Last Updated: March 2026 | Reading Time: 9 minutes | ~2,000 words
Chronic kidney disease (CKD) is a progressive, largely irreversible condition defined as abnormalities of kidney structure or function present for more than 3 months — characterised by reduced glomerular filtration rate (GFR <60 mL/min/1.73m²) and/or evidence of kidney damage (proteinuria, haematuria, abnormal imaging, or pathological abnormalities). India bears a disproportionate CKD burden: the estimated prevalence of CKD in India is 800 per 100,000 population (~17% of adults in some studies) — with approximately 220,000 new patients requiring renal replacement therapy (dialysis or transplantation) annually, of whom only approximately 10–15% can access it. India’s CKD mortality is approximately 2.2 lakh–2.5 lakh deaths per year from CKD/ESKD (end-stage kidney disease), making it among the top 10 causes of premature death in India. The two dominant causes of CKD in India mirror the diabetes and hypertension epidemic: diabetic nephropathy (30–40% of CKD) and hypertensive nephrosclerosis (20–30%) together account for over 60% of CKD in Indian tertiary centres. Additional India-specific causes include: chronic glomerulonephritis (IgA nephropathy — most common GN India; FSGS; membranous nephropathy), CKD of uncertain aetiology (CKDu — Uddanam in Andhra Pradesh/Odisha — environmental heavy metal exposure, dehydration, aristolochic acid from herbal remedies), chronic interstitial nephritis (analgesic nephropathy from NSAID overuse — extremely common India), and obstructive uropathy (renal calculi — urinary stones very prevalent India). Most Indians with CKD are completely asymptomatic until GFR falls below 15–20 mL/min — making early detection through routine screening of high-risk groups (diabetics, hypertensives) critical.
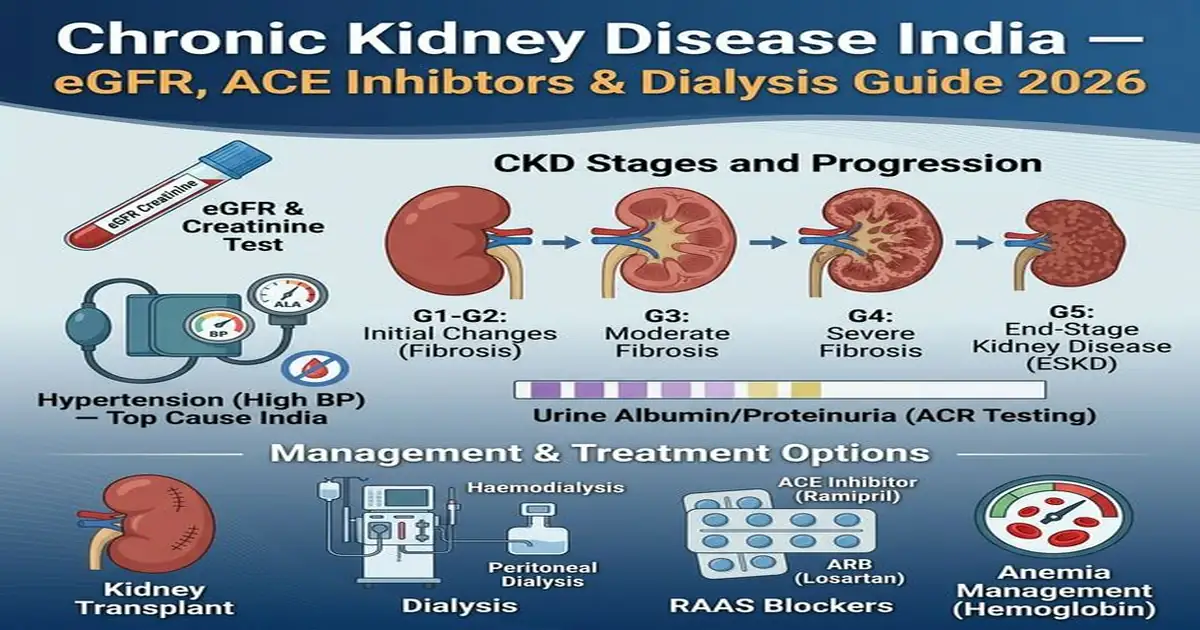
CKD India — Staging, Management and Renal Replacement Therapy
| CKD Stage / Category | eGFR / Criteria | Management Goals | India Context |
|---|---|---|---|
| CKD G1–G2 (Early CKD — High Risk Stage) | G1: eGFR ≥90 mL/min/1.73m² + kidney damage markers (proteinuria ACR ≥30 mg/g, haematuria, abnormal imaging); G2: eGFR 60–89 mL/min/1.73m² + kidney damage markers; eGFR alone without damage markers does NOT diagnose CKD at G1/G2 (many older adults have eGFR 60–89 without CKD — age-related GFR decline is normal); at G1/G2 the kidney still functions near-normally; symptoms absent; opportunity window for slowing/stopping CKD progression entirely | Primary prevention focus: strict BP control (<130/80 mmHg — KDIGO 2022 target for CKD); ACE inhibitor (e.g., ramipril 5–10mg/day) or ARB (losartan 50–100mg/day, telmisartan 40–80mg/day) — FIRST-LINE for CKD with proteinuria especially diabetic nephropathy (reduces intraglomerular pressure — reduces proteinuria — slows fibrosis; RENAAL, IDNT, MICRO-HOPE trials); SGLT2 inhibitors (empagliflozin 10mg, dapagliflozin 10mg, canagliflozin 100mg): now STANDARD OF CARE in CKD with proteinuria (eGFR ≥20) — REDUCE-IT, CREDENCE, DAPA-CKD, EMPA-KIDNEY trials → 30–40% reduction in CKD progression and cardiovascular events; particularly valuable in diabetic CKD where SGLT2i gives dual benefit; strict diabetic control (HbA1c <7.0%); dietary protein moderation (0.8 g/kg/day — avoid high-protein diets); avoid NSAIDs/contrast dye/nephrotoxic drugs; smoking cessation | India: most CKD G1/G2 is never diagnosed — no routine eGFR or urine ACR screening; spot urine albumin:creatinine ratio (ACR): easiest, most sensitive early CKD marker — available at all labs ₹200–400; ACR ≥30 mg/g (microalbuminuria) → CKD diagnosis if persistent 3 months; annual ACR + serum creatinine in ALL diabetics and hypertensives (WHO/KDIGO/India NKF recommendation); SGLT2i: dapagliflozin/empagliflozin generics now available India at ₹15–30/tablet (major affordability improvement from ₹60–90 branded); RAAS blocker generic (ramipril, losartan, telmisartan): ₹1–5/tablet; enormous cost-effectiveness at CKD G1/G2 — avoiding dialysis (₹15,000–20,000/month) by spending ₹200–500/month on drugs |
| CKD G3 (Moderate CKD) | G3a: eGFR 45–59; G3b: eGFR 30–44; kidney damage well established; compensatory hypertrophy of remaining nephrons; patient still largely asymptomatic; nocturia (nighttime urination frequency) may begin; mild anaemia (haemoglobin 10–11 g/dL) from reduced erythropoietin production; CKD-MBD (mineral and bone disorder): phosphate retention → elevated PTH (secondary hyperparathyroidism) begins; vitamin D deficiency worsens | All G1/G2 measures plus: CKD-MBD management: dietary phosphate restriction (avoid high-phosphate foods — processed foods, cola drinks, dairy excess, red meat excess); phosphate binders (calcium carbonate with meals if phosphate elevated); activated vitamin D (calcitriol 0.25–0.5 µg/day) if PTH elevated; serum phosphate, PTH, calcium: monitor every 6 months; CKD Anaemia: EPO (erythropoietin stimulating agent — ESA): darbepoetin or epoetin alfa if Hb <10 g/dL; iron supplementation (IV iron sucrose preferred if on haemodialysis or oral iron poorly absorbed — ferritin target 200–500 µg/L; TSAT >20%); target Hb 10–12 g/dL on ESA (not higher — CHOIR/CREATE trials: higher targets increase CV risk); eGFR monitoring: every 3–6 months; preparation for renal replacement therapy options should begin at G3b: education about HD, PD, transplant options | India G3 management gap: most patients not identified until G4/G5 crisis presentation (acute pulmonary oedema, hyperkalemia, seizures from uraemia); CKD awareness India extremely low — national survey (SEEK study): only 6% of high-risk Indians had been tested for CKD; ESA (darbepoetin, epoetin): expensive (₹1,000–2,000/injection subcutaneously); free at some PMJAY-empanelled hospitals; PMJAY (Pradhan Mantri Jan Arogya Yojana = Ayushman Bharat): covers haemodialysis up to 100 sessions/year for PMJAY beneficiaries; renal function monitoring: serum creatinine + eGFR every 3–6 months in G3 essential to track progression trajectory; eGFR decline rate: >5 mL/min/1.73m²/year = rapid progression → intensify all interventions |
| CKD G4 (Severe CKD — Pre-Dialysis Planning) | eGFR 15–29; uraemic symptoms may begin: fatigue, anorexia, nausea, pruritus (itch from phosphate/uraemia), restless leg syndrome; fluid retention (ankle oedema, dyspnoea); severe anaemia; hypertension worsening; metabolic acidosis (low bicarbonate — accelerates muscle loss and bone disease); risk of hyperkalaemia (high potassium → cardiac arrhythmia — dangerous); risk of severe anaemia; cardiovascular risk dramatically elevated | All prior measures plus: Critical: prepare patient and family for renal replacement therapy (RRT): haemodialysis (HD), peritoneal dialysis (PD), or kidney transplant; AV fistula creation: refer vascular surgeon NOW at G4 (before G5) — AV fistula for HD access takes 3–6 months to mature; if fistula not planned → HD via tunnelled catheter → higher infection/thrombosis risk; Low-protein diet: 0.6–0.8 g/kg/day (with keto-amino acid supplementation); Metabolic acidosis treatment: sodium bicarbonate supplementation (maintain serum HCO3 >22 mmol/L); Hyperkalaemia management: dietary potassium restriction (avoid bananas, tomatoes, potatoes, oranges, vegetables with skin on); potassium binders (patiromer/sodium zirconium cyclosilicate/resonium — calcium resonium powder India: ₹30–50/dose); Hyperphosphataemia: phosphate binders (sevelamer carbonate — newer; or calcium carbonate — cheap); Diuretics: loop diuretics (furosemide IV/oral) for fluid overload management; ACE/ARB: continue unless hyperkalaemia prevents (consider with caution) | India crisis: AV fistula preparation is chronically delayed — most Indian CKD patients arrive at dialysis initiation via emergency AVF or dual-lumen catheter due to late detection/late nephrology referral; PMJAY HD coverage: 100 sessions/year (3 sessions/week = 150/year needed) — inadequate for standard 3×/week HD; gap causes under-dialysis, hospitalisation, mortality; Chandigarh PGI Nephrology, AIIMS Nephrology, CMC Vellore — top India CKD centres; transplant waiting lists: 3–5 year wait for deceased donor kidney India (5,000–6,000 transplants/year for 220,000 needing RRT); living donor transplant: most common India; Balaji Hospital, PSG Hospitals Coimbatore — high-volume transplant centres |
| CKD G5 / ESKD — Renal Replacement Therapy | eGFR <15 mL/min/1.73m²; ESKD (end-stage kidney disease) = kidney function too low to sustain life without RRT; indications to start dialysis (when to initiate): symptomatic uraemia (pericarditis, encephalopathy, nausea/vomiting not controlled); refractory hypervolemia (fluid overload not responding to diuretics); refractory hyperkalaemia (K >6.5 mmol/L or ECG changes); metabolic acidosis refractory (pH <7.2); eGFR <6 mL/min even asymptomatic (KSD guidelines); Haemodialysis (HD): 3×/week (Mon/Wed/Fri or Tue/Thu/Sat); 4–5 hours/session; arteriovenous fistula (AVF — preferred access) or tunnelled vascular catheter; removes waste + fluid + electrolytes via blood filtration through semipermeable membrane; Peritoneal Dialysis (PD): CAPD (continuous ambulatory PD) — 4 exchanges/day (2L each); or APD (automated PD — overnight machine); uses peritoneum as natural semipermeable membrane; done at HOME — no machine/clinic visits; much better autonomy but not suitable for all (peritoneal adhesions, abdominal surgery, hernias) | India HD vs PD: HD vastly more common in India (90%+ on HD); PD under-utilised despite being cheaper and home-based (inadequate training infrastructure, supplier issues with PD bags); Kidney transplant: gold standard — QoL + survival superior to dialysis; living donor (most common India — sibling/spouse/parent); deceased donor (cadaveric — very limited — only 5–6% of India’s transplants); HLA matching, crossmatch, ABO compatibility; immunosuppression post-transplant: tacrolimus + mycophenolate + prednisolone (triple therapy); rejection monitoring: serum creatinine, protocol biopsies; PMJ AY: kidney transplant covered for Ayushman Bharat beneficiaries at empanelled centres; PMGKY: free dialysis (3×/week) at PM Dialysis Programme government hospitals (2016 onwards — 200+ districts) | India dialysis access: only 10–15% of ESKD patients access any RRT; 85–90% die without dialysis access; PM Dialysis Programme: scaled from 5,000 patients (2016) to 200,000+ (2024) — largest single expansion of dialysis access in Indian history; still a fraction of need; ECMO/CRRT: continuous renal replacement therapy in ICU setting for AKI/ESKD with haemodynamic instability — available at major tertiary hospitals; kidney transplant: 5-year graft survival 85–90% India (comparable to global); 5-year patient survival on HD: 50–60% (India) vs 60–70% (USA) — reflecting India’s younger onset ESKD burden from diabetes + late detection |
| CKD-Specific India Challenges — Analgesic Nephropathy, CKDu & NSAID Epidemic | Analgesic nephropathy (chronic interstitial nephritis from NSAIDs): among the most important and preventable causes of CKD in India; NSAIDs (diclofenac, ibuprofen, aceclofenac, nimesulide, ketorolac) available OTC in India (no prescription required for most); used chronically and excessively for pain (osteoarthritis, back pain, headache); mechanism: renal prostaglandin inhibition → afferent arteriolar vasoconstriction → chronic ischaemia → fibrosis; cumulative dose-dependent nephrotoxicity; fenacetin-paracetamol nephropathy: historical; CKD of Uncertain Aetiology (CKDu — Uddanam CKD): Uddanam region, Srikakulam district, AP — one of the world’s highest CKD prevalence rates in young male agricultural workers with no diabetes/hypertension; hypotheses: fluoride/heavy metal contamination groundwater, dehydration, low antioxidant diet, herbal aristolochic acid; IGKV1-39 locus identified in genome-wide study (genetic susceptibility); similar CKDu in Sri Lanka (Rajarata region), Central America (Mesoamerican nephropathy) | NSAID avoidance: NO NSAID use in CKD G3+ (absolute contraindication — further accelerates fibrosis); prefer paracetamol (acetaminophen — renally safe in recommended doses); tramadol (with dose adjustment in CKD); gabapentin (with dose reduction in CKD) for neuropathic pain; OTC NSAID sale in India: major public health failure — FDA India has NOT restricted OTC NSAID sale; advocacy needed; CKDu: no proven treatment beyond supportive care; mass screening in Uddanam (ASHA-based urine dipstick programmes) → early identification; water source improvement projects; farmer hydration campaigns; agricultural worker health monitoring | India NSAID crisis: diclofenac gel + tablet freely available ₹10–30 at any medical shop; millions use chronically without knowing renal toxicity; pharmacist education required; NSAID nephropathy India: estimated 5–10% of CKD — preventable entirely with paracetamol substitution; CKDu Uddanam: “graveyard of young men” — entire villages of young farmers with ESKD without traditional risk factors; state government AP: Uddanam CKD relief fund, renal care camps, government dialysis centres in Srikakulam |
Frequently Asked Questions
How do creatinine and eGFR work — and what levels should worry a diabetic or hypertensive Indian?
Creatinine and eGFR are the two most commonly used — and most commonly misinterpreted — kidney function tests in India. Understanding their relationship is essential for every person with diabetes or hypertension: Serum creatinine — what it measures and why it’s imperfect: Creatinine is a metabolic by-product of creatine phosphate breakdown in muscle; it is filtered by the glomerulus and not reabsorbed — thus serves as an endogenous marker of glomerular filtration; serum creatinine rises as kidney function falls (inverse relationship); HOWEVER: creatinine has a massive “blind spot” — because of the kidney’s enormous functional reserve, creatinine remains within the “normal” laboratory range until approximately 50% of kidney function is lost; a person with eGFR of 45 mL/min (G3a — significant CKD) may have creatinine of only 1.5–1.8 mg/dL — within many Indian labs’ printed “normal range” of up to 1.5–2.0 mg/dL; this is the creatinine illusion: normal creatinine does NOT mean normal kidneys; additionally, creatinine varies with muscle mass: a thin elderly Indian woman with creatinine 1.1 mg/dL may have eGFR of only 38 mL/min (G3b — severe CKD); a muscular young man with creatinine 1.5 mg/dL may have eGFR of 70 mL/min (normal). eGFR — the correct kidney function measure: eGFR (estimated Glomerular Filtration Rate) is calculated from serum creatinine + age + sex using validated equations (CKD-EPI 2021 — no longer includes race coefficient; or MDRD); eGFR accounts for muscle mass and age — far more accurate than creatinine alone; eGFR interpretation: ≥90 = G1 (normal or high — need kidney damage marker to diagnose CKD); 60–89 = G2 (mildly reduced); 45–59 = G3a (mildly to moderately reduced); 30–44 = G3b (moderately to severely reduced); 15–29 = G4 (severely reduced); <15 = G5 (kidney failure); most lab reports in India still do NOT auto-calculate eGFR — this must change (NKF India recommendation: all labs should automatically calculate and report eGFR when creatinine is ordered); how to calculate yourself: use any online CKD-EPI calculator (enter age, sex, serum creatinine); or download the Kidney Failure Risk Equation (KFRE) app. Urine albumin:creatinine ratio (ACR) — the earlier, more sensitive test: Detects kidney damage before eGFR falls; ACR <30 = normal (A1); ACR 30–300 = microalbuminuria (A2 — moderate damage); ACR >300 = macroalbuminuria (A3 — severe damage); ACR test: spot urine (random sample — morning preferred); simple, cheap (₹200–400 India); must be repeated twice over 3 months to confirm CKD (ACR elevated once may be transient — UTI, fever, exercise); at what point should a diabetic/hypertensive worry: ANY ACR >30 + confirmed at 3 months = CKD → start ACE inhibitor/ARB immediately regardless of blood pressure; eGFR <60 persisting 3 months = CKD; eGFR declining by >5 mL/min/year = rapid progression → urgent nephrology referral.
What diet should a CKD patient in India follow — and what drugs must be avoided?
Dietary management and drug avoidance are the two most impactful non-pharmacological interventions in CKD management — and both are poorly understood by most CKD patients in India: CKD diet in India — the key principles by nutrient: Protein: CKD G3–G5 (not on dialysis): low-protein diet 0.6–0.8 g/kg/day (reduces uraemic waste production, slows fibrosis); India problem: high-protein diets (protein supplements, whey protein, excess dal/pulses for vegetarians) are extremely popular and cause rapid CKD worsening in known CKD patients; keto-acid analogues (Ketosteril — ₹8–10/tablet): supplement to low-protein diet to prevent malnutrition while restricting protein; on dialysis (HD/PD): INCREASE protein to 1.2–1.4 g/kg/day (dialysis removes protein — need more); Potassium: CKD G4–G5 and on dialysis: restrict high-potassium foods; HIGH potassium (restrict): banana (richest K fruit), tomato, potato, sweet potato, spinach, orange, coconut water, avocado, dried fruits; SAFE potassium (allow): apple, pear, grapes, berries, cabbage, carrot, cucumber, cauliflower (boiling/discarding water reduces potassium in vegetables by 30–50%); India danger: coconut water (very popular India — 600–700 mg K per serving) → fatal hyperkalaemia documented in ESKD patients who drank coconut water; Phosphate: CKD G3+: restrict high-phosphate foods; HIGH phosphate (restrict): dairy (milk, curd, cheese, paneer), cola drinks (phosphoric acid), processed meats, legumes excess; phosphate binders: calcium carbonate (with meals: ₹10–20/tablet), sevelamer (more expensive: ₹30–60/tablet), calcium acetate; Sodium: restrict to <2g/day (most India food salt-heavy — reduce cooking salt, papad, pickle, processed snacks); Salt restriction reduces BP, fluid retention, proteinuria — massive CKD benefit; Indian low-sodium diet challenges: preserved foods (achar/pickle contain very high sodium), street food, restaurant food; Fluids: CKD G4/G5 and HD: restrict fluids to urine output + 500mL/day (avoid overhydration — volume overload causes pulmonary oedema, hypertension); CAPD (PD) patients: less fluid restriction than HD. Drugs to AVOID absolutely in CKD: NSAIDs (diclofenac, ibuprofen, aceclofenac, nimesulide, naproxen, ketorolac, piroxicam): ABSOLUTELY CONTRAINDICATED in CKD G3+ — cause acute-on-chronic kidney injury, hyperkalemia, fluid retention; even a single dose of IV ketorolac post-surgery can precipitate AKI on CKD; substitute: paracetamol (safe in CKD — only hepatic metabolism); Contrast dye (IV iodinated contrast — CT scan, coronary angiogram, IVP): NEPHROTOXIC in CKD — contrast-induced nephropathy (CIN); if eGFR <45: pre-hydrate with IV saline + use low-osmolar contrast + minimise volume; if eGFR <30: avoid contrast CT if possible (US/MRI alternative); Aminoglycoside antibiotics (gentamicin, amikacin): highly nephrotoxic — avoid in CKD or reduce dose with extended interval monitoring; Metformin: hold if eGFR <30 (risk of lactic acidosis); safe up to eGFR 30–45 with monitoring; Lithium: nephrotoxic with chronic use; herbal medicines: many Indian herbal/Ayurvedic formulations contain aristolochic acid (Aristolochia spp. — found in some household remedies — causes irreversible aristolochic acid nephropathy — AAN); completely avoid any unlabelled herbal preparation; traditional Indian pain relief remedies (many OTC Ayurvedic formulations contain plant-derived NSAIDs); Gadolinium MRI contrast: NSF (nephrogenic systemic fibrosis) risk in ESKD — use with extreme caution if eGFR <30.
What to Read Next
- Diabetes — Diabetic Nephropathy: ACR Yearly; ACE Inhibitor + SGLT2i Combination Cuts CKD Progression 60%; HbA1c <7% Slows Microalbuminuria
- Hypertension — BP <130/80 in CKD (KDIGO 2022); ACE/ARB Preferred; Thiazide vs Loop Diuretics by eGFR; Amlodipine Safe in All CKD Stages
- Kidney Stones — Recurrent Calculi Cause Obstructive CKD; Hydration 2.5L/Day; Stone Composition Guides Prevention; Staghorn = Immediate Urology
- Anaemia — CKD Anaemia of Chronic Disease: EPO Deficiency + Iron Deficiency; IV Iron Sucrose + ESA; Target Hb 10-12 g/dL; Avoid Hb >13 on ESA
- Hepatitis C — HCV + CKD: Glecaprevir/Pibrentasvir Safe in eGFR <30; No SOF; Free G/P Treatment at NVHCP for HCV-CKD Coinfection
A 52-year-old man with 15-year history of Type 2 diabetes in Hyderabad. His annual blood tests always showed creatinine 1.4 mg/dL — “normal” according to the lab report. His HbA1c averaged 9.2%. He took diclofenac 50mg twice daily for knee pain for 3 years. His nephrologist finally calculates his eGFR: 28 mL/min — G4 CKD. His urine ACR: 850 mg/g. He has had advanced CKD for years — lurking behind that “normal” creatinine. Diclofenac is stopped immediately. He starts ramipril + empagliflozin. His HbA1c is brought to 7.1%. His potassium is 5.9 — coconut water is stopped. An AV fistula is created. In 12 months: eGFR has stabilised at 25 — not improved, but not declining. He has bought himself time. Two years later, his brother donates a kidney. His eGFR is 58 with the transplant. He need not have reached G4 — if his creatinine had been converted to eGFR twelve years ago.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on KDIGO CKD Clinical Practice Guidelines 2024, India NKF CKD Management Protocol 2023, SEEK India CKD Prevalence Study, and PM Dialysis Programme Annual Report 2023. Last updated: March 2026.
🔬 Diabetic or Hypertensive? Get These Two Tests Annually: (1) Urine ACR (albumin:creatinine ratio) — at any lab ₹200–400. (2) Serum creatinine + eGFR calculation — ask your doctor to calculate eGFR (or enter creatinine + age + sex into any online CKD-EPI calculator). If ACR >30 or eGFR <60: start ACE inhibitor + SGLT2 inhibitor immediately with nephrologist guidance. Stop all NSAIDs (diclofenac, ibuprofen).
🚫 NSAIDs Are Banned in CKD — Stop Diclofenac/Ibuprofen Now If CKD G3+: Diclofenac, ibuprofen, aceclofenac, nimesulide, and all other NSAIDs are absolutely contraindicated in CKD stages G3–G5. Even a short course accelerates kidney failure. Switch to paracetamol (acetaminophen) for pain relief in CKD. This single change can buy years of kidney function.
⚕️ Medical Disclaimer: This article provides general educational information about CKD. All staging, treatment decisions (ACE inhibitor, SGLT2i, dialysis modality, transplant evaluation), dietary and drug adjustments in CKD require qualified nephrologist assessment. CKD management is highly individualised — do not self-adjust medications without medical supervision.
