Last Updated: March 2026 | Reading Time: 8 minutes | ~1,900 words
Coeliac disease (celiac disease — CD) is a chronic autoimmune enteropathy triggered by dietary gluten (a protein complex found in wheat, barley, and rye) in genetically predisposed individuals (HLA-DQ2 or HLA-DQ8 haplotypes). In coeliac disease, ingested gluten triggers a T-cell-mediated immune response in the small intestinal mucosa, causing progressive villous atrophy — flattening of the finger-like projections (villi) that dramatically expand intestinal absorptive surface area — resulting in malabsorption of essential nutrients (iron, calcium, fat-soluble vitamins, folate, B12). India has a particularly significant coeliac burden: estimated prevalence is approximately 1 in 100–200 individuals (0.5–1%) — with an estimated 6–8 million Indians with coeliac disease, of whom the vast majority remain undiagnosed. CD is especially prevalent in the North Indian wheat-belt (Punjab, Haryana, Rajasthan, UP, Delhi, Himachal Pradesh) where wheat forms the staple diet from infancy, but it is present across all Indian regions. The condition manifests across a wide spectrum — from classic GI presentation (diarrhoea, malabsorption, failure-to-thrive in children) to completely silent/atypical presentation (detected only on screening of high-risk groups — anaemia, short stature, osteoporosis, infertility, liver disease). The only treatment is a strict, lifelong, completely gluten-free diet (GFD) — which is simultaneously the most effective and most socially challenging treatment in gastroenterology, given India’s wheat-centric food culture (roti, bread, samosa, biscuits, atta, pasta, seviyan — all gluten-containing).
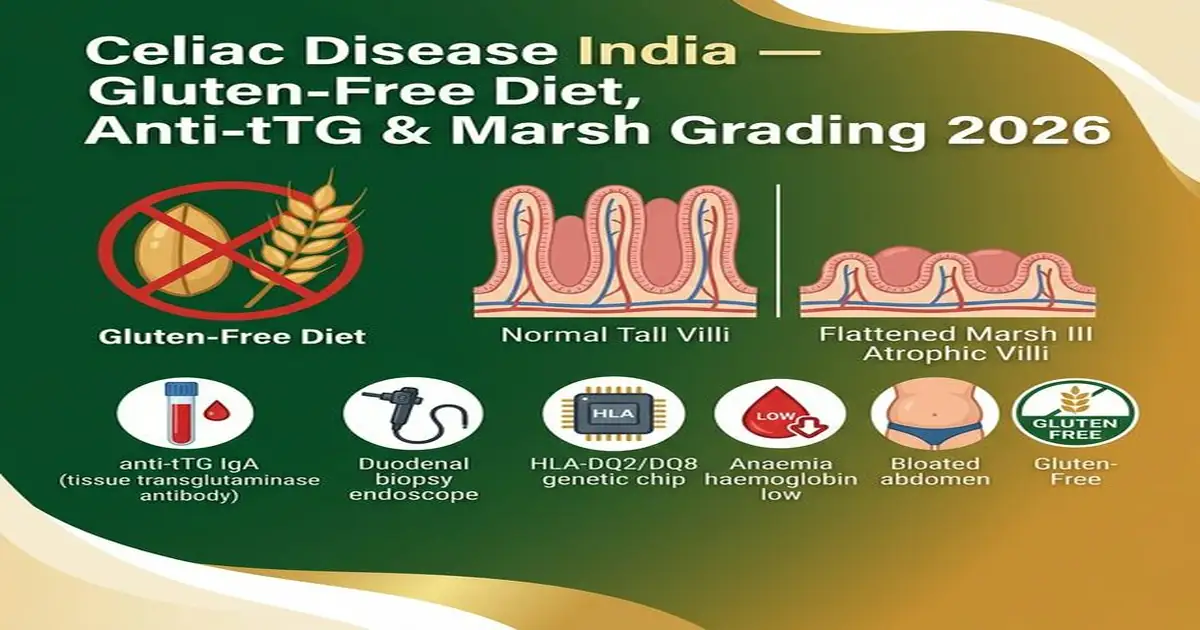
Celiac Disease India — Diagnosis, Marsh Grading and Gluten-Free Living
| Domain | Details | India Context |
|---|---|---|
| Clinical Presentations — Classic, Atypical & Silent | Classic/GI presentation (more common in children <5 years): chronic/recurrent diarrhoea (pale, bulky, offensive, floating stools — steatorrhoea from fat malabsorption); abdominal bloating and distension (prominent “pot belly” in children — from gas + fluid in lumen); weight loss / failure to thrive (inadequate caloric absorption); anorexia; irritability; Atypical/extra-intestinal presentations (more common in older children and adults): iron-deficiency anaemia refractory to oral iron (most common atypical presentation India — duodenal mucosa where iron is absorbed is destroyed → iron not absorbed → anaemia not responding to supplements); short stature (growth hormone-independent — malnutrition/malabsorption → stunting); delayed puberty; osteoporosis (calcium/Vit D malabsorption → low bone density → fractures); recurrent oral aphthous ulcers; dental enamel hypoplasia (permanent teeth — characteristic); elevated liver enzymes (hepatitis of uncertain cause — “cryptogenic hypertransaminasaemia” → coeliac screen); infertility/recurrent miscarriage (female); peripheral neuropathy; Dermatitis herpetiformis (DH — pathognomonic skin manifestation): intensely pruritic papulovesicular rash on extensor surfaces (elbows, knees, buttocks, scalp) — IgA deposits in dermal papillae; almost exclusively associated with coeliac (90%+ CD); skin biopsy DIF (direct immunofluorescence) diagnostic; Silent/subclinical coeliac: abnormal serology + histology but NO symptoms; detected only on screening of high-risk groups | India CD recognition failure: the commonest presentation of coeliac disease diagnosed in India today is NOT diarrhoea — it is refractory iron-deficiency anaemia in a young woman from Punjab/Haryana who has not responded to 3–6 months of iron supplementation; this is the index CD case India gastroenterologists most commonly see; other common India triggers: short child in class (short stature, not catching up); 15-year-old girl with delayed menarche + microcytic anaemia; young woman with recurrent miscarriages; chronic liver disease patient with elevated transaminases; key India clinical rule: any iron deficiency anaemia in a NORTH INDIAN patient (wheat-belt) that does not respond adequately to 3 months oral iron → coeliac disease screen with anti-tTG IgA; Dermatitis herpetiformis India: under-recognised; itchy rash on elbows/knees → misdiagnosed as scabies, eczema, contact dermatitis; DIF of skin biopsy (from uninvolved perilesional skin) → granular IgA in dermal papillae = coeliac confirmed |
| Diagnosis — Anti-tTG IgA, Marsh Grading, Endoscopy | Serology (first step): Anti-tissue transglutaminase IgA (anti-tTG IgA): sensitivity 95%, specificity 95%; BEST single screening test for coeliac; MUST be tested while patient is still on gluten-containing diet (if already GFD → serology may be falsely negative → challenge with gluten 14g/day × 6 weeks before testing); Anti-endomysial antibody IgA (AEA IgA): specificity ~99% — confirmatory; less widely available; Anti-deamidated gliadin peptide IgG (DGP IgG): useful when total IgA deficiency (selective IgA deficiency in 2–3% of coeliac population → anti-tTG IgA falsely negative despite coeliac → must test DGP IgG or anti-tTG IgG); total serum IgA: check simultaneously with anti-tTG IgA (if IgA <0.07 g/L = deficient → switch to IgG-based tests); HLA-DQ2/DQ8 testing: NOT used to diagnose CD (90% of general population HLA-DQ2 → high false positive); used to EXCLUDE CD (absence of DQ2 AND DQ8 → coeliac nearly impossible — very high NPV ~100%) — useful in equivocal cases or if patient already on GFD; Upper GI endoscopy + duodenal biopsy: confirmatory (required before GFD in adults for definitive histological diagnosis); findings: scalloping of duodenal folds; mosaic pattern; Marsh Grading (modified Marsh-Oberhuber): Marsh 0: normal; Marsh I: increased IELs (intraepithelial lymphocytes ≥25 per 100 enterocytes) — mild/equivocal; Marsh II: Marsh I + crypt hyperplasia; Marsh IIIA: partial villous atrophy; Marsh IIIB: subtotal villous atrophy; Marsh IIIC: total villous atrophy — classic coeliac; take ≥4 biopsies from D2 and D1 (patchy distribution → single biopsy may miss); Paediatric diagnosis (ESPGHAN 2020): if anti-tTG IgA ≥10× upper limit of normal + AEA positive + HLA-DQ2/DQ8 positive → coeliac confirmed WITHOUT endoscopy (paediatric no-biopsy pathway) | India diagnosis access: anti-tTG IgA ELISA: ₹400–800; widely available at NABL labs, most hospital labs; anti-endomysial antibody: less available (AIIMS, CMC Vellore, SRL Diagnostics, Metropolis); upper GI endoscopy with biopsy: ₹3,000–8,000 private; free at government medical college hospitals; India specific: no-biopsy pathway (ESPGHAN 2020) increasingly adopted for paediatric CD — avoids endoscopy under GA in children if serological criteria met + HLA available; HLA DQ2/DQ8 testing India: ₹5,000–15,000 (4basecare, Medgenome, Strand Life Sciences); not widely available — used selectively; AIIMS Delhi Gastroenterology: one of highest-volume coeliac centres in Asia (runs dedicated coeliac clinic); SGPGI Lucknow, Fortis Hospital: high-volume CD centres in North India |
| Gluten-Free Diet — The Only Treatment | Strict lifelong GFD: remove ALL wheat, barley, rye, and their derivatives; even trace gluten (<20 ppm — Codex Alimentarius threshold for “gluten-free”) causes mucosal damage in strictest patients; GLUTEN CONTAINS: all wheat products (atta/maida/semolina/suji/dalia/daliya; roti, chapati, paratha, puri, naan, kulcha, bread, biscuits, cakes, pasta, macaroni, spaghetti, noodles, seviyan/vermicelli [wheat-based]) ; barley (barley water, barley atta, kadha containing barley, beer); rye (rare India); Hidden gluten (major trap India): soy sauce (contains wheat); commercial atta-mixed flours; glucose syrup from wheat; communion wafers; medications (tablets may use wheat starch as excipient); dextrin (sometimes wheat-derived); artificial colours/flavours (may have wheat derivatives); SAFE gluten-free grains: rice (chawal — staple — unprocessed); maize/corn (makka atta); jowar (sorghum); bajra (pearl millet); ragi (finger millet — nachni); kuttu (buckwheat — gluten-free despite name); amaranth (rajgira); quinoa; millets; sama (barnyard millet); SAFE protein: all pulses/dals (moong, masoor, chana, urad); all vegetables; all fruits; eggs; meat; fish; dairy (milk, curd, paneer — if plain, no additives); MONITORING after GFD: anti-tTG IgA: repeat at 6 months and 12 months after GFD → should fall to normal (titre fall confirms compliance + mucosal recovery); symptom response: typically dramatic — diarrhoea resolves in 2–4 weeks; anaemia recovers in 3–6 months; bone density (DEXA scan): baseline + repeat at 2–5 years; add calcium 1000mg/day + Vit D 2000 IU/day; repeat endoscopy: after 1–2 years in adults to confirm mucosal recovery (Marsh 0 or I) — not mandatory if serology normalised and asymptomatic | GFD India challenges: wheat is THE staple in North India — social and cultural barrier enormous (“she can’t eat roti?”); cross-contamination: roti tawa shared with family → contamination → ongoing damage; flour-milling on same grinder as wheat; restaurants: impossible to guarantee gluten-free cooking in Indian kitchens (atta tawa, shared oil); gluten-free flour availability: rice flour (chawal atta), bajra atta, jowar atta, ragi atta, kuttu atta: widely available in Indian supermarkets (₹50–150/kg); gluten-free atta blends (specifically labelled): Salgaon, Diethood, Gluten-Free India brands: ₹300–500/kg; prescription GFD India: no reimbursement system for GFD cost (unlike UK — NHS GFD prescription); India resources: Celiac Society of India (celiacsocietyindia.com); online India coeliac WhatsApp groups (recipe sharing); Zomato/Swiggy “gluten-free” tag: use with caution (restaurants may not understand cross-contamination); certified GFD restaurant database: beginning in Bangalore, Mumbai, Delhi |
| Complications of Untreated or Poorly-Controlled Celiac | Short-term: malabsorption of iron, calcium, Vitamin D, folate, B12, fat-soluble vitamins (ADEK) → deficiency syndromes; Long-term (if untreated OR poorly compliant): Osteoporosis (low BMD → fragility fractures — hip, vertebral, wrist → spine fractures India common in middle-aged women with undiagnosed CD); Lymphoma (Enteropathy-Associated T-Cell Lymphoma — EATL): most feared complication of untreated/refractory CD; 4–10× higher lymphoma risk in severe untreated CD vs general population; NOT seen in well-controlled GFD-adherent patients; Refractory Celiac Disease Type I/II (RCD): persistent villous atrophy + symptoms despite strict GFD × ≥12 months; RCD-II: aberrant IEL T-cell population (premalignant — EATL precursor) → management with immunosuppression (budesonide, azathioprine, cladribine); Small bowel carcinoma: 2–3× increased risk; Functional hyposplenism: immune dysfunction (IgA deficiency + functional asplenia in some CD → pneumococcal, HiB vaccines recommended); Non-responsive CD: persistent symptoms/serology elevation on apparently strict GFD → commonest cause: dietary indiscretion (inadvertent gluten ingestion) → dietitian review → eliminate hidden gluten sources; second: refractory CD; third: co-existing condition (SIBO — small intestinal bacterial overgrowth, microscopic colitis, IBS, pancreatic exocrine insufficiency) | India EATL: relatively rare (EATL less common India absolute number vs Europe — possibly related to different CD duration before diagnosis, different dietary patterns); however: elderly patient with previously well-controlled CD developing new weight loss, abdominal pain, fever → EATL must be excluded (CT enterography + capsule endoscopy + FDG-PET); SIBO and CD India: extremely common co-occurrence — persistent diarrhoea on GFD in India → check for SIBO (hydrogen breath test — glucose H2 breath test) + empirical rifaximin 400mg TID × 14 days; lactose intolerance: secondary to CD (villous atrophy → reduced lactase → lactose malabsorption → diarrhoea) — resolves with mucosal recovery on GFD; temporary lactose restriction (1–3 months) during initial GFD may help; India-specific: milk-based diet post CD diagnosis — temporary lactose restriction often required initially |
| Screening High-Risk Groups & Associated Conditions | First-degree relatives: siblings 10%, parents/children 5% risk of CD → screen all 1st-degree relatives with anti-tTG IgA; Associated autoimmune conditions (screen for CD and screen within CD for these): Type 1 Diabetes (T1DM): 5–10% of T1DM have CD; annual anti-tTG IgA in all T1DM; autoimmune thyroid disease (Hashimoto’s thyroiditis, Graves’ disease): 2–5% CD prevalence; Down syndrome (Trisomy 21): 5–12% CD — screen with anti-tTG IgA; Turner syndrome: 4–8%; Williams syndrome: 5%; IgA nephropathy: screen; Selective IgA deficiency: test with anti-tTG IgG (not IgA) in IgA deficient; Unexplained elevated transaminases (ALT/AST): CD in 9% cases (“coeliac hepatitis”); Primary Sclerosing Cholangitis screening; Associated skin: Dermatitis herpetiformis; Psoriasis (modest association); Associated neurology: gluten ataxia (anti-gliadin IgG antibodies + cerebellar ataxia — rare but important); peripheral neuropathy | India screening implementation: anti-tTG IgA in ALL T1DM patients at diagnosis and every 2 years → almost never done in routine practice; North Indian children with Down syndrome: rarely screened for CD; opportunity: paediatric endocrinology clinics (AIIMS, KEM) should screen all T1DM for CD systematically; refractory transaminase elevation (ALT/AST 2–3× ULN × >6 months without viral/fatty liver cause) → coeliac screen mandatory; family screening India: cascade testing of 1st-degree relatives after index CD case diagnosis → almost never done — family members informed but not systematically tested; Coeliac Society India (CSI): advocating for systematic family screening + nationwide CD awareness, working with IAP (Indian Academy of Paediatrics) on paediatric CD guidelines |
Frequently Asked Questions
Is celiac disease the same as gluten intolerance — and should I go gluten-free even without a diagnosis?
The terms “celiac disease,” “gluten sensitivity,” and “gluten intolerance” are frequently confused — including by healthcare providers in India — leading to both under-treatment of true CD and over-diagnosis of non-CD conditions with unnecessarily restrictive diets: The three distinct conditions involving gluten: 1. Celiac Disease (CD): autoimmune — anti-tTG IgA positive, Marsh III histology, HLA-DQ2/DQ8, lifelong GFD mandatory; complications include EATL, osteoporosis, lymphoma if untreated; 2. Non-Celiac Gluten Sensitivity (NCGS): gluten-triggered symptoms (bloating, diarrhoea, brain fog, fatigue) WITHOUT anti-tTG antibodies, WITHOUT villous atrophy, WITHOUT HLA-DQ2/DQ8 necessarily; diagnosis of exclusion (CD excluded + IBS excluded + wheat allergy excluded, then NCGS possible); mechanism: possibly FODMAPs in wheat (fructans) rather than gluten per se (Biesiekierski 2013 double-blind crossover); GFD often helps symptoms (possibly FODMAP restriction effect); not associated with long-term complications; GFD not mandatory lifelong — can liberalise based on tolerance; 3. Wheat Allergy: IgE-mediated allergy to wheat proteins (NOT gluten specifically) — immediate urticaria, angioedema, anaphylaxis after wheat ingestion; skin prick test/wheat-specific IgE positive; not autoimmune; can improve/resolve over time; managed with wheat avoidance. The India trend problem — going GFD without diagnosis: India trend: “I feel better when I avoid wheat — I must have celiac” → self-start GFD without testing → returns 6 months later to gastroenterologist; problem: starting GFD before diagnostic testing makes CD diagnosis impossible (serology normalises, histology recovers) → either must do prolonged gluten challenge (6 weeks eating gluten) to retest — very unpleasant — or HLA-DQ2/DQ8 (exclusion only); correct sequence MANDATORY: (1) get tested FIRST while still on gluten diet → (2) anti-tTG IgA test → (3) if positive → endoscopy biopsy → (4) Marsh III confirmed → (5) THEN start GFD; “Should I go gluten-free without a diagnosis?”: NO — not if you think you might have celiac; get tested first; if CD excluded (negative serology + normal biopsy on gluten diet) and symptoms still present → NCGS possible → empirical GFD trial is reasonable; if CD confirmed → GFD is lifelong mandatory, not optional; self-diagnosed “celiac” on GFD: frequently seen India — many such patients do NOT have true CD (some have NCGS, some have IBS, some have nothing) → false diagnosis leads to unnecessary lifelong restriction + may miss the real diagnosis.
How do I maintain a gluten-free diet in India — a practical guide?
Living gluten-free in India requires knowledge of Indian food composition, vigilance about hidden gluten, and confident communication with family and food providers — here is a practical guide tailored specifically to the Indian context: Safe Indian staple foods (naturally gluten-free): Rice (all forms — plain rice, rice flour roti, idli, dosa, uttapam, poha/flattened rice, muri/puffed rice) — SAFE; all South Indian rice-based cuisine is largely naturally GFD; Jowar (sorghum flour) rotis — SAFE; Bajra (pearl millet) rotis — SAFE; Ragi (finger millet/nachni) rotis/porridge — SAFE; Kuttu (buckwheat) rotis — SAFE (despite “wheat” in English name — botanically not a grain — gluten-free; used in Navratri fasting in India — already gluten-free fasting tradition!); Rajgira (amaranth) laddoos/rotis — SAFE; Sama (barnyard millet) rice — SAFE (Navratri fasting food); all dal/legumes (moong, masoor, chana, rajma, urad, toor) — SAFE if not mixed with wheat flour; all plain vegetables — SAFE; all plain fruits — SAFE; plain paneer, plain dahi (curd), plain milk — SAFE; rice noodles (rice vermicelli — chawal seviyan vs wheat seviyan — check label); Dangerous Indian foods (contain gluten — avoid strictly): All wheat atta rotis/chapati/paratha/puri/naan/kulcha; maida products (bread, biscuits, namkeen mathri, samosa, cake, pastry); suji/semolina (upma, rava idli/dosa — UNSAFE — rava = semolina = durum wheat); dalia (broken wheat porridge); seviyan/vermicelli IF wheat-based (check label — “wheat seviyan” vs “rice seviyan”); soy sauce (contains wheat — use coconut aminos or tamari certified GFD instead); most commercial biscuits/cookies; maggi/other wheat noodles; beer (barley — use cider or rice wine/wine instead); flavoured crisps (may have wheat flour coating — check label); commercial spice mixes (may contain wheat flour as anti-caking); Cross-contamination prevention India (critical): Separate tawa (griddle) for GFD rotis in household; separate flour container; separate colander/strainer; separate storage area (not next to wheat atta); inform domestic worker about contamination risk; eating out: South Indian restaurants (idli/dosa/rice-based) safer than North Indian (roti-based); inform restaurant: “No wheat, no maida, no suji — allergy” (food allergy language more understood than “celiac”); dedicated GFD restaurants in metro cities (Delhi, Mumbai, Bangalore): use Celiac Society India restaurant guide; travel in India: carry gluten-free snacks (rice cakes, roasted poha, kuttu crackers — available online); air travel: request GFD meal in advance (most airlines accommodate); Monitoring your adherence India: anti-tTG IgA every 6–12 months (should be negative/minimal) — best objective adherence marker; if tTG rising — hidden gluten somewhere → dietitian review; join Celiac Society India online community — recipe groups, restaurant reviews, product reviews by Indian CD patients.
What to Read Next
- Anaemia — Celiac = Most Common Cause of Refractory Iron-Deficiency Anaemia India; Anti-tTG Before IV Iron in Any Unexplained IDA; GFD Restores Iron Absorption
- IBS — Celiac vs IBS: Exclude CD First in Every IBS Patient with North Indian Wheat Diet; Anti-tTG IgA + Endoscopy; Different Treatment Pathways
- Osteoporosis — Celiac Bone Disease: Calcium + Vit D + GFD; DEXA Baseline at Diagnosis; Bisphosphonate Only After GFD Established + Ca/VitD Replete
- Type 1 Diabetes — T1DM + Celiac: 5-10% T1DM Have CD; Annual Anti-tTG Screening; GFD Improves T1DM Glycaemic Control; Coeliac Hepatitis in T1DM
- Thyroid — Hashimoto Thyroiditis + Celiac: Screen Anti-tTG in All Autoimmune Thyroid; GFD May Reduce TPO Antibody Titre; Treat Both Conditions
A 14-year-old girl from Ludhiana, Punjab — the shortest girl in class 9. Hb: 8.2 g/dL. Taking iron syrup for 8 months — no improvement. Paediatrician: anti-tTG IgA ordered: 127 U/mL (normal <10). Upper GI endoscopy: Marsh IIIC — complete villous atrophy. Diagnosis: coeliac disease. Dietitian referral. Family counselled: no roti, no bread, no biscuits — jowar/bajra/rice only. Three months later: Hb 11.5 g/dL. Six months later: growing 4cm in 6 months (first time in 3 years). One year later: Hb 13.1 g/dL, anti-tTG 8 U/mL (normal). “She’s eating rice rotis now — the rest of us are also trying jowar rotis and they’re actually delicious.” The wheat she could not digest had stunted her for 5 years. The test cost ₹600. The diet change cost zero extra. Eight months of iron syrup: ₹4,000. Wasted — because no one screened for coeliac.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on BSG Coeliac Disease Guidelines 2014 (updated 2021), ESPGHAN Coeliac Guidelines 2020, AIIMS Gastroenterology Coeliac India Protocol, and Celiac Society of India resources. Last updated: March 2026.
🌾 Refractory Anaemia Not Responding to Iron? Get Anti-tTG IgA Test: If you have taken iron tablets for 3+ months and your haemoglobin is not improving — especially if you are from North India (Punjab, Haryana, UP, Rajasthan, Delhi) where wheat is the staple — ask your doctor for anti-tissue transglutaminase IgA (anti-tTG IgA) blood test. Cost: ₹400–800 at any NABL lab. If elevated: endoscopy biopsy confirms coeliac. Do NOT start gluten-free diet before testing — it makes diagnosis impossible.
⚠️ Do NOT Start Gluten-Free Diet Before Testing: Starting GFD before anti-tTG IgA and endoscopy causes false-negative results — making coeliac disease impossible to diagnose properly. Always test first while still eating wheat. If coeliac confirmed → strict lifelong GFD. If excluded → GFD can still be tried for symptom relief but is not medically mandatory.
⚕️ Medical Disclaimer: This article provides general educational information about coeliac disease. All serological testing interpretation, endoscopy biopsy assessment, Marsh grading, and management of complications (RCD, EATL, osteoporosis) require qualified gastroenterologist and dietitian assessment. GFD in young children requires paediatric dietitian involvement to ensure nutritional adequacy.
