Last Updated: March 2026 | Reading Time: 10 minutes | ~2,100 words
India is in the grip of a heart attack epidemic — and it is getting younger. India accounts for 60% of the world’s heart disease burden despite having only 18% of the global population. More alarmingly, Indians have heart attacks 10 years earlier than Western populations — with a significant proportion occurring in people under 40. Most heart attack deaths in India are preventable — and most occur not because treatment is unavailable, but because the warning signs are not recognised, valuable time is wasted, and the victim reaches hospital too late. This guide could save your life — or someone you love.
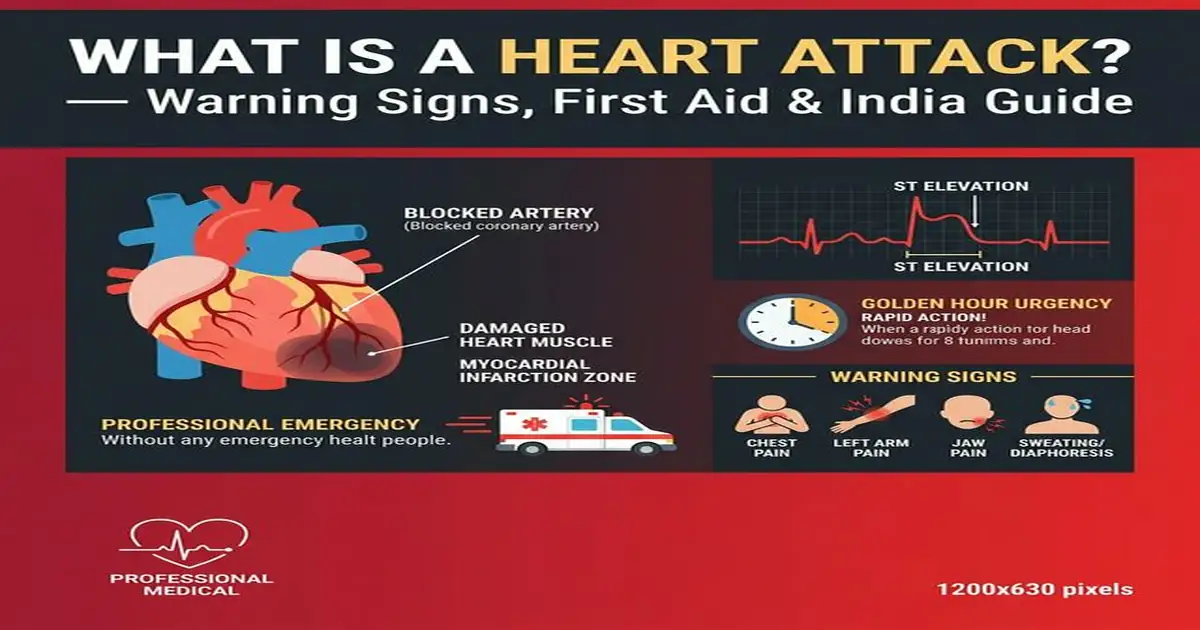
What Exactly is a Heart Attack?
A heart attack (medically: Myocardial Infarction or MI) occurs when blood supply to a section of the heart muscle is completely blocked — causing that section to begin dying from lack of oxygen. The heart muscle (myocardium) requires a constant supply of oxygenated blood through three coronary arteries. Over years, cholesterol and inflammatory plaque builds up inside these arteries (atherosclerosis), narrowing them. A heart attack typically occurs when a plaque suddenly ruptures — exposing its contents to the bloodstream, triggering an instant blood clot (thrombus) that completely blocks the artery. Blood flow stops. The heart muscle cells in the zone supplied by that artery start dying within 20 minutes. Every minute of continued blockage kills more heart muscle. Hence the cardiac emergency mantra: “Time is muscle — muscle is life.”
Types of Heart Attack
| Type | Full Name | ECG Finding | Urgency | Treatment |
|---|---|---|---|---|
| STEMI | ST-Elevation Myocardial Infarction | ST segment elevation — complete blockage | 🚨 Extreme — minutes matter | Emergency angioplasty (PCI) within 90 min; or thrombolysis within 30 min if PCI unavailable |
| NSTEMI | Non-ST-Elevation MI | ST depression or T-wave changes — partial blockage | 🔴 Urgent — hours matter | Urgent angiography + PCI within 24–72 hrs; anticoagulants |
| Silent MI | Painless heart attack | Often found incidentally on ECG (old Q waves) | ⚠️ Diagnosed late | Standard post-MI treatment once identified; higher risk in diabetics |
🚨 Heart Attack Warning Signs — Know Every One
The most dangerous misconception: that a heart attack always feels like a dramatic crushing chest pain. Many Indians — particularly women and diabetics — have “atypical” presentations without classic chest pain. Know ALL the warning signs:
| Warning Sign | Description | How Common |
|---|---|---|
| Chest discomfort / pressure / pain | Heaviness, tightness, squeezing, or pressure in the centre or left of chest; may come and go or be constant. NOT always “crushing” or “sharp” | Most common — 70–80% of MIs |
| Pain radiating to left arm | Dull ache or numbness down the left arm — the classic “Hollywood” sign; can be either arm or both | 50–60% |
| Jaw, neck, or throat pain | Unexplained jaw ache, throat tightness, or neck pain — often dismissed as tooth or neck problem | 30–40%, especially in women |
| Breathlessness (with or without chest pain) | Sudden difficulty breathing even at rest or with minimal activity — particularly alarming if new | 40–60% |
| Cold sweat and clamminess | Sudden profuse sweating with pale, cold, clammy skin — the body diverting blood from skin to heart | 50–60% |
| Nausea and vomiting | Unexplained sudden nausea, especially in the elderly — frequently dismissed as acidity or food poisoning | 30–50%, higher in inferior MI |
| Extreme fatigue | Overwhelming, sudden, unexplained fatigue — especially in women in the days before a heart attack | Very common in women (70%) |
| Dizziness or fainting | Light-headedness, near-fainting, or actual loss of consciousness — indicates poor cardiac output | 20–30% |
| Epigastric pain (upper abdomen) | Pain felt in upper abdomen rather than chest — very frequently confused with acidity, especially inferior MI | 20–30%, often leads to missed diagnosis |
🚨 The most dangerous Indian habit during a heart attack: Taking antacids for chest pain and waiting hours to see if it resolves. Upper abdominal pain, jaw pain, sweating, and breathlessness during a suspected heart attack require calling 108 IMMEDIATELY — not waiting to see if “acidity settles.”
Heart Attack First Aid — What to Do (and NOT Do) Right Now
- ☎️ Step 1 — Call 108 (India emergency) IMMEDIATELY. Do not drive yourself. Do not wait. Do not watch and see. Call now. Tell them “possible heart attack” so a cardiac-capable ambulance is dispatched.
- 🛋️ Step 2 — Rest immediately. Sit or lie the patient down in the most comfortable position (usually semi-reclined). Stop all physical activity.
- 💊 Step 3 — Aspirin 325mg (or 150mg) — chew, do NOT swallow whole. If available and the patient is not aspirin-allergic, give one aspirin tablet to chew (not swallow) — this dissolves the clot-forming platelets faster. This alone saves lives. Keep aspirin at home.
- 👔 Step 4 — Loosen tight clothing. Remove tie, unbutton collar, loosen belt — reduce any restriction on breathing and chest.
- 🧘 Step 5 — Stay calm and reassure the patient. Anxiety raises adrenaline which worsens heart workload. Keep the patient as calm as possible while waiting for ambulance.
- 💨 Step 6 — If the patient becomes unconscious and has no pulse — start CPR immediately. Push hard and fast in the centre of the chest — 100–120 compressions per minute. Do not stop until ambulance arrives.
- ❌ Do NOT give water or food — patient may need emergency surgery
- ❌ Do NOT give ibuprofen (Brufen) or naproxen — NSAIDs worsen outcomes in heart attacks
- ❌ Do NOT let the patient walk or climb stairs during an active MI
- ❌ Do NOT delay hospital — every 30-minute delay = 7.5% higher mortality
The Golden Hour — Why Time to Treatment is Everything
| Time Since Heart Attack | Heart Muscle Loss | Survival & Outcome |
|---|---|---|
| 0–30 minutes | Minimal — very early; reversible ischaemia | Best outcomes; near-complete recovery possible with immediate PCI |
| 30–90 minutes (golden hour) | Moderate loss beginning; some cells dying | Excellent outcomes with emergency angioplasty (PCI) — “door-to-balloon” within 90 min target |
| 90 min – 3 hours | Significant muscle loss; infarct enlarging | Good outcomes still possible; thrombolysis (clot-busting drug) very effective if PCI unavailable |
| 3–6 hours | Major loss; infarct nearly complete | Treatment still reduces mortality significantly but recovery is more limited |
| > 6 hours | Established infarct; most damage done | Treatment prevents extension; manages complications; cardiac rehabilitation critical |
| > 12 hours | Full infarct; scarring beginning | No benefit from opening artery (late PCI) in stable patients; medical management + rehab |
Why Indians Have Heart Attacks Earlier — Risk Factors
| Risk Factor | Indian Context | Modifiable? |
|---|---|---|
| Atherogenic dyslipidaemia (High TG, Low HDL) | Most common Indian lipid pattern — high-sugar, high-refined carb diet | ✅ Yes |
| Type 2 Diabetes | 101 million Indians with diabetes — 2–4× higher MI risk | ✅ Yes |
| Hypertension | 220 million Indians with high BP — #1 risk factor for MI and stroke | ✅ Yes |
| Tobacco use (smoking + chewing) | 267 million Indians use tobacco; smoking doubles MI risk | ✅ Yes |
| Abdominal obesity | High waist, low BMI possible — visceral fat = higher risk | ✅ Yes |
| Physical inactivity | Sedentary urban and rural India alike — independent MI risk factor | ✅ Yes |
| Stress / psychological factors | India-specific: job stress, financial stress, sleep deprivation — cortisol-driven MI risk | ✅ Partially |
| South Asian genetics | GWAS studies confirm South Asians have higher genetic predisposition to early coronary artery disease | ❌ No — but lifestyle modifications are MORE impactful precisely because of genetic risk |
Frequently Asked Questions
What is the difference between a heart attack and cardiac arrest?
This is one of the most important medical distinctions that every Indian should know — because the response required is completely different. A heart attack is a plumbing problem — a blockage in a coronary artery cuts off blood supply to heart muscle. The heart continues beating but its muscle is dying progressively. The patient is usually conscious, in pain, and can speak. There is time (though not much) to get to a hospital. A cardiac arrest is an electrical problem — the heart’s electrical system fails, causing the heart to stop beating entirely (ventricular fibrillation or asystole). The patient immediately loses consciousness and stops breathing. There is NO time — brain death begins within 4–6 minutes without CPR. The survival rate of cardiac arrest without bystander CPR and defibrillation within 6 minutes is less than 10%. Key connection: An untreated heart attack can trigger cardiac arrest (the dying heart muscle disrupts electrical conduction) — which is why rapid treatment of a heart attack is so critical. If someone collapses, loses consciousness, and is not breathing — that is cardiac arrest. Start CPR immediately (100–120 chest compressions/minute, hard and fast) and call 108 — every minute without CPR reduces survival by 10%.
Can a young, fit person have a heart attack?
Yes — and in India, this is occurring at an alarming and increasing rate. Multiple high-profile cases of young, apparently fit Indians dying suddenly (many during exercise or sport) reflect a combination of: Familial Hypercholesterolaemia (FH) — genetic condition causing very high LDL from birth; can cause heart attacks in the 20s and 30s even with perfect lifestyle. Affects 1 in 250 Indians — undiagnosed in most. Hypertrophic Cardiomyopathy (HCM) — genetic thickening of heart muscle; the most common cause of sudden cardiac death in young athletes. Often completely silent until the fatal event. Premature coronary artery disease in South Asians — studies show Indians develop coronary plaque 10 years earlier, often with lower LDL than Western standards but higher TG levels. Cocaine and other stimulant use — causes acute coronary spasm and clot formation; increasingly relevant in urban India. Stress + sleep deprivation + metabolic syndrome — the “young professional” pattern of chronic stress, poor sleep, high-sugar diet, and no exercise creating premature atherosclerosis. The takeaway: any young Indian with a family history of early heart disease, recurrent unexplained chest pain, or syncope (fainting) during exercise should have a thorough cardiac evaluation — ECG, echocardiogram, lipid profile, and possibly stress test — regardless of age and apparent fitness.
What happens after a heart attack — recovery guide?
Surviving a heart attack is the beginning of a long-term management journey —not the end point. Post-MI recovery and prevention of future attacks involves: Medications (usually lifelong): Dual antiplatelet therapy (aspirin + clopidogrel/ticagrelor) for 12 months post-PCI; statin (high-intensity — atorvastatin 80mg or rosuvastatin 20–40mg) to aggressively lower LDL; beta-blocker (metoprolol, bisoprolol) to reduce heart workload; ACE inhibitor/ARB (ramipril, telmisartan) to protect heart function; sometimes aldosterone antagonist (spironolactone) if heart function is significantly impaired. Cardiac rehabilitation: A structured programme of supervised exercise, education, and psychological support — shown to reduce mortality by 25–30% after MI. Sadly underutilised in India. Lifestyle overhaul: Complete tobacco cessation (non-negotiable); Mediterranean-style diet; regular moderate exercise (30 min daily walking, building to more); weight management; stress reduction. Follow-up monitoring: Echocardiogram after 6 weeks to assess heart function (ejection fraction); regular lipid profile, HbA1c, blood pressure monitoring; nuclear stress test or repeat angiography if symptoms return. Return to work: Most patients can return to desk work in 2–4 weeks; physically demanding jobs take 6–12 weeks; driving can resume after 4 weeks if no complications; sexual activity after 4–6 weeks. Depression after MI affects 20–30% of patients — recognition and treatment is as important as physical recovery.
Is acidity or gas pain the same as heart attack pain?
This distinction is critically important in India because upper abdominal pain and “gas” are so universally attributed to acidity that true cardiac pain is frequently missed. Key differences: Acidity/GERD: Burning sensation (not pressure/heaviness); typically after eating or lying down; improves with antacids; associated with sour belching; no sweating or breathlessness; no arm/jaw radiation; no breathlessness. Heart attack: Pressure, heaviness, or squeezing (even if felt in upper abdomen); may worsen with physical activity; does NOT reliably improve with antacids (this is a critical test — antacids can temporarily mask associated burning but the fundamental pressure/discomfort persists); associated with sweating, breathlessness, or nausea; may radiate to jaw, neck, or left arm. The dangerous scenario: A patient with inferior MI (blockage of the right coronary artery) presents with upper abdominal pain and vomiting — and is given antacids by the family for 3–4 hours before seeking cardiac care. This delayed presentation is extremely common in India and leads to preventable death. The rule: any upper abdominal pain associated with sweating, breathlessness, or radiation to jaw/arm — even without classic chest pain — is cardiac until proven otherwise. Seek emergency care immediately; do not take antacids and wait.
What is angioplasty and do I need it after a heart attack?
Angioplasty (formally: Percutaneous Coronary Intervention or PCI) is the standard emergency treatment for STEMI (complete blockage heart attack). A catheter is inserted through the wrist (radial approach — most common in India now) or groin, guided to the blocked coronary artery under X-ray, and a balloon is inflated to open the blockage. A stent (small metal mesh tube) is then deployed to keep the artery open permanently. In India’s best cardiac centres, this procedure takes 45–60 minutes from arrival, can be done under local anaesthesia without general anaesthesia, and patients typically walk the next day. The target time: “door-to-balloon” under 90 minutes — the time from hospital arrival to coronary artery being opened. PCI reduces mortality by 25–30% compared to no intervention in STEMI. When PCI is not immediately available (in smaller towns or during transfer), thrombolysis (clot-busting injection — streptokinase or tenecteplase) can be given within 30 minutes of hospital arrival — effective in 50–70% of cases and buys time until PCI can be performed (“pharmaco-invasive strategy”). Not every heart attack requires PCI — NSTEMI management is more individualised based on risk score, symptoms, and ECG findings. Post-PCI, two antiplatelet drugs are required for at least 12 months to prevent stent clotting — stopping these early is a common cause of death after angioplasty in India.
What to Read Next
- What is Cholesterol? — The Primary Driver of Heart Attacks
- High Blood Pressure — #1 Modifiable Risk Factor for MI and Stroke
- Diabetes India — 2–4× Higher Heart Attack Risk
- Control Blood Sugar — Reversing Metabolic Risk Protects Your Heart
- Fatty Liver — Metabolic Syndrome Connecting Fatty Liver & Heart Disease
Every Indian family should know two things: the phone number 108, and aspirin 325mg to chew. The leading cause of premature death in India is not cancer, not COVID — it is heart disease. Recognise the signs, act in seconds, chew aspirin, call 108, and get to a cath lab. Time is muscle. Muscle is life.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on CSI (Cardiology Society of India) STEMI Guidelines 2023, ACC/AHA MI Management Guidelines, and Indian cardiovascular disease epidemiology data. Last updated: March 2026.
Authoritative Sources: CSI — STEMI Guidelines India 2023 | ACC/AHA — MI Guidelines | WHO — Cardiovascular Disease | ICMR India
⚕️ Medical Disclaimer: This article is for general informational and emergency awareness purposes. If you suspect a heart attack — in yourself or anyone else — call 108 immediately. Do not use this article to self-diagnose or delay emergency care. Every minute matters.
