pyridoxine (Vitamin B6) supplementation: Isoniazid (H) blocks B6 metabolism → causes peripheral neuropathy. All patients on isoniazid should receive pyridoxine 25–50mg/day to prevent this side effect. Avoid alcohol completely: Alcohol causes hepatotoxicity and the anti-TB drugs (especially isoniazid, rifampicin, pyrazinamide) are also hepatotoxic — combining them risks severe liver failure. Take medications on empty stomach (if well tolerated): Rifampicin absorption is significantly reduced by fat-containing food — ideally taken 30–60 minutes before breakfast. If severe nausea, can be taken with light food. The Nikshay Poshan Yojana ₹500/month helps but is insufficient for meaningful nutritional intervention — families must prioritise food expenditure during the treatment period.
What to Read Next
- What is Asthma? — Often Confused with TB in Early Stages
- Iron Deficiency Anemia — TB + Anemia = Very Common Indian Co-morbidity
- Vitamin B12 Deficiency — Malnutrition Driving Both B12 Deficiency and TB Risk
- Vitamin D Deficiency — Low Vitamin D Significantly Increases TB Risk
- Diabetes — Diabetics Have 3× Higher Risk of Active TB
TB is old, but it is not defeated. It thrives on malnutrition, crowding, and incomplete treatment. Free diagnosis. Free treatment. ₹500/month for nutrition. A cough for 2 weeks is not just acidity or “weakness” — in India, it is TB until proven otherwise. Get tested. Get treated. Complete every dose.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on RNTCP/NTEP India guidelines, WHO TB Report 2023, and published Indian TB epidemiology data. Last updated: March 2026.
Authoritative Sources: NTEP India — National TB Elimination Programme | WHO Global TB Report 2023 | ICMR India | Mayo Clinic — TB
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. TB diagnosis requires sputum testing and medical evaluation. All TB treatment in India is provided free under the national programme. Never start or stop anti-TB medications without medical supervision.
