Last Updated: March 2026 | Reading Time: 9 minutes | ~2,100 words
Snakebite is one of India’s most devastating and underappreciated public health emergencies: India suffers the world’s highest snakebite mortality, with approximately 58,000 deaths annually — accounting for nearly half of global snakebite mortality (WHO global estimate: 81,000–138,000 deaths/year). An additional 1.2–1.4 million venomous snakebites occur annually in India, with many survivors suffering permanent disability (limb loss from tissue necrosis, renal failure, neurological sequelae). The overwhelming majority of snakebite deaths in India are rural, agricultural, and nocturnal — occurring when farmers, labourers, and children step on or disturb snakes during the night (particularly during monsoon when snakes flee flooded burrows). Access to Anti-Snake Venom (ASV) is the only life-saving treatment, yet 60–70% of snakebite victims seek initial care from traditional healers or quacks, causing treatment delays of 6–18 hours that convert survivable bites into fatalities. India’s “Big Four” venomous snakes — Russell’s viper (Daboia russelii), Common krait (Bungarus caeruleus), Indian cobra (Naja naja), and Saw-scaled viper (Echis carinatus) — account for the vast majority of medically significant bites, though the actual number of medically important species exceeds 50 in India.
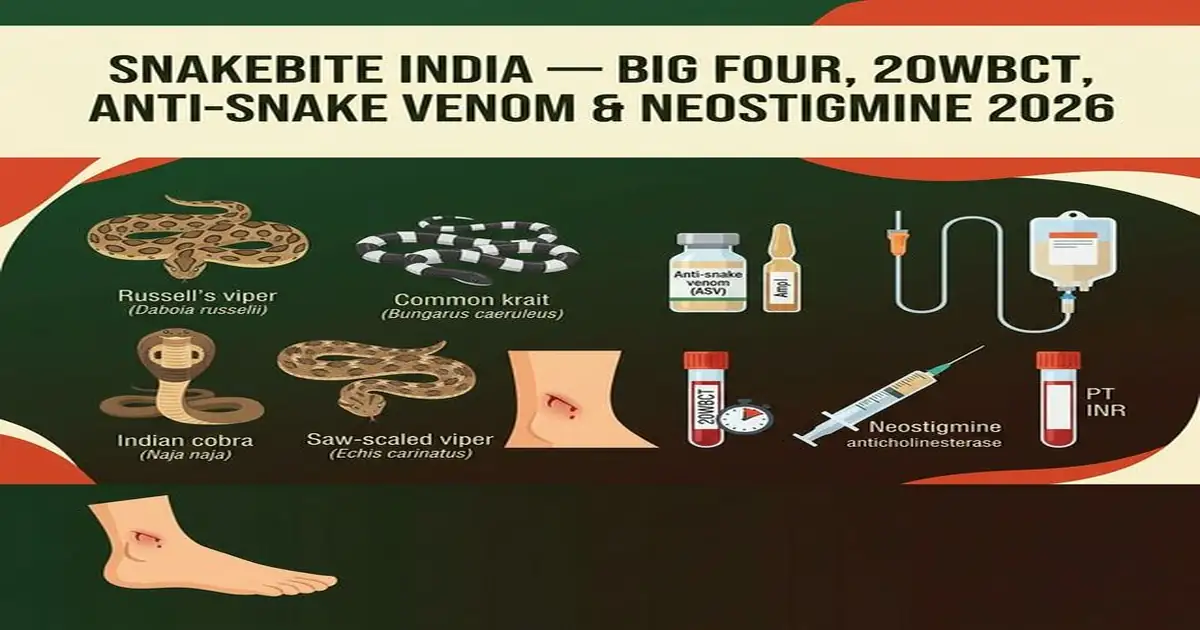
Snakebite India — Envenomation Syndrome, Diagnosis and Management
| Snake / Venom Type | Clinical Syndrome | Diagnosis | Treatment | India Notes |
|---|---|---|---|---|
| Russell’s Viper (Daboia russelii) — Haemotoxic + Neurotoxic + Cytotoxic | Local: severe swelling, bruising, blistering, tissue necrosis (commonest cause of snakebite limb loss India); Systemic: coagulopathy (DIC-like — VICC: venom-induced consumption coagulopathy — 20WBCT non-clotting; PT/INR elevated; fibrinogen depleted); spontaneous haemorrhage (gum bleeding, haematuria, haemoptysis, intracranial haemorrhage); Acute Kidney Injury (AKI — bilateral cortical necrosis; oliguria — most common cause of snakebite-AKI in India — Russell’s viper nephrotoxicity direct); neurotoxicity (ptosis, ophthalmoplegia — some Russell’s viper populations South India — local venom variation) | 20-Minute Whole Blood Clotting Test (20WBCT): bedside test — 1–2mL fresh blood drawn into clean glass tube; leave undisturbed 20 minutes at room temperature; if blood non-clotting = systemic envenomation by haemotoxic snake = ASV mandatory; repeat 20WBCT every 6 hours until clotting restored; PT/INR/aPTT (laboratory — confirms coagulopathy); fibrinogen (depleted in VICC — DIC-like); serum creatinine, urine output (AKI monitoring); platelet count | Anti-Snake Venom (ASV): India polyvalent ASV (covers all Big Four — Haffkine, VINS, Premium Serums): 10 vials IV initial dose (severe envenomation); each vial = 10mL; infuse over 30–60 minutes; repeat 20WBCT at 6 hours: if still non-clotting → repeat 10 vials; continue until 20WBCT restores; total ASV requirements in severe Russell’s viper DIC: 20–40+ vials; Fresh frozen plasma (FFP): for coagulopathy if ASV given and coagulation not restoring; AKI: strict fluid management, haemodialysis (CRRT preferred in oliguria); limb: do NOT incise/suck wound; do NOT apply tourniquet (worsens necrosis); surgical debridement after ASV for necrotic tissue; fasciotomy if compartment syndrome | Russell’s viper: highest snakebite morbidity India; AKI → dialysis → permanent renal failure in many survivors from Odisha, AP, Tamil Nadu, Karnataka; bilateral cortical necrosis = irreversible; early ASV prevents AKI (venom has direct nephrotoxic effect); haemorrhagic stroke from coagulopathy — GCS monitoring; Russell’s viper bite site: usually lower limb (paddy fields — agricultural exposure); ASV anaphylaxis: common (up to 40% patients) → adrenaline, chlorphenamine, hydrocortisone pre-treatment before ASV in high-risk patients |
| Common Krait (Bungarus caeruleus) — Neurotoxic (Presynaptic) | Local: minimal (krait venom has little local effect — fang marks may be invisible); Systemic: descending symmetrical neuromuscular paralysis — ptosis first (bilateral drooping eyelids — typically 6–12 hours post-bite); progresses to ophthalmoplegia (external eye muscle paralysis); facial weakness; dysarthria (slurred speech); dysphagia (difficulty swallowing — aspiration risk); descending limb weakness; respiratory muscle paralysis → respiratory failure → death if untreated; onset often during sleep (krait bites predominantly nocturnal — patient may wake with neurological symptoms thinking “I am having a stroke”); abdominal pain/vomiting (autonomic involvement) | Clinical: ascending/descending paralysis + bilateral ptosis + history of sleep → characteristic; 20WBCT usually normal (neurotoxic — not haemotoxic); neostigmine test: neostigmine 0.04mg/kg IM + atropine 0.02mg/kg IV — if ptosis/paralysis improves in 30 minutes = post-synaptic neurotoxin responding (cobra-type); krait = PRESYNAPTIC → neostigmine largely ineffective (once acetylcholine stores depleted at presynaptic terminal — cannot be reversed pharmacologically); CSF normal; nerve stimulation studies if available | ASV (polyvalent): 10 vials — MUST be given as early as possible (presynaptic toxin — ASV neutralises unbound venom before it irreversibly destroys presynaptic acetylcholine release); once paralysis established, ASV cannot reverse it — it only neutralises circulating free venom; Mechanical ventilation: the critical intervention — respiratory support until spontaneous recovery (krait paralysis typically reverses in 5–10 days if supported); ICU with ventilator access = determining factor for survival; neostigmine: limited benefit (presynaptic mechanism) but worth trying in mixed envenomation; aspiration prevention: NG tube feeding, semi-recumbent position | Krait is the “silent killer” — nocturnal bite during sleep, minimal local pain/swelling, patient may not know bitten (krait fang marks tiny); many krait deaths occur because patient presents in the morning with “stroke-like” weakness; no mechanical ventilator in rural hospital = near-certain death from respiratory failure; India ICU ventilator shortage: critical gap in snakebite death prevention; Maharashtra, Gujarat, Rajasthan, UP — highest krait burden; ASHA workers must be trained to recognise bilateral ptosis + nocturnal onset as krait emergency |
| Indian Cobra (Naja naja) — Neurotoxic (Post-Synaptic) + Cytotoxic | Local: swelling, necrosis (cobra venom cytotoxic — tissue damage), blistering; severe local pain; Systemic: postsynaptic neuromuscular blockade — ptosis, ophthalmoplegia, facial paralysis, respiratory muscle weakness → respiratory failure; onset 1–4 hours; RESPONDS TO NEOSTIGMINE (postsynaptic — anticholinesterase reverses paralysis by accumulating acetylcholine at NMJ); cobra also causes cardiovascular effects (hypotension, arrhythmia); “spitting cobras” — Naja species — ocular envenomation from venom spitting → corneal ulceration → irrigate immediately with water | Clinical differentiation from krait: cobra bites have MORE local envenomation (swelling/necrosis); onset faster (1–4h vs 6–12h krait); neostigmine test POSITIVE (cobra postsynaptic); 20WBCT normal (not haemotoxic); CSF normal; electrodiagnostics if available | ASV: 10 vials IV urgently; Neostigmine 0.04mg/kg IM + atropine 0.02mg/kg IV (must give atropine first — prevents neostigmine muscarinic effects — vomiting, bradycardia, bronchospasm): neostigmine reverses cobra paralysis dramatically — “reversal within 20–30 minutes” — can be repeated; Mechanical ventilation if neostigmine response inadequate or respiratory failure before neostigmine effective; wound care: cobra necrosis — debridement; eye irrigation if venom in eye (copious water irrigation 15+ minutes) | Cobra neurotoxicity is REVERSIBLE with neostigmine + ASV unlike krait; critical India message: give atropine BEFORE neostigmine; “SAVE” protocol India (Symptomatic + ASV + Ventilation + Electrolytes); cobra bites common in agricultural areas across India; Naja naja variants across India have differing cytotoxic/neurotoxic venom ratios; WBCT normal distinguishes from Russell’s viper haemotoxicity |
| Saw-Scaled Viper (Echis carinatus) — Haemotoxic | Local: pain, swelling, local necrosis; Systemic: coagulopathy (VICC — similar to Russell’s viper but often less severe); spontaneous bleeding (similar to Russell’s viper but generally milder renal involvement than Russell’s); rare neurotoxicity; characteristic sound: lateral rubbing of keeled scales creates rasping sound (“saw-scaled” — viper produces this when threatened) | 20WBCT non-clotting (haemotoxic); PT/INR elevated; fibrinogen depleted; clinical bleeding assessment; FBC (thrombocytopenia) | ASV (polyvalent): 10 vials; repeat 20WBCT 6-hourly; coagulation restoration as clinical endpoint; FFP if required; supportive care similar to Russell’s | Saw-scaled viper: Rajasthan, Gujarat, Maharashtra (dry arid regions; sandy rocky terrain — unlike Russell’s viper wetlands); highly irritable, quick-striking; sounds before strike (important warning sign to leave area); coagulopathy less severe than Russell’s viper typically; AKI less common; mortality lower than Russell’s with ASV |
| General Snakebite First Aid India — What to Do and NOT Do | DO: Keep patient calm and still (reduce lymphatic venom spread); immobilise bitten limb (splint like fracture — below heart level); reassure (90% of snakebites in India are by non-venomous snakes or dry bites); transport immediately to nearest facility with ASV; mark time of bite and progression of symptoms; DO NOT: apply tourniquet (increases local tissue damage → necrosis/gangrene); cut and suck wound (causes infection + additional tissue damage; no benefit); apply traditional herbal remedies or “stone treatment”; waste time with traditional healers; attempt to catch/kill snake (additional bite risk) | Not applicable — first aid education | Not applicable | India: 90% of patients go first to traditional healers (faith healers, jhad-phunk practitioners) — average delay to hospital 6–18 hours; this delay is the primary cause of death; community education campaigns: focus must be “go directly to hospital — tourniquet does not work — traditional treatment does not work”; AIIMS snake venom research unit; TNMSC antivenom distribution Tamil Nadu; Maharashtra ASV distribution under NRHM; WHO snakebite classified as Neglected Tropical Disease (2017) |
Frequently Asked Questions
How does the 20-Minute Whole Blood Clotting Test work — and why is it India’s most important bedside snakebite test?
The 20-Minute Whole Blood Clotting Test (20WBCT) is one of the most elegantly simple and diagnostically powerful bedside tests in all of emergency medicine — and in India’s resource-limited snakebite management context, it is absolutely central to decision-making: How to perform 20WBCT (WHO recommended method): Draw 2–3mL of fresh venous blood into a clean, dry glass tube (glass — NOT plastic; glass surface activates coagulation factors; plastic does not); place tube undisturbed at room temperature; wait 20 minutes; gently tilt the tube; if blood is clotted (solid, gelatinous — does not flow when tilted) = NORMAL coagulation = no haemotoxic envenomation = ASV may not be needed (watch and repeat); if blood is LIQUID (does not clot — flows freely when tube tilted) = COAGULOPATHY = systemic haemotoxic envenomation = ASV MANDATORY immediately; do NOT disturb the tube while waiting — movement disrupts clot formation and gives false non-clotting result. Why 20WBCT in India context: India’s polyvalent ASV is expensive, in limited supply, and causes frequent anaphylaxis (serum sickness) — yet must NOT be withheld in genuinely envenomated patients; 20WBCT resolves the dilemma in haemotoxic envenomation — objective, free, no laboratory equipment needed, available at every PHC in India; sensitivity for haemotoxic envenomation (Russell’s viper, Saw-scaled viper) approximately 85–90%; a positive 20WBCT (non-clotting blood) is DEFINITIVE evidence of systemic haemotoxic envenomation and mandates ASV — no further confirmation required; it also serves as the treatment endpoint — repeat 20WBCT at 6 hours after ASV: if clotting restored = sufficient ASV given; if still non-clotting = give another 10-vial course; 20WBCT does NOT detect neurotoxic envenomation (krait, cobra, some Russell’s viper populations) — neurotoxic syndrome must be diagnosed clinically. ASV response monitoring with 20WBCT: Pre-ASV 20WBCT: non-clotting (confirms envenomation); 6h post-ASV 20WBCT: if clotting = ASV working; if non-clotting = repeat 10 vials; 12h post-ASV 20WBCT: should be clotting by this point if adequate ASV given; continued non-clotting at 12h: consider ASV quality issue, very heavy venom load, or concurrent DIC from other cause; FFP use: give FFP AFTER ASV (not before — pro-coagulant FFP in the presence of active venom → continued clotting factor depletion with newly infused factors = wasted resource; first neutralise venom with ASV, then replace coagulation factors); platelet threshold for FFP/cryoprecipitate: fibrinogen <1 g/L or active bleeding. Limitations of 20WBCT: False negative: early bite (venom not yet fully absorbed — may be clotting at 2 hours and non-clotting at 4 hours — repeat 20WBCT at 1, 3, 6, 12 hours if clinical suspicion high); false positive: plastic tube (does not activate coagulation → blood appears non-clotting); sample tube contaminated with anticoagulants; haematological disease causing pre-existing coagulopathy; recent anticoagulant use (warfarin, heparin); does NOT test for neurotoxic envenomation — krait/cobra with normal 20WBCT can still be fatal if respiratory paralysis develops.
What should you do if bitten by a snake in rural India — and what traditional treatments are dangerous?
The single most important determinant of survival from venomous snakebite in India is NOT which snake bit you, NOT how much venom was injected, and NOT how severe your symptoms are — it is how quickly you reach a facility with Anti-Snake Venom. Everything else is secondary. And the single biggest barrier to survival is the cultural reliance on traditional healing that delays that crucial journey: The correct immediate first aid — do this NOW: Stay calm — anxiety and movement increase heart rate → increases venom absorption rate via lymphatics; keep the bitten limb immobilised and at or below heart level (splint as though fracturing — reduces lymphatic venom spread); remove tight clothing, rings, bracelets from bitten extremity (limb will swell massively); note the time of bite (crucial for clinical management — symptom timeline helps determine snake species and severity); travel to the nearest hospital with ASV IMMEDIATELY — do not stop anywhere; if possible, note the appearance of the snake (colour, head shape, markings) — but do NOT attempt to catch or kill it (additional bite risk; not essential for treatment — polyvalent ASV covers all Big Four). Dangerous traditional practices that kill people in India: Tourniquet/tight ligature: a piece of cloth/rope tied tightly above the bite — NEVER DO THIS; tourniquet concentrates venom in the limb, cuts off arterial blood supply → limb ischemia and necrosis → amputation requirement; does NOT prevent systemic venom absorption (venom absorbed through lymphatics, not blood vessels); the “tourniquet causes gangrene” complication is extremely common in India — many limb amputations post-snakebite are tourniquet-related, not venom-related; Cut and suck: traditional practice of cutting the bite site with a blade and sucking out venom — ineffective (venom absorbed within minutes), causes infection, nerve/vessel damage; Traditional stone (nagamani): black stone applied to bite — useless; Traditional herbal remedies (jaljeera, oil massage, herbal paste): delay hospital transport — the most dangerous intervention in India; Traditional healers (fakirs, snake charmers): they blow on wounds, give herbal concoctions, make anti-venom claims — go directly to hospital and do not stop at any traditional healer; Faith healing and religious rituals: families circle around the “spiritually” treated patient while venom continues to absorb; Electric shock treatment (illegal): administered in some rural areas — painful, no evidence, delays care. India snakebite death pattern — the predictable tragedy: Bite at 10pm while sleeping or walking barefoot in paddy field → family applies tourniquet → transport to local faith healer → 6 hours wasted → reach district hospital at 4am with coagulopathy, AKI, respiratory failure → insufficient ASV vials (stock-out at district hospital — requires 20–40 vials for severe Russell’s viper but district hospital has 5) → death; this pattern repeats 58,000 times per year in India; WHO’s Global Snakebite Initiative targets 50% reduction in global snakebite mortality by 2030 — India must fix community awareness AND ASV supply chain simultaneously.
What to Read Next
- Kidney — Russell’s Viper AKI: Bilateral Cortical Necrosis; CRRT Critical; Early ASV Prevents Renal Failure; Dialysis at AIIMS/JIPMER/PGI
- Malaria — Monsoon Season: Same Rural Communities Bear Both Snakebite and Malaria Burden; Dual Diagnosis Possible; Concurrent Treatment
- Leptospirosis — Monsoon Season Co-burden with Snakebite in Paddy-Farming Communities; Both Need Early Empirical Treatment
- Arthritis — Snakebite Necrosis → Limb Loss → Disability; Rehabilitation and Prosthetics After Snakebite Amputation in Rural India
- Depression — Snakebite Survivors with Disability or Limb Loss: High PTSD, Depression Rates in Rural India; Integrate Mental Health in Follow-Up
A 16-year-old boy in Odisha is walking back from his family’s paddy field at dusk. He feels a sharp pain in his right ankle. He sees a thick-bodied snake slithering away — Russell’s viper. His family ties a cloth tourniquet tightly around his knee. They take him to the village healer. Six hours later — with a gangrenous foot, actively bleeding gums, and zero urine output — he arrives at the district hospital. The doctor has three ASV vials. He needs forty. He dies of intracranial haemorrhage. He was 16 years old. In America, Europe, Australia — this bite would be survivable in any emergency room. In rural Odisha: 58,000 stories like his, every year.
About This Guide: Written by the StudyHub Health Editorial Team (studyhub.net.in) based on WHO Guidelines for the Management of Snakebites in South-East Asia (2nd edition, 2016), India National Snakebite Management Protocol (DGHS 2021), and the Lancet Commission on Snakebite 2024 data. Last updated: March 2026.
🐍 Snakebite = Medical Emergency: NO Tourniquet — NO Traditional Healer — GO DIRECTLY TO HOSPITAL: If bitten by a snake: (1) Stay calm. (2) Do NOT apply tourniquet — this causes gangrene. (3) Do NOT go to a traditional healer. (4) Go directly to the nearest Government hospital with ASV. (5) Immobilise the bitten limb. Tell the doctor the time of bite and describe the snake. Every hour of delay increases your chance of death.
💉 Anti-Snake Venom is Free at Government Hospitals: India’s polyvalent Anti-Snake Venom (ASV) covers all four Big Four snakes (Russell’s viper, Krait, Cobra, Saw-scaled viper) and is available free-of-cost at government district hospitals and medical colleges. Demand it. If your district hospital is out of stock — insist on transfer to the nearest medical college hospital. ASV is the ONLY cure for snakebite. No traditional remedy, no tourniquet, no electric shock — only ASV.
⚕️ Medical Disclaimer: This article provides general educational information about snakebite management. ASV dose, 20WBCT interpretation, neostigmine use, and ICU management of severe envenomation require qualified emergency medicine/toxicology specialist assessment. Do not attempt snakebite treatment based solely on this guide.
