Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
COPD (Chronic Obstructive Pulmonary Disease) is a progressive, largely irreversible lung disease — and one of the most under-diagnosed conditions in India. Estimates suggest 55 million Indians have COPD, making India home to the largest COPD burden in the world. Unlike asthma, which is largely reversible, COPD involves permanent structural damage to the lungs that worsens progressively over years. The most tragic fact about COPD in India: it is not just a disease of smokers — nearly 50% of Indian COPD patients are non-smokers, primarily affected by decades of biomass fuel smoke (chulha cooking), indoor air pollution, and occupational dust exposure. This is a uniquely Indian pattern that the medical world is only beginning to fully recognise.
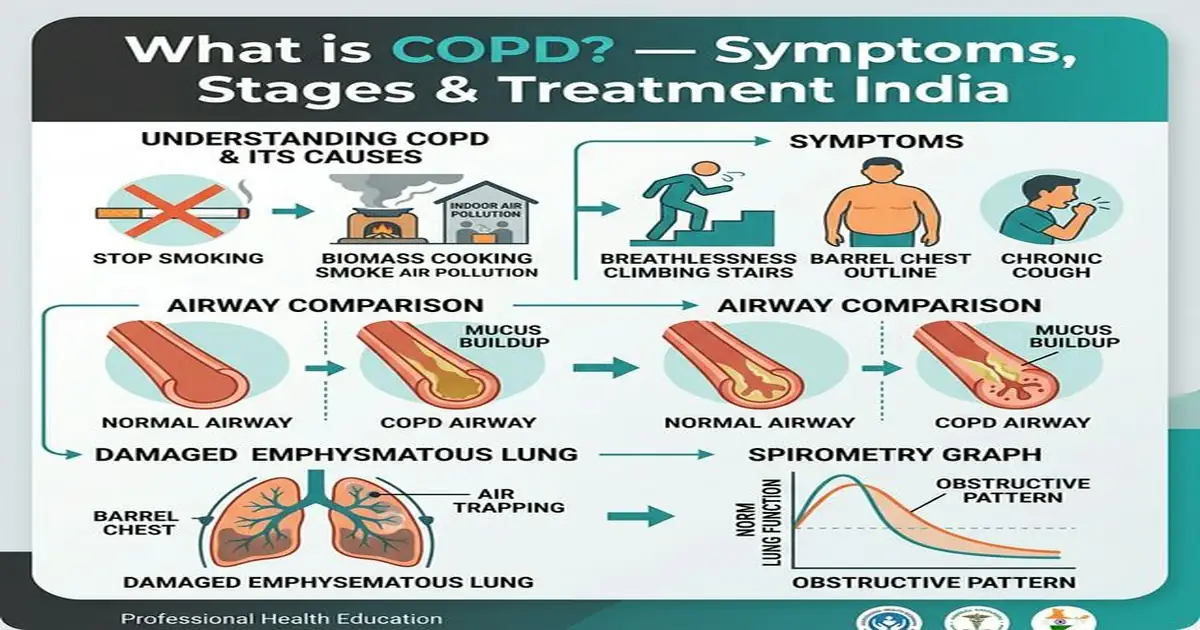
What is COPD? — Two Components Explained
COPD is an umbrella term for two overlapping conditions that frequently coexist:
| Component | What Happens | Dominant Feature |
|---|---|---|
| Chronic Bronchitis | Chronic inflammation and excess mucus production in the large airways (bronchi); persistent productive cough for 3+ months in 2 consecutive years | Cough + sputum (“blue bloater” — cyanotic, oedematous) |
| Emphysema | Destruction of the alveolar walls — the tiny air sacs where gas exchange occurs. Air traps in enlarged, floppy alveoli. Gas exchange severely impaired. | Breathlessness (“pink puffer” — breathless, thin, pursed-lip breathing) |
Causes of COPD in India — Beyond Smoking
| Cause | Indian Context | % Attributed |
|---|---|---|
| Cigarette smoking | Primary cause globally; bidi smoking (unfiltered rolled tobacco) especially harmful — 3–4× more tar per stick than cigarettes | ~50% in India |
| Biomass fuel smoke (chulha) | Cooking on wood, cow dung, crop residue — affects 600 million Indians, predominantly rural women who cook 3–5 hours/day. COPD from biomass is the uniquely Indian pattern. | ~30–40% in India |
| Occupational dust / chemical exposures | Coal miners, silica/stone quarry workers, construction workers, cotton textile workers (byssinosis); grain dust in agricultural settings | ~15–20% in India |
| Indoor air pollution (non-biomass) | Kerosene stoves, poorly ventilated homes with tobacco smoke, mosquito coil smoke (chronic) | Additional contribution |
| Childhood respiratory infections | Recurrent childhood pneumonia permanently impairs lung development — “pre-COPD” state; early-onset adult COPD | Emerging recognition |
| Alpha-1 Antitrypsin Deficiency (AATD) | Rare genetic cause of early-onset emphysema (30–40s) — often family history of liver disease | Rare (<1%) |
COPD Symptoms — How They Progress
| Symptom | Early COPD | Moderate COPD | Severe COPD |
|---|---|---|---|
| Breathlessness (dyspnoea) | Only with strenuous exertion (running, climbing many stairs) | Breathless climbing 1 flight of stairs; walking fast on flat | Breathless at rest; cannot walk 100m; severely limits all activity |
| Chronic cough | Morning cough; may be dismissed as “smoker’s cough” | Persistent daily cough with sputum | Continuous productive cough; frequent exacerbations |
| Sputum production | Minimal; clear | Daily; white/yellow | Copious; purulent during exacerbations |
| Wheeze | Usually absent or mild | May wheeze with activity | Wheeze at rest; often audible without stethoscope |
| Barrel chest | Not yet visible | Beginning to develop | Obvious barrel-shaped chest from air-trapping; hyperinflation on X-ray |
| Cyanosis (blue lips/nails) | ❌ | Mild during exertion | Resting cyanosis in severe cases |
| Ankle oedema | ❌ | ❌ or mild | Significant — indicates right heart failure (cor pulmonale) |
GOLD Staging of COPD — Based on Spirometry
| GOLD Stage | FEV1 (% predicted) | Severity | Typical Symptoms | Treatment |
|---|---|---|---|---|
| GOLD 1 (Mild) | ≥ 80% | Mild | May be asymptomatic; mild cough/sputum; breathless only with strenuous exertion | SABA as needed (salbutamol); smoking cessation; vaccinations |
| GOLD 2 (Moderate) | 50–79% | Moderate | Breathless on walking fast; climbing stairs; regular cough/sputum | LAMA (tiotropium) daily; LABA + ICS if blood eosinophils high or frequent exacerbations |
| GOLD 3 (Severe) | 30–49% | Severe | Breathless walking on flat; frequent exacerbations; significantly limits activities | LAMA + LABA; add ICS if exacerbations; pulmonary rehabilitation |
| GOLD 4 (Very Severe) | < 30% | Very Severe | Breathless at rest; cor pulmonale; may need long-term oxygen therapy (LTOT) | Triple therapy (LAMA + LABA + ICS); LTOT; consider lung transplant evaluation |
COPD Exacerbations — The Most Dangerous Events
COPD exacerbations — acute worsening of breathlessness, cough, and sputum beyond normal day-to-day variation, often triggered by respiratory infections (viral most common) — are the primary driver of COPD mortality and hospitalisation. Each severe exacerbation causes permanent additional lung function loss and shortens survival. Preventing exacerbations is the most important treatment goal in COPD management: annual influenza vaccine; pneumococcal vaccine; LAMA (tiotropium) significantly reduces exacerbations; roflumilast (PDE4 inhibitor) for frequent exacerbating severe COPD. Management of exacerbation: increase salbutamol frequency; systemic steroids (prednisolone 40mg × 5 days — shorter courses now recommended); antibiotics if sputum is purulent/yellow (amoxicillin, doxycycline, or azithromycin); controlled oxygen (target SpO2 88–92%); hospitalisation for severe exacerbations.
Frequently Asked Questions
Can COPD be reversed or cured?
COPD cannot be cured or reversed — the structural lung damage (destroyed alveoli in emphysema, airway remodelling in chronic bronchitis) is permanent. However, several important qualifications change what “irreversible” means in practical terms: Stopping smoking halts progression — even at GOLD 3, cessation of smoking dramatically slows the rate of FEV1 decline from the accelerated rate seen in active smokers (~80ml/year) to something close to normal ageing (~25ml/year). This is the single most impactful intervention. Treatment significantly improves quality of life and reduces mortality — LAMA (tiotropium) therapy in GOLD 2–4 COPD reduces breathlessness, exacerbation frequency, hospitalisations, and mortality. Patients feel dramatically better even though their FEV1 does not significantly improve. Pulmonary rehabilitation — a structured programme of supervised exercise, breathing techniques, and education — improves exercise capacity, breathlessness, and quality of life by 20–30% independent of lung function, by improving muscle efficiency and reducing anxiety/breathlessness perception. Lung volume reduction surgery or bronchoscopic procedures (endobronchial valves) can benefit selected severe emphysema patients by removing over-inflated, non-functional lung tissue — allowing the remaining lung to work more efficiently. Lung transplantation is the only “cure” for end-stage COPD, but is limited by availability and post-transplant survival in India.
What is a spirometry test and do I need one?
Spirometry is the gold-standard test for diagnosing COPD — and it is the only way to confirm the diagnosis and stage severity. The test measures: FEV1 (Forced Expiratory Volume in 1 second) — how much air you can blow out in the first second; FVC (Forced Vital Capacity) — total air blown out in one breath; FEV1/FVC ratio — the critical COPD diagnostic ratio. In COPD: FEV1/FVC ratio < 0.70 (post-bronchodilator) confirms airflow obstruction. The minimal improvement with bronchodilator (<12% or <200ml) distinguishes COPD from asthma. Who needs spirometry in India: anyone over 40 with chronic productive cough, breathlessness, or wheeze — especially current or ex-smokers, bidi smokers, chulha-cooking women with 10+ years’ exposure, miners and quarry workers, and construction workers with dust exposure. Spirometry is widely available at district hospitals, chest clinics, and DOTS centres at low cost (₹300–800). It is scandalously underused in India — most COPD patients are diagnosed only at GOLD 3–4 when substantial irreversible damage has occurred, when earlier diagnosis and cessation could have dramatically slowed progression.
Non-smoker COPD — can women who only cook get COPD?
Yes — and this is one of the most critical public health facts about COPD in India that remains poorly known. Women who cook using biomass fuels (wood, cow dung, crop residue) on traditional chulha stoves 3–5 hours daily for 20–30 years face cumulative smoke exposure equivalent to or exceeding heavy cigarette smoking. Several key facts: PM2.5 levels inside a kitchen during chulha cooking can exceed 1,000 μg/m³ — 40× the WHO safe limit. A woman cooking twice daily for 20 years may inhale more carcinogenic and inflammatory particles than a 2-pack-a-day smoker. Multiple Indian studies confirm COPD prevalence of 10–20% in rural non-smoking women who cook with biomass — equivalent to or higher than male smoker rates. This “biomass COPD” or “Household Air Pollution COPD” is a distinct phenotype: typically older women, non-smoking, with chronic cough and progressive breathlessness; often co-exists with TB (biomass smoke also damages TB immunity); frequently misdiagnosed as recurrent chest infections or “weakness.” Solutions: transition to LPG or electric cooking (Ujjwala Yojana has helped — but compliance remains an issue); improve kitchen ventilation (chimneys, exhaust fans); cook outdoors when possible; N95 mask while cooking if biomass cannot be avoided. India cannot address its COPD burden without addressing household air pollution from biomass cooking.
What is the difference between COPD and asthma?
This is one of the most important clinical distinctions in pulmonary medicine — and one that is frequently confused in India, leading to inappropriate treatment. Key differences: Age of onset — asthma usually starts in childhood or young adulthood; COPD typically presents after age 40. Smoking/biomass history — COPD almost always has significant exposure; asthma can occur with no smoke exposure. Reversibility — asthma shows >12% and >200ml FEV1 improvement after bronchodilator; COPD shows minimal improvement (<12% or <200ml). Progression — asthma is non-progressive with appropriate treatment; COPD is relentlessly progressive even with treatment (though slower with cessation). Eosinophils — blood eosinophils >300 cells/μL suggests asthmatic component (important for ICS response); COPD often has neutrophilic (non-eosinophilic) inflammation. Reversibility on spirometry is the definitive test. Asthma-COPD Overlap (ACO): 15–20% of obstructive lung disease patients have features of both — often ex-smokers with childhood asthma, or long-standing poorly controlled asthmatics with fixed obstruction. ACO has worse outcomes than either condition alone and requires combined treatment (ICS + LABA + LAMA). Management differences: Asthma prioritises ICS (inflammation-suppressor); COPD prioritises LAMA (bronchodilator — tiotropium); LABA+ICS without LAMA in severe COPD is no longer gold standard. Getting this distinction right is clinically important — ICS monotherapy in COPD increases pneumonia risk without proportionate benefit.
What is long-term oxygen therapy (LTOT) in COPD?
Long-term oxygen therapy (LTOT) is the only pharmacological intervention proven to significantly reduce mortality in severe COPD — and it is dramatically underutilised in India. LTOT is indicated when resting SpO2 is persistently ≤88% (PaO2 ≤55 mmHg on arterial blood gas) on two measurements 3 weeks apart in a stable state, OR SpO2 ≤89% in the presence of cor pulmonale (right heart failure) or polycythaemia. Mechanism: chronic hypoxia causes pulmonary hypertension (hypoxic vasoconstriction) → right heart failure. LTOT prevents this cascade — the MRC and NOTT trials showed LTOT >15 hours/day reduces 5-year mortality by 50% compared to no oxygen. The prescription: minimum 15 hours/day (including during sleep and exertion). Oxygen concentrators (electric devices that extract oxygen from room air, 93–95% purity) are the practical home delivery option in India — available for purchase/rent from medical equipment suppliers (₹20,000–60,000 purchase, or ₹500–2,000/month rental). Unfortunately, LTOT is not currently covered under PMJAY (Ayushman Bharat) or most state health schemes — a major policy gap. Key point: oxygen is medicine, not air — it should be prescribed by a doctor based on documented blood oxygen levels, not given casually to any breathless COPD patient. Administering high-flow oxygen (above 88–92% SpO2 target) in severe COPD can suppress the hypoxic drive and worsen CO2 retention (COPD patients rely on hypoxia as breathing stimulus — unlike normal individuals).
What to Read Next
- What is Asthma? — Key Differences from COPD
- Tuberculosis — Biomass Smoke Increases Both TB and COPD Risk
- Vitamin D Deficiency — Low Vitamin D Worsens COPD Outcomes
- Heart Attack — COPD Patients Have High Cardiovascular Co-morbidity
- Cholesterol — Shared Risk Factors: Smoking Causes Both COPD and Heart Disease
Every rural woman cooking three meals a day over a chulha knows breathlessness intimately — she calls it “weakness” or “old age.” It is COPD. It started 20 years ago with the first fire she lit. LPG stoves, better ventilation, and earlier spirometry testing could prevent a catastrophe unfolding silently across India’s villages.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on GOLD (Global Initiative for COPD) 2024 guidelines, Indian Chest Society COPD guidelines, and India-specific biomass COPD research. Last updated: March 2026.
Authoritative Sources: GOLD — Global Initiative for COPD 2024 | Indian Chest Society | WHO — COPD | ICMR India
⚕️ Medical Disclaimer: This article is for general informational and educational purposes only. COPD diagnosis requires spirometry testing. Never self-adjust oxygen therapy or stop prescribed medications without medical supervision. Seek emergency care for sudden severe breathlessness worsening.
